Article Contents ::
- 1 Dialysis for Renal Failure
- 2 Indications for putting patients on dialysis are:
- 3 PERITONEAL DIALYSIS
- 4 Forms of peritoneal dialysis
- 5 HEMODIALYSIS
- 6 The Dialysis Circuit
- 7 Vascular access AV fistula
- 8 Venous catheters
- 9 Dialyzate circuits
- 10 Dialysis targets
- 11 Renal function is assessed by
- 12 Complications of Dialysis
- 13 RENAL TRANSPLANT
Dialysis for Renal Failure
Dialysis is a procedure for replacement of renal function to treat renal failure. Dialysis prolongs the life of ESRD (End Stage Renal Disease) patients. The leading causes of ESRD are diabetes mellitus, hypertension, glomerular nephritis, polycystic kidney disease and obstructive uropathy. patients with acute renal failure or acute kidney injury (AKI) is principally supportive, with renal replacement therapy (RRT) indicated in patients with severe kidney injury
Indications for putting patients on dialysis are:
- 1. Presence of uremic syndrome
- 2. Presence of hyperkalemia not responding to con-
- servative management
- 3. Bleeding, diathesis
- 4. Extracellular volume expansion
- 5. Acidosis not responding to medical management
- 6. Creatinine clearance of 10 ml/minute/1. 73 sq m body surface’ area.
- Refractory fluid overload Hyperkalemia (plasma potassium concentration >6.5 meq/L)
- or rapidly rising potassium levels Signs of uremia, such as pericarditis, neuropathy,
- or an otherwise unexplained decline in mental status Metabolic acidosis (pH less than 7.1)
PERITONEAL DIALYSIS
- 1 to 3 L of dextrose containing solution is infused into the peritoneal cavity and allowed to remain for 2 to 4 hours.
- Toxic materials are removed by convective clearance through ultrafiltration and diffusive clearance through concentration gradient.
- Water and solutes moves into peritoneal cavity and some of it may be absorbed from the peritoneal cavity.
- Access to peritoneal cavity is obtained through a peritoneal catheter placed in the peritoneal cavity through the skin.
Forms of peritoneal dialysis
1. CAPD – Continuous ambulatory peritoneal dialysis.
- Dialysis solution is infused into peritoneal cavity during the day and exchanged 3-4 times daily.
2. CCPD – Continuous cyclic peritoneal dialysis.
- In CCPD, exchanges are performed at night 4-5 times when the patient sleeps. In the morning the patient does his usual regular activities.
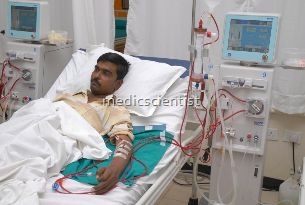
HEMODIALYSIS
- It is based on the principle of solute diffusion across a semi permeable membrane. Solutes are removed from the blood into dialyzate and excess water volume is removed from the patient by ultrafiltration.
The Dialysis Circuit
- Blood is withdrawn from the arterial side by the blood pump and pumped through the dialyzer back to the patient through venous segment.
Vascular access AV fistula
- An AV fistula is created in the patient’s arm.
- This is done when serum creatinine is more than 4 mg/dl and creatinine clearance is less than 25 ml / min., or when regular dialysis is needed.
- AV fistula is made between an artery and vein which are in close proximity like radiocephalic or brachiocephalic.
- The fistula can be used after 6 – 12 weeks of making.
Venous catheters
- Venous catheters can be placed in subclavian, jugular or femoral veins.
Dialyzate circuits
- The water and dialyzate are mixed by the machine and enters the dialyzer which consists of the dialyzer membrane of cellulose or semi cellulose.
- Anticoagulation is done during hemodialysis to prevent thrombosis in dialyzer and circuits.
Dialysis targets
- The blood flow rates are 300 – 500 ml/min. with dialyzate flow rates of 500 – 800 ml/min.
- The urea clearance is 200 – 350 ml/min.
- 9-12 hours of dialysis is required each week divided into 3 sessions.
- There should be a 65% reduction in predialysis and post dialysis blood urea nitrogen.
Renal function is assessed by
- Serum creatinine
- Blood urea nitrogen Creatinine and urea clearance
- Measurement of GFR (glomerular filtration rate) using radioisotope such as iodothalamate.
- In acute renal failure hemodialysis, continuous renal replacement therapies, and peritoneal dialysis may be done.
- In chronic renal failure or ESRD – hemodialysis, peritoneal dialysis – CAPD (continuous ambulatory peritoneal dialysis), or CCPD (continuous cyclic peritoneal dialysis), or renal transplant may be done.
- In younger patients, peritoneal dialysis is preferred. In older patients, obese patients with very poor renal function, hemodialysis is preferred.
Complications of Dialysis
- · Thrombosis of vascular access
- · Infections of fistula
- · Hypotension
- · Cramp;s
- · Dialysis disequilibrium syndrome – Nausea, vomiting,’ restlessness, headache, seizures, coma, arrhythmias
- · Hypoxia’,
- · Hypoglycemia
- · Haemorrhage
- · Pyrogenic reactions.
RENAL TRANSPLANT
- Renal transplant is the best treatment of advanced chronic renal failure.
- Transplantation results in improved lifestyle and improved life expectancy. It should be done in patients with end-stage renal disease without serious diabetes, coronary artery disease, AIDS, hepatitis B, hepatitis C, malignancy.
- Donors may be cadavers or living donors with HLA antigen compatibility and same major ABO blood group.
- The living donor kidney is removed and the organ is placed in inguinal fossa without entering the peritoneal cavity.
- The problems are acute irreversible rejection or chronic rejection. Hemodialysis is done within 48 hours of surgery, electrolytes and fluid balance are maintained.
- Immunosuppressive drugs like cyclosporine is started. Antibiotics may be needed for management of infections.
- Chronic renal transplant rejection may be caused by recurrent disease, hypertension, cyclosporine or tacrolimus (immunosuppressive), nephrotoxicity, chronic rejection, focal glomerulosclerosis etc.
