Article Contents ::
- 1 Leprosy (Hansen’s Disease) Causes, Symptoms, Signs, Diagnosis With Treatment
- 2 Leprosy is a chronic infective disease, also called Hansen’s disease.
- 3 Etiology:
- 4 Epidemiology Mycobacterium leprae:
- 5 Transmission Mycobacterium leprae
- 6 Clinical features Mycobacterium lepra —
- 7 TUBERCULOID LEPROSY Features are:
- 8 LEPROMATOUS LEPROSY
- 9 LEPRA REACTIONS
- 10 Type 1 lepra reaction —
- 11 Type 2 Lepra reaction —
- 12 LUCIO’S HENO ENON It is found in Mexico.
- 13 Complications of Leprosy Extremities–
- 14 Diagnosis Biopsy of skin:
- 15 Treatment lepromatous lepros
- 16 Treatment of ENL (erythema nodosum leprosum)
Leprosy (Hansen’s Disease) Causes, Symptoms, Signs, Diagnosis With Treatment
 |
| Leprosy(Hansen’s Disease) types Causes of leprosy sign and Symptoms |
Leprosy is a chronic infective disease, also called Hansen’s disease.
- It is caused by Mycobacterium leprae.
- Clinical manifestations are seen in skin, peripheral nervous system, upper respiratory tract, eyes, and testes.
- The main involvement is of the peripheral nerve from large trunks to small dermal nerves.
- The disease is transmitted from person to person.
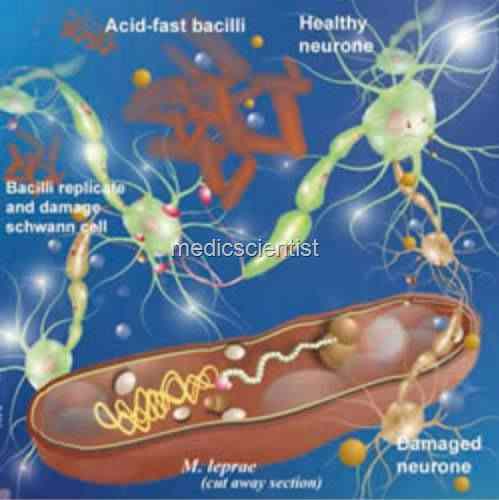 |
| Mycobacterium leprae M. lepra |
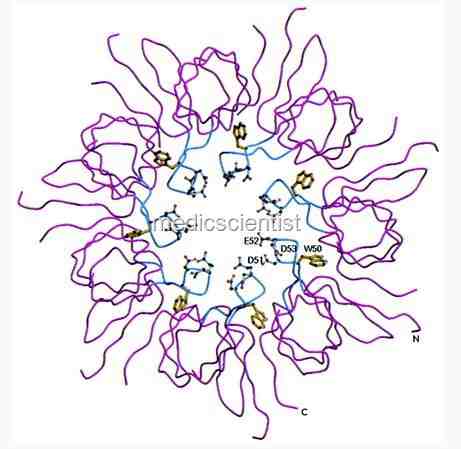 |
| M. lepra |
Etiology:
- M. leprae is an obligate intracellular bacillus.
- The bacteriologic index is a measure of infection with 4+ to 6+ denoting severe infection.
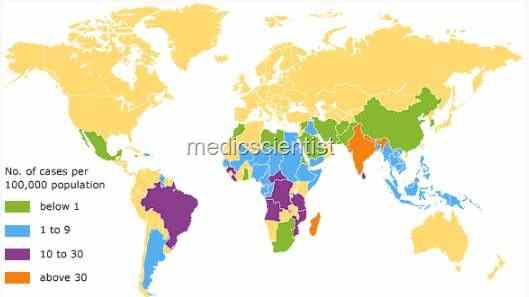 |
| Epidemiology Mycobacterium leprae |
Epidemiology Mycobacterium leprae:
- It is a disease of the developing nations.
- It is found in poor people, rural people and patients of AIDS.
- Common in second and third decades. s more common in f1lllP.
 |
| Transmission Epidemiology Mycobacterium lepra |
Transmission Mycobacterium leprae
- Nasal droplet infection
- Contact with infected soil
- Aerosol – like a sneeze
- Insect vectors
- Dermal inoculation like tattoo
- Intimate contact with infected person.
