Article Contents ::
- 1 Cardiac Arrest
- 2 Causes of cardiac arrest
- 3 Symptoms :
- 4 Features of Cardiac Arrest
- 5 Arrhythmias and circulatory failure
- 6 Management of Sudden cardiovascular collapse/ Cardiac arrest
- 7 5. Initial response and Basic Life Support (BLS)
- 8 2. Advanced Life Support (ALS) This includes:
- 9 a. Immediate defibrillation is done for VT VF with 200 – 360 J.
- 10 b. Prompt intubation, ventilation and arterial blood gas analysis is done.
- 11 c. An IV line is inserted and antiarrhythmic therapy started if defibrillation has failed (sinus rhythm is not restored).
- 12 IV Amiodarone
- 13 IV Procainamide
- 14 IV calcium gluconate
- 15 3. Post-resuscitation care
- 16 4. Long-term management
Cardiac Arrest
- Death is an irreversible cessation (stoppage) of all biologic functions.
- Cardiac arrest is an abrupt cessation of cardiac pump function which may be reversible by prompt intervention; otherwise it leads to certain death.
- Cardiac arrest is due to ventricular fibrillation in 80% of cases. Rest are due to bradyarrhythmias, asystole, pulseless electrical activity (PEA) and sustained ventricular tachycardia (VT).
- Sudden cardiac death (SCD) is a natural death due to cardiac·causes which leads to sudden loss of consciousness within one hour of acute symptoms, the time and mod~ of death are unexpected, although the patient mat have pre-existing heart disease.
- Cardiovascular collapse is a sudden loss of effective blood flow due to cardiac or vascular factors which may reverse spontaneously or with specific management.
- Cardiovascular collapse may be caused by vasovagal syncope, postural hypotension, severe bradycardia or cardiac arrest.
- Syncope reverses spontaneously but cardiac arrest requires intervention.
- The absence of effective mechanical cardiac activity
- This section is not a substitute for an AHA-approved Advanced Cardiac Life Support (ACLS) course and is intended only as a quick reference.
Causes of cardiac arrest
- Coronary artery disease – Acute coronary syndrome (ACS)
- MI (Myocardial infarction)
- IHSS (Idiopathic hypertrophic subaortic stenosis or hypertrophic cardiomyopathy)
- Dilated cardiomyopathy
- Myocarditis
- Right ventricular dysplasia (Brugada’s syndromethere is RBBB and sudden death)
- Valvular heart diseases
- WPW syndrome (Wolff Parkinson White syndrome)
- Conduction defects (Stokes Adams Syndrome-
- Syncope due to complete heart block)
- Acute heart failure
- Shock – Low cardiac output state
- Hypokalemia
- Hypoxaemia and acidosis
- Cardiac toxins
- Anaphylaxis.
Symptoms :
- Abrupt loss of consciousness, followed by death occurring within an hour of the onset of the illness (i.e., sudden death) is the typical presentation of cardiac arrest.
Features of Cardiac Arrest
- There are two major factors which lead to loss of effective circulation –
Arrhythmias and circulatory failure
- When arrhythmia is the terminal event, the duration of terminal illness is short.
- When the death is sudden, usually there is ventricular fibrillation.
- Heart rate usually increases and VPCs (ventricular premature contractions) develop, preceding cardiac arrest.
- Most cardiac arrests that are caused by VF (ventricular fibrillation) begin with a run of sustained or nonsustained VT (ventricular tachycardia).
- In circulatory failure there is gradual progression to death. In circulatory failure, death is due to cardiac asystole.
- In death due to cardiac causes there is no loss of consciousness usually till the end.
Management of Sudden cardiovascular collapse/ Cardiac arrest
- 1. Assess the initial response and give basic life support
- 2. Advanced life support
- 3. Post resuscitation care
- 4. Long term management.
5. Initial response and Basic Life Support (BLS)
- · Confirm whether there is cardiac arrest.
- · Check the state of consciousness, respiratory movements, skin color, carotid and femoral pulses.
