Article Contents ::
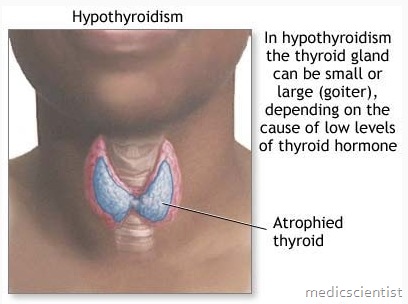
What is HYPOTHYROIDISM ?
- Hypothyroidism is a state of deficient function of the thyroid gland i.e. deficient secretion of thyroid hormones.
- In hypothyroidism normal thyroid hormone levels are maintained by a rise in TSH. This is called subclinical hypothyroidism.
- Later free T4 level falls and TSH levels rise further. This is the stage of clinical hypothyroidism when features of deficiency of thyroid hormones become manifest.
- Sub-clinical hypothyroidism is found in 10% of women over the age of 60 years.
Types of hypothyroidism
Primary hypothyroidism
- is a primary deficiency of thyroid hormones due to hyposecretion by the thyroid gland.
- A normal TSH level means that the patient cannot have primary hypothyroidism. In primary hypothyroidism i. e. disease of thyroid responsible for hypothyroidism, the TSH level rises. As a screening test TSH estimation is very good.
- T4 cannot be used as a screening test because it cannot detect sub clinical hypothyroidism (normal T4 with elevated TSH).
Secondary hypothyroidism
- is due to anterior pituitary hormone deficiencies.
- Isolated TSH deficiency is rare.
- TSH levels may be normal, low or slightly increased in secondary hypothyroidism. Free T4 is low.
Signs and Symptoms of HYPOTHYROIDISM
- History
- Arthralgias
- Carpal tunnel syndrome
- Cold intolerance
- Constipation
- Decreased memory, concentration
- Decreased sweating
- Depression
- Hearing impairment
- Hoarseness
- Menorrhagia
- Modest weight gain (10 lb [4.5 kg])
- Muscle cramps
- Onset may be insidious, subtle
- Paresthesias
- Weakness, fatigue, lethargy
- Physical Exam
- Bradycardia
- Coarsening or huskiness of voice
- Delayed relaxation of deep-tendon reflexes
- Dry, coarse skin
- Dull facial expression
- Hypothermia
- Increased diastolic BP
- Macroglossia
- Periorbital puffiness
- Reduced body and scalp hair
- Reduced systolic BP
- Swelling of hands and feet (nonpitting)
Causes of hypothyroidism:
- 1. Autoimmune hypothyroidism (Hashimoto’s thyroiditis)
- 2. Iodine deficiency
- 3. Amiodarone and lithium
- 4. Antithyroid drugs
- 5. Iodine excess
- 6. Congenital hypothyroidism
- 7. After thyroidectomy or irradiation
- 8. Thyroiditis
- 9. Hypopituitarism
- 10. Hypothalamic diseases.
Clinical Manifestations of Hypothyroidism
- · Tiredness and weakness
- · Dry skin
- · Feeling of cold
- · Hair loss
- · Difficulty in concentration and poor memory
- · Constipation, weight gain, poor appetite
| • | Hoarseness of voice |
| • | Dyspnoea |
| • | Menorrhagia |
| • | Paraesthesia |
| • | Deafness |
| • | Bradycardia |
| • | Edema – Non-pitting |
| • | Delayed tendon reflex |
| • | Carpal tunnel syndrome |
| • | Pleural effusion |
| • | Pericardial effusion. |
HYPOTHYROIDISM Associated Conditions
- Anemia
- Depression
- DM
- Down syndrome
- Hypercholesterolemia
- Hyponatremia
- Hypoparathyroidism
- Idiopathic adrenocorticoid deficiency
- Ischemic heart disease
- Metabolic syndrome
- Mitral valve prolapse
- Myasthenia gravis
- Rapid-cycling bipolar disorder
- Vitiligo
Lab diagnosis
- · TSH estimation (elevated)
- · T4 (Low)
- · TPO antibodies (thyroid peroxidase)
- · FNA (fine needle aspiration) biopsy
- · Elevated cholesterol and triglycerides
- · Anaemia.
Treatment of HYPOTHYROIDISM
- Levothyroxine 100 – 150 IJgjday.
- Lower doses may be given to patients of Grave’s disease who need replacement after treatment of hyperthyroidism.
- Dose is adjusted to keep the TSH levels in the lower range. TSH is measured 2 months after start of treatment.
- There is full relief after 3 – 6 months, after normal TSH levels are regained.
- Levothyroxine is increased in doses of 25 IJg only. Overtreatment with T4 (thyroxine) results in reduced bone density and atrial fibrillation.
- Once TSH levels are stable, then TSH may be measured annually only.
- T4 has a long half life of 7 days, therefore, any missed doses can be made up by taking 2-3 tablets at once.
- Pregnant women should be made euthyroid. Patients should be euthyroid before surgery. Elderly patients require less thyroxine.
