Article Contents ::
- 1 Respiratory Failure
- 2 Respiratory failure means:
- 3 Hypoxemic
- 4 Hypercarbic
- 5 Respiratory failure may be acute or chronic.
- 6 Four different types of respiratory failure can be present:
- 7 Causes of respiratory failure:
- 8 Nervous system
- 9 Muscles of respiration
- 10 Airways
- 11 Alveolar system
- 12 Vasculature
- 13 Clinical Features of respiratory failure
- 14 Nervous system
- 15 Muscular dysfunction
- 16 Airway dysfunction
- 17 Alveolar disease
- 18 Pulmonary vascular disease
- 19 Management of Respiratory Failure
- 20 Triggering —
- 21 Auto-PEEP —
Respiratory Failure
- Respiratory failure is defined as inadequate gas exchange due to malfunction of one or more components of the respiratory system.
Respiratory failure means:
- Hypoxaemia – P02 <60 mmHg, or y Hypercarbia – PC02 >45 mmHg.
- So, respiratory failure may be hypoxaemic, hypercarbic or combined.
-
Hypoxemic
- respiratory failure is defined by arterial O2 saturation <90% while receiving an inspired O2 fraction >0.6.
- Acute hypoxemic respiratory failure can result from pneumonia, pulmonary edema (cardiogenic or noncardiogenic), and alveolar hemorrhage. Hypoxemia results from ventilation-perfusion mismatch and intrapulmonary shunting.
-
Hypercarbic
- respiratory failure is characterized by respiratory acidosis with pH <7.30. Hypercarbic respiratory failure results from decreased minute ventilation and/or increased physiologic dead space.
Respiratory failure may be acute or chronic.
- Acute respiratory failure is sudden and life-threatening.
- Chronic respiratory failure occurs gradually and compensation and adaptations in various organ systems occur ..
- Respiratory insufficiency means that there is a compensated state in a patient with respiratory disease and impaired function.
Four different types of respiratory failure can be present:
- Type I:
- There is acute hypoxemic respiratory failure. d” There is alveolar congestion.
- Ex. Pulmonary oedema, pneumonia, lung injury,
- Type II —
- there is hypercarbia
- it is seen in bronchial asthma, pneumothorex, drug overdose,
- brain stem injury,hypothyroidism,
- sleep disorders, myasthenia gravis,
- GB syndrome, myopathy etc.
- Type III :
- This is due to lung collapse.
- It is also called perioperative respiratory failure.
- Type IV:
- This occurs in shock due to hypoperfusion of respiratory muscles.
aOpen lung ventilation (OLV) involves the use of any of these specific modes with tidal volumes (or applied pressures) to achieve 5—6 mL/kg, and positive end-expiratory pressures achieve maximal alveolar recruitment. b FIo2 is usually set to 1.0 initially, unless there is a specific clinical indication to minimize FIo2, such as history of chemotherapy with bleomycin. Once adequate oxygenation is documented by blood gas analysis, FIo2 should be decreased in decrements of 0.1—0.2 as tolerated, until the lowest FIo2 required for an Sao2 >90% is achieved. Abbreviations: f, frequency; I/E, inspiration/expiration; FIo2, inspired O2; PEEP, positive end-expiratory pressure; for ventilator modes, see text; Vt, tidal ventilation.
| Ventilator Mode | Independent Variables (Set by User) | Dependent Variables (Monitored by User) | Trigger/Cycle Limit | Advantages | Disadvantages | Initial Settings |
| ACMVa | FIO2 Tidal volume Ventilator rate Level of PEEP Inspiratory flow pattern Peak inspiratory flow Pressure limit | Peak airway pressure, PaO2, PaCO2 Mean airway pressure I/E ratio | Patient/timer Pressure limit | Timer backup Patient-vent synchrony Patient controls minute ventilation | Not useful for weaning Potential for dangerous respiratory alkalosis | FIO2 = 1.0b Vt = 10–15 mL/kga f = 12–15/min PEEP = 0–5 cmH2O Inspiratory flow = 60 L/min |
| SIMVa | Same as for ACMV | Same as for ACMV | Same as for ACMV | Timer backup useful for weaning | Potential dyssynchrony | Same as for ACMVa |
| PCVa | FIO2 Inspiratory pressure level Ventilator rate Level of PEEP Pressure limit I/E ratio | Tidal volume Flow rate, pattern Minute ventilation PaO2, PaCO2 | Timer/patient Timer/pressure limit | System pressures regulated Useful for barotrauma treatment Timer backup | Requires heavy sedation Not useful for weaning | FIO2 = 1.0b PC = 20–40 cmH2Oa PEEP = 5–10 cmH2O f = 12–15/min I/E = 0.7/1–4/1 |
| PSV | FIO2 Inspiratory pressure level PEEP Pressure limit | Same as for PCV + I/E ratio | Inspiratory flow Pressure limit | Assures synchrony Good for weaning | No timer backup | FIO2 = 0.5–1.0b PS = 10–30 cmH2O 5 cmH2O usually the level used PEEP = 0–5 cmH2O |
Causes of respiratory failure:
-
Nervous system
- The medulla and its neural pathways control respiration. Dysfunction of this pathway results in central apnoea.
