Article Contents ::
- 1 Pulmonary Thromboembolism
- 2 Predisposing factors
- 3 Genetic Factors
- 4 Pathophysiology of Pulmonary Thromboembolism
- 5 Pulmonary Thromboembolism EPIDEMIOLOGY —
- 6 Pulmonary Thromboembolism Clinical Features
- 7 Pulmonary Thromboembolism Symptoms and signs are
- 8 Diagnosis of Pulmonary Thromboembolism
- 9 Blood test:
- 10 ECG:
- 11 Chest X-ray:
- 12 Venous Doppler
- 13 Chest CT :
- 14 Lung scan:
- 15 MRI :
- 16 Echocardiography :
- 17 Treatment of Pulmonary Thromboembolism
- 18 Anticoagulation with heparin and warfarin preventing pulmonary embolism
- 19 Prevention of Pulmonary Thromboembolism
Pulmonary Thromboembolism
Pulmonary thromboembolism means the embolization and lodgment of thombi in the pulmonary vasculature.
Predisposing factors
- PE refers to obstruction of the pulmonary artery or one of its branches by material (eg, thrombus, tumor, air, or fat ) that originated elsewhere in the body.
- Acute pulmonary embolism (PE) is a common and often fatal disease.
- Unfortunately, the clinical presentation of PE is variable and nonspecific, making accurate diagnosis difficult.
- Mortality can be reduced by prompt diagnosis and therapy.
- Air travel
- preventing pulmonary embolism
- obesity
- Cigarette smoking Oral contraceptives Pregnancy
- Surgery
- Traum
- Antiphospholipid antibody syndrome
- Cancer ‘.
- Systemic
- hypertension
- COPD.
Genetic Factors
- Autosomal dominant gene mutation – factor V Leiden and Prothrombin.
Pathophysiology of Pulmonary Thromboembolism
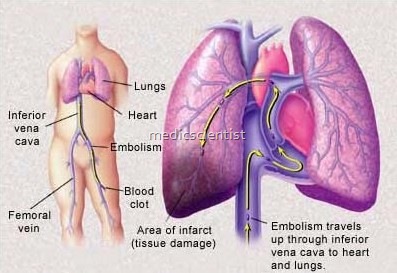
- Venous thrombi from pelvic and deep leg veins embolize to pulmonary arterial circulation or through patent foramen ovale j ASD to arterial circulation.
- There is increased pulmonary vascular resistance, impaired gas exchange, alveolar hyperventilation, decreased pulmonary compliance.
- Most PE arise from thrombi in the deep venous system of the lower extremities.
- There is right heart failure, decreased LV output, coronary artery hypoperfusion, circulatory collapse and death.
- However, they may also originate in the right heart or the pelvic, renal, or upper extremity veins.
Pulmonary Thromboembolism EPIDEMIOLOGY —
- This study certainly underestimates the true incidence and prevalence of PE, since more than half of all PE are probably undiagnosed.
- preventing pulmonary embolism
- peripheral pulmonary stenosis, pulmonary toilet
- PE was the presumed cause of death in approximately 200,000.
- In a study of more than 42 million deaths that occurred over a 20-year duration, almost 600,000 patients (approximately 1.5 percent) were diagnosed with PE .
Pulmonary Thromboembolism Clinical Features
- Embolism may be thrombus, fat embolism, tumor embolism, air embolism, IV drug user substance embolism, amniotic fluid embolism.
- RISK FACTORS —
- pulmonary toilet
- While much of the data related to risk factors are from patients with DVT, a few studies have looked specifically at patients with acute PE
- PE is a common complication of deep vein thrombosis (DVT), occurring in more than 50 percent of cases with phlebographically confirmed DVT
Pulmonary Thromboembolism Symptoms and signs are
- Dyspnoea Tachypnoea Syncope
- peripheral pulmonary stenosis
- Cyanosis
- Pleuritic pain
- Cough
- Hemoptysis
- Fever
- Chest pain
- Angina pectoris
- Hypotension
- Tachycardia
- Distended neck veins
- Loud P, (loud pulmonary component of second heart sound)
- RV failure.
- Massive PE may be accompanied by acute right ventricular failure, manifested by increased jugular venous pressure,
- The most common symptoms were dyspnea at rest or with exertion
- Circulatory collapse was uncommon
- Symptoms or signs of lower extremity deep venous thrombosis (DVT) were common
Diagnosis of Pulmonary Thromboembolism
-
Blood test:
- Plasma D-dimer enzyme linked immuno sorbent assay (ELISA) level is increased more than 500ngjml.
-
ECG:
- shows sinus tachycardia, AF(atrial fibrillation), S in lead 1, Q in lead 3, inverted T in lead 3.
-
Chest X-ray:
- is normal. There may be focal oligemia (decreased blood supply) called Westermark’s sign, wedge-shaped obesity called Hampton’s Hump, enlarged right descending pulmonary artery called Palla’s sign.
-
Venous Doppler
- shows DVT – Deep vein thrombosis.
-
Chest CT :
- Large central PE (pulmonary embolism) seen.
- Multislice scanners can show pulmonary blood vessels obstruction.
-
Lung scan:
- Albuminlabeled radionuclide shows pulmonary capillary blood flow and perfusion defects.
-
MRI :
- MR pulmonary angiography using gadolinium
- . is non-nephrotoxic, safe, and shows organic as well as functional lung disease.
-
Echocardiography :
- evidence of MI, cardiac tam~ ponade, RV dyskinesia, RVF seen.
- Pulmonary angiography: may not be required.
Treatment of Pulmonary Thromboembolism
- Thrombolysis Embolectomy
- preventing pulmonary embolism
- pulmonary catheter
- Anticoagulation with heparin, warfarin Secondary prevention of embolization by inferior vena cava filters NSAIDs
- Dobutamine for positive inotropic support and pulmonary vasodilatation
- Volume loading
- Low molecular weight heparin.
-
Anticoagulation with heparin and warfarin preventing pulmonary embolism
- Heparin is given along with warfarin for 5 days.
- preventing pulmonary embolism
- Dose of heparin is 5-10,000 units IV bolus followed by 1,000 units/hour.
- Dose of warfarin is 5 mg dail ad’usted accordin -.10 I R.
- Then he arin discontinued after 5 days and warfarin continued for 6 months to maintain INR of 1.5-3.
-
Prevention of Pulmonary Thromboembolism
- preventing pulmonary embolism
- Graduated compression stockings.
- Pneumatic compression devices .
- prophylaxis with anticoagulants in confined patients.
