Article Contents ::
Mediastinal Diseases
- The mediastinum is the region between the two pleural sacs i.e. the central portion of thorax.
- It is separated into 3 compartments.
-
Anterior mediastinum
- contains the thymus, lymph nodes, internal mammary arteries and veins.
- The anterior compartment (also referred to as the anterosuperior compartment or retrosternal space) is anterior to the pericardium and includes the thymus, the extrapericardial aorta and its branches, the great veins, and lymphatic tissue.
-
Middle mediastinum
- contains the heart, the ascending and transverse arches of the aorta, vena cavae, the bracheocephalic arteries and veins, the phrenic nerves, the trachea, the main bronchi, lymph nodes, pulmonary arteries and veins.
- The middle compartment is bounded by the pericardium anteriorly, the posterior pericardial reflection, the diaphragm, and the thoracic inlet.
-
Posterior mediastinum
- contains descending v thoracic aorta, oesophagus, thoracic duct, azygos and hemiazygos veins, lymph nodes.
- The posterior compartment extends from the posterior pericardial reflection to the posterior border of the vertebral bodies and from the first rib to the diaphragm
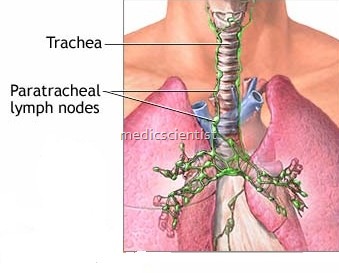
Mediastinal masses
- · Thymomas
- · Lymphomas
- · Neoplasms
- · Thyroid masses
- · Vascular masses
- · Granulomatous diseases
- · Cysts – bronchogenic and pleuro-pericardial
- · Neurogenic tumors
- · Meningoceles
- · Esophageal diverticula.
SIGNS AND SYMPTOMS —
- Most mediastinal tumors in adults are either asymptomatic (found on plain chest radiographs or computed tomographic (CT) scans
- Phrenic nerve damage can present with an elevated hemidiaphragm.
- Airway compression can lead to recurrent pulmonary infection and/or hemoptysis.
- Hoarseness can occur due to recurrent laryngeal nerve involvement.
- Esophageal compression can cause dysphagia. Involvement of the spinal column can result in paralysis.
- Horner’s and superior vena cava syndromes arise due to sympathetic ganglion and superior vena caval involvement, respectively
RADIOLOGIC EVALUATION —
- The evaluation of a newly diagnosed mediastinal mass is directed by its anatomic location and by patient age.
- The PA and lateral chest radiographs Small masses that were initially overlooked may be visible retrospectively,
- Mediastinal masses are diagnosed by CT scan, barium studies, nuclear scans, FNAC, mediastinoscopy.
- The CT scan can help define the anatomic location of the mass, determine its morphology and attenuation coefficient (cystic, fatty, enhancement characteristics, and soft tissue),
- Acute and Chronic mediastinitis
- Causes of mediastinitis are esopha eal erforation, tu erculosis, sarcoidosis, fungal diseases.
- Pneumomediastinum
- There is gas in the interstices of the mediastinu.m.
Causes of Mediastinal Diseases are:
- 1. Alveolar rupture.
- 2. Rupture of oesophagus, trachea, bronchi.
- 3. Dissection of air from neck or abdomen.
Clinical features of Mediastinal Diseases :
- There is substernal chest pain, subcutaneous emphysema in the suprasternal notch,
- Hamman’s sign (crunching noise, heard with the heart beat, in the left lateral position).
- Mediastinal Diseases Chest X-ray: confirms the diagnosis.
Treatment of Mediastinal Diseases :
- Oxygen inhalation and needle aspiration, if required.
- Usually no treatment is required.
- But directed by the specific or likely diagnosis obtained through the history, physical examination, radiologic studies, and other diagnostic tests.
- Exploration and resection through a limited or full median sternotomy or thoracotomy (eg, resection of teratoma and thymic masses).
- Resection via minimally invasive video-assisted (VATS) procedures (may be appropriate for bronchogenic, esophageal duplication cysts or localized neurogenic tumors)