-
Muscles of respiration
- The dia hr m, the intercostal muscles, suprasternal, sternoCleidomastoid and other small muscles are responsible for the motor part ‘Of respiration. Muscle paralysis results in respiratory failure.
-
Airways
- If there is obstruction of air passages – ~ airways, bronchi or alveoli, then due to airway system sfunction, there can be respiratory failure.
-
Alveolar system
- In colla se of lung, congestion, injury, there is alveolar system dysfunction. –
-
Vasculature
- The pulmonary vasculature, if diseased, can lead to respiratory failure.
Clinical Features of respiratory failure
- Upper airway should be checked. There may be central or peripheral ganosis. Respirator .related deth and pattern of respiration ma be altered.
- There may be flarin of nostrils ursed li s use of accessory muscles of respiration.
- Oxygen and CO2 in arterial blood is estimated by arterial blood gas analysis. Pulse oximetry is done.
- To assess which part of the respiratory system is responsible for the respiratory failure, the folloWing table is useful:
Nervous system
- Respiratory rate is < 12jmin., with hypoxia,hypercarbia and acidemia.
Muscular dysfunction
- The vital capacity is < 10 ml/kg and inspiratory force is < -20 cm H20.
- There is presence of paradoxical respiratory motion.
Airway dysfunction
- There is wheezing or ronchi and raw airway re~istance > 10 cm H20/ L /sec.
Alveolar disease
- There is consolidation of lungs. PaC02 is elevated. Chest x-ray shows infiltrates.
Pulmonary vascular disease
- JVP is raised. ECG shows RVH with strain p~t- tern or RBBB.
Management of Respiratory Failure
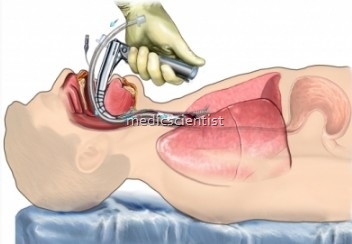
- General care of mechanically ventilated pts is reviewed along with weaning from mechanical ventilation. A cuffed endotracheal tube is often used to provide positive pressure ventilation with conditioned gas
- Airway protection, oxygenation, and ventilation is provided.
- Supplemental oxygen is given.
- Noninvasive positive pressure ventilation (NPPV) refers to positive pressure ventilation delivered through a noninvasive interface (nasal mask, facemask, or nasal plugs), rather than an invasive interface (endotracheal tube, tracheostomy).
- Airway is opened with head tilt – chin lift maneuver, foreign body removed.
- After an endotracheal tube has been in place for an extended period of time, tracheostomy should be considered, primarily to improve pt comfort and management of respiratory secretions.
- Suction is done for vomit or blood. Tracheostomy may be required.
- Adequate oxygenation – 100% oxygen is given. Artificial ventilation/Mechanical ventilation, if required, is started.
- Endotracheal intubation may be done for mechanical ventilation.
- PEEP is given in patients with mechanical ventilation.
- In some circumstances, noninvasive positive pressure ventilation (NPPV) delivered through a tightly fitting nasal or full facemask should be considered for treatment of impending respiratory failure
- Cause of respiratory failure assessed. Treat infections.
- Anti-inflammatory or immuno-suppressive drugs are given.
- Bronchodilators.
- Anticoagulants or thrombolytics. Diuretics.
Triggering —
- Ventilators can be triggered by a change in alveolar pressure (ie, pressure triggered) or flow (ie, flow triggered)
- The trigger sensitivity is usually set at -1 to -2 cmH2O when pressure triggering is used.
- The trigger sensitivity is usually set at 2 L/min when flow triggering is used.
Auto-PEEP —
- Intrinsic positive end-expiratory pressure (ie, intrinsic PEEP or auto-PEEP) can be measured in a relaxed patient by occluding the expiratory port of the ventilator circuit