- Caring for a leprosy patient by nurse and doctors does not give them infection.
 |
| Clinical features Mycobacterium lepra |
 |
| Clinical features Mycobacterium lepra |
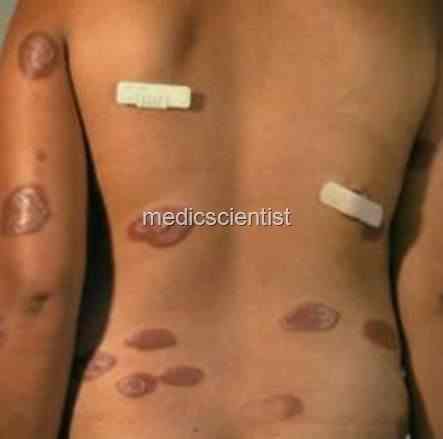
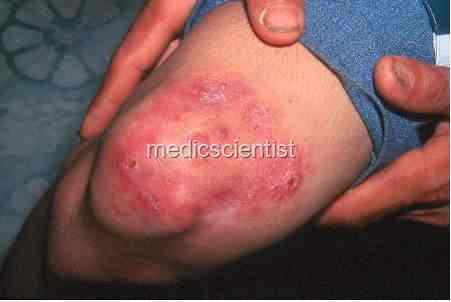
Clinical features Mycobacterium lepra —
- · Incubation period 2 – years.
- · The disease may be tuberculoid, borderline tuberculoid, mid borderline, borderline lepromatous and lepromatous leprosy.
- · This spectrum of presentation from tuberculoid to lepromatous is a change from asymmetric, localized macules and plaques to nodular, hard, symmetric and generalized skin lesions, an increasing bacterial load and decreasing immunity.
 |
| TUBERCULOID LEPROSYFeatures |
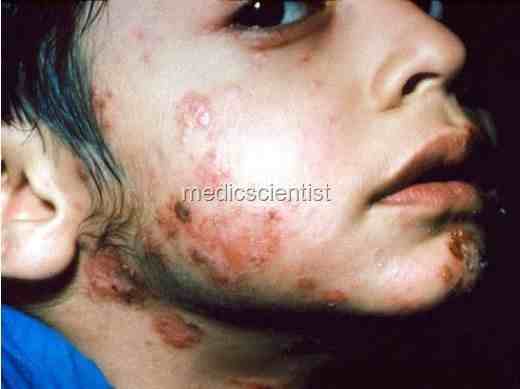
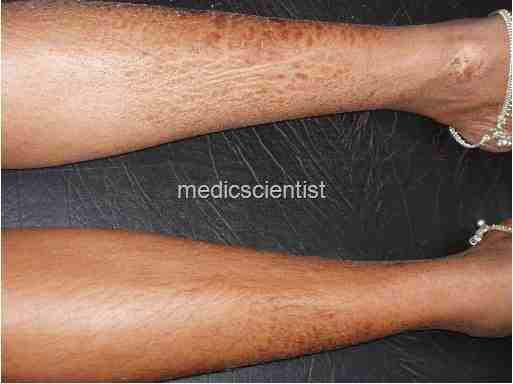
TUBERCULOID LEPROSY Features are:
- · Hypopigmented macules or plaques, sharply demarcated, red, hypoesthetic, dry, scaly and anhidrotic.
- · A few peripheral nerves show asymmetric enlargement like the ulnar, posterior auricular, peroneal, posterior tibial nerves.
- · It is the most common form of disease.
- · Lepromin skin test is positive.
 |
| LEPROMATOUS LEPROSY |
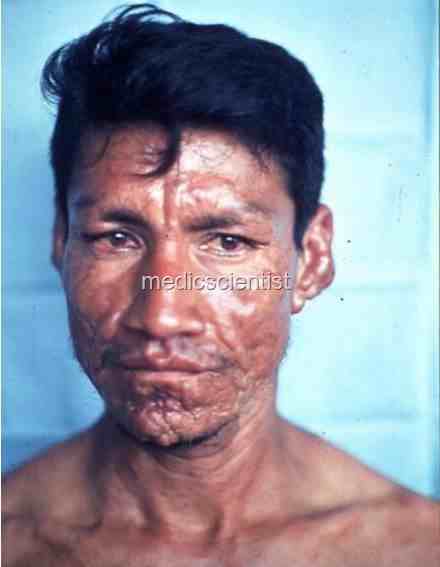
LEPROMATOUS LEPROSY
- There are symmetrical skin nodules, raised plaques, leonine faeces.
- Loss of eyebrows (specially lateral one-third), eyelashes. ~ry scaly skin._
- Leprabacilli are numerous on the skin and peripheral nerves.
- Nerve enlargement and damage is mmetrical. There is symmetrical peripheral neuropathy with nerve trunk enlargergment.
- Upper respiratory tract, anterior chamber of eye and testes are involved .
- Lepromin skin test is negative.
LEPRA REACTIONS
- Leprosy may present with lepra reactions.
- Lepra reactions may also occur after start of chemotherapy.
 |
| Type 1 leprareaction |
Type 1 lepra reaction —
- It is common in borderline cases.