- · In case a foreign body is obstructing the respiratory passage, a Heimlich maneuver is done to dislodge the obstruction.
- · For VT and VF a precordial blow or thump with the clenched fist is given on the lower third of sternum. [If defibrillator is available, immediate electrical defibrillation is done with 300-360 J energy].
- · The airway is cleared. Head is tilted back and chin lifted so that oropharynx can be explored to clear the airway.
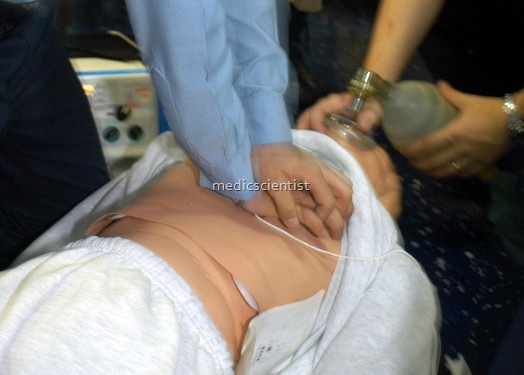
- · Mouth-to-mouth respiration or oropharyngeal airway, oesophageal obturators and masked Ambu bag is used to maintain ventilation.
- · Cardiac massage: For every 2 breaths given, 15 chest compressions are given. For chest compressions to maintain cardiac pump function, the palm of one hand is placed over the lower sternum with the other resting on the dorsum of the lower first hand.
- · The sternum of the patient is depressed without bending the arms of the resuscitator, at a rate qf about 100 per minute. The sternum is depressed about 4 cm with each compression.
2. Advanced Life Support (ALS) This includes:
- a. Defibrillation / Cardioversion / Pacing
- b. Intubation with an endotracheal tube
- c. Insertion of IV line ,It should be done in the above sequence only.
a. Immediate defibrillation is done for VT VF with 200 – 360 J.
- Epinephrine 1 mg IV is given if defibrillation fails, and then defibrillation repeated.
- Epinephrine is repeated every 5 minutes. Vasopressin 40 units IV single dose may be given instead of epinephrine.
b. Prompt intubation, ventilation and arterial blood gas analysis is done.
- Ventilation with oxygen reverses hypoxaemia and acidosis.
- NaHC03 – For acidotic patients 1 meq / kg of NaHC03 is given IV and half of this dose repeated every 15 minutes as required.
c. An IV line is inserted and antiarrhythmic therapy started if defibrillation has failed (sinus rhythm is not restored).
-
IV Amiodarone
150 mg in 10 minutes followed by 1 mg / min up to 6 hours and 0.5 mg/min thereafter is given.
- A bolus of 1 mg / kg of lidocaine is given IV, and the dose repeated in 2 minutes in patients of acute MI with cardiac arrest.
-
IV Procainamide
100 mg in 5 minutes up to 500 mg, followed by continuous infusion at 5 mg / min may be tried for persistent arrhythmias.
IV calcium gluconate
is given in patients of acute hyperkalemia in resistant VF with hypocalcemia, or in patients who have received toxic doses of calcium channel blockers.
- Cardiac arrest due to asystole is managed with epinephrine and atropine, IV or intracardiac. External pacing is done. Prognosis is poor.
- Pulseless electrical activity is treated with epinephrine, atropine and pacing.
3. Post-resuscitation care
- · In acute MI, if ventricular fibrillation occurs it responds to life support techniques easily.
- · VF which occurs after a certain period has passed after acute MI, resuscitation is less successful and recurrence rate is high.
- · In hemodynamically unstable patients, VF, bradyarrhythmias, asystole and PEA (Pulseless Electrical Activity) are common and have a bad prognosis.
- · Often anoxic encephalopathy develops and death occurs.
- · Inducing hypothermia can save these patients by reducing metabolic demands and cerebral edema.
- · Patients with cancer, renal failure, CNS disease, septicemia have a poor survival after cardiac arrest.
4. Long-term management
- Includes ICD (Intra Cardiac Device), detailed studies regarding underlyin