- There are signs of inflammation over skin lesions. There is neuritis, low grade fever.
- The ulnar nerve is very painful.
- Nerve damage resulting in foot-drop may occur. Down grading reactions are lepra reactions before start of antimicrobial therapy.
- Reversal reactions are leprareaction after start of therapy.
 |
| Type 2Lepra reaction |
Type 2 Lepra reaction —
- It is also called erythema nodosum leproticum. It occurs within 2 years of start of therapy. There are painful red papules, malaise, high fever, neuritis, uveitis, lymphadenitis, orchitis, glomerulonephritis.
- It may end in death.
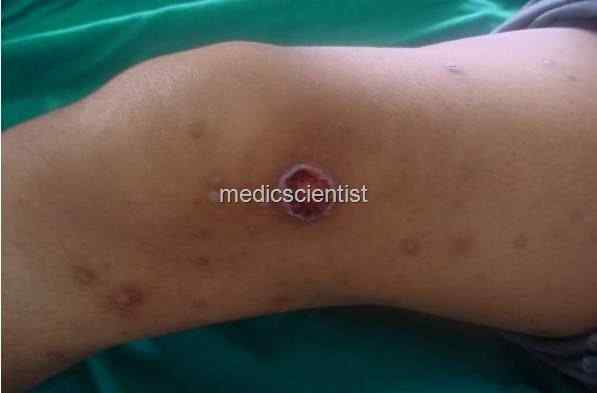
LUCIO’S HENO ENON It is found in Mexico.
- It is seen in diffuse lepromatous leprosy.
- There are large ulcerated lesions on lower extremities.
 |
| Complications ofLeprosyExtremities |
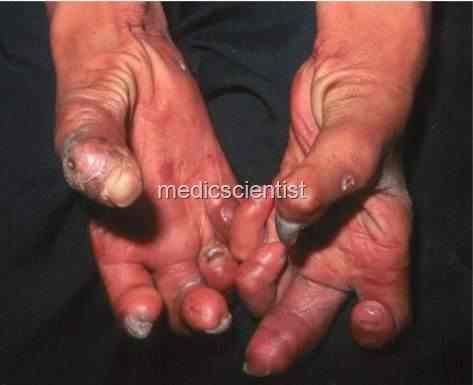
Complications of Leprosy Extremities–
- There is loss of fine touch, pain and heat sensation but position and vibration is spared.
- There is clawing of hands due to ulnar and median nerve damage.
- There is foot drop due to peroneal nerve palsy. There may be ulcers on the hands and feet.
- Fingers and toes are lost due to osteolytic process and injury.
Nose:
- · Chronic nasal congestion
- · Epistaxis
- ·Destruction of nasal cartilage with saddle-nose deformity and anosmia
Eye:
- · Corneal insensitivity
- · Uveitis
- · Cataract
- · Glaucoma
- ·Blindness
Testes:
- · Orchitis
- · Aspermia
- · Impotence
Amyloidosis:
- · Secondary amyloidosis affecting liver and kidney
Nerves:
- • Abscess
 |
| Diagnosis lepromatous leprosy Biopsyofskin |
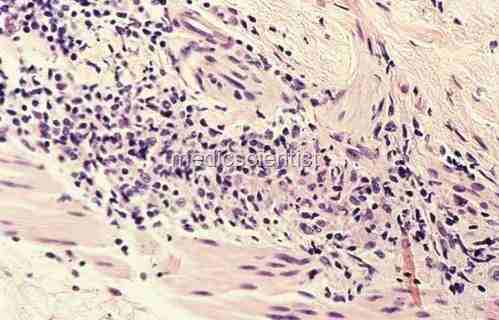
Diagnosis Biopsy of skin:
- In lepromatous leprosy even normal skin will show the bacilli.
- In tuberculoid leprosy biopsy must be taken from the lesion.
- Scraping the skin and examining under the microscope may show the bacilli.
IgM antibodies
- PGL 1 (phenolic glycolipid) are found in untreated patients.
Treatment lepromatous lepros
- Tuberculoid leprosy – Dapsone 100 mg/day for 5 years.
- Lepromatous leprosy – Rifampin 600 mg/day for 3 years + Dapsone 100 mg /day for a long time.
- Treatment of reactions – Glucocorticoids Prednisone 40-60 mg/day gradually tapered and continued for 3 months.
- Clofazimine 200 to 300 mg/d is less efficacious than steroids.
Treatment of ENL (erythema nodosum leprosum)
- – Glucocorticoids.
Prevention lepromatous lepros
- · Vaccination at birth with BCG.
- · Dapsone reduces incidence of tuberculoid leprosy.
