Article Contents ::
- 1 Treatment of Pneumonia ,INDICATIONS FOR HOSPITALIZATION in Pneumonia ,Resistant Pneumonia
- 2 Risk factors for drug Resistant Pneumonia —
- 3 INDICATIONS FOR HOSPITALIZATION in Pneumonia —
- 4 No comorbidities or recent antibiotic use —
- 5 Comorbidities or recent antibiotic use —
- 6 Antibiotic Therapy for Pneumonia
- 7 For pseudomonas infection:
- 8 For aspiration pneumonia:
- 9 Duration of Antibiotic treatment:
- 10 ASPIRATION PNEUMONIA
- 11 Clinical features of Aspiration pneumonia
- 12 HOSPITAL ACQUIRED PNEUMONIA
- 13 Etiopathogenesis of Pneumonia
- 14 Clinical manifestations of nosocomial infections
- 15 Diagnosis
- 16 Treatment
- 17 Clinical features Pneumonia
Treatment of Pneumonia ,INDICATIONS FOR HOSPITALIZATION in Pneumonia ,Resistant Pneumonia
defined as an acute infection of the pulmonary parenchyma in a patient who has acquired the infection in the community, as distinguished from hospital-acquired (nosocomial) pneumonia, No comorbidities or recent antibiotic use and Comorbidities or recent antibiotic use Treatment according the condition.
- The diagnostic approach to patients with CAP
- Assess severity
- Oxygen therapy
- Circulatory support –
- Etiological detection
- Rule out tuberculosis
- Rule out pulmonary embolism
- Treat co-existent diseases
- Prevent aspiration
- Send investigations
- Chest x-ray and CT scan.
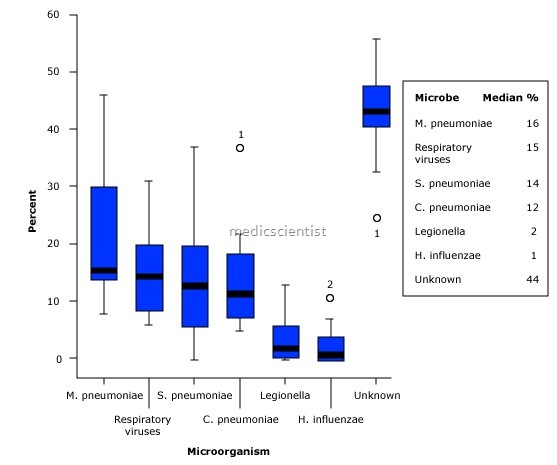
Risk factors for drug Resistant Pneumonia —
- Risk factors for and other issues related to drug resistance in patients with CAP are discussed in detail elsewhere.
- Summarized briefly,
- risk factors for drug-resistant
- S. pneumoniae in adults include: Age >65 years
- Beta-lactam, macrolide, or fluoroquinolone therapy within the past three to six months
- Alcoholism Medical comorbidities Immunosuppressive illness or therapy Exposure to a child in a day care center
- Recent therapy or a repeated course of therapy with beta-lactams, macrolides, or fluoroquinolones is a risk factor for pneumococcal resistance to the same class of antibiotic.
INDICATIONS FOR HOSPITALIZATION in Pneumonia —
- CURB-65 uses five prognostic variables :
- Confusion (based upon a specific mental test or disorientation to person, place, or time)
- Urea (blood urea nitrogen in the United States) >7 mmol/L (20 mg/dL)
- Respiratory rate >30 breaths/minute
- Blood pressure [BP] (systolic <90 mmHg or diastolic <60 mmHg)
- Age >65 years
- The authors of the original CURB-65 report suggested that patients with a CURB-65 score of 0 to 1,
- Those with a score of 2 should be admitted to the hospital, and those with a score of 3 or more should be assessed for ICU care, particularly if the score was 4 or 5.
No comorbidities or recent antibiotic use —
- For uncomplicated pneumonia in patients who do not require hospitalization, have no significant comorbidities and/or use of antibiotics within the last three months,
- Azithromycin
- (500 mg on day one followed by four days of 250 mg a day); 500 mg a day for three days, or 2 g single dose (microsphere formulation) are acceptable alternative regimens
- Clarithromycin
- XL (two 500 mg tablets once daily) for five days or until afebrile for 48 to 72 hours
- Doxycycline
- (100 mg twice a day) for seven to 10 days
Comorbidities or recent antibiotic use —
- The presence of significant comorbidities (ie, chronic obstructive pulmonary disease [COPD], liver or renal disease, cancer, diabetes, chronic heart disease, alcoholism, asplenia, or immunosuppression), and/or use of antibiotics within the prior three months, increases the risk of infection with more resistant pathogens.
- Combination therapy with a beta-lactam effective against S. pneumoniae (high-dose amoxicillin, 1 g three times daily or amoxicillin-clavulanate 2 g twice daily
- or cefpodoxime 200 mg twice daily
- or cefuroxime 500 mg twice daily) PLUS either a macrolide (azithromycin 500 mg on day one followed by four days of 250 mg a day
- or clarithromycin 250 mg twice daily or clarithromycin XL 1000 mg once daily) or doxycycline (100 mg twice daily).
- A respiratory fluoroquinolone (gemifloxacin 320 mg daily, levofloxacin 750 mg daily, or moxifloxacin 400 mg daily) for a minimum of five days.
- Treatment should be continued for a minimum of five days.
Antibiotic Therapy for Pneumonia
- Macrolide plus second generation or third generation cephalosporin.
- Clarithromycin 500 mg bd x 10 days.
- Azithromycin 500 mg once than 250 mg od for 4 days.
- Doxycycline 100 mg bd for 10 days.
- Fluoroguinolone-
- Levofloxacin500 mg od,
- Moxifloxacin 400 mg od,
- Gatifloxacin 400 mg od, for DRSP infection (Drug resistent Strepto pneumoniae)
- Cefpodoxime- 200 mg bd
- Cefuroxime axe 750 mg tid IV
- Ceftriaxone – 1 g 12 hourly IV
- Cefotaxime – 2 g 6 hourly IV
- Amoxicillin + Clavulanic acid + Macrolide – 875/ 125mg tid
- Ceftriaxone 1 g IV 12 hourly + AZithromycin 1 g IV then 500 mg after 24 hours
- Cefotaxime + AZithromycin
- Ampicillin + Sulbactam + Azrithromycin.
For pseudomonas infection:
- Imipenem 500 mg 6 hourly IV I Meropenem
- Piperacillin / Tazobactam 3.375 gm. 6 hourly IV + Ciprofloxacin 500 mg bd IV.
For aspiration pneumonia:
- Metronidazole + Levofloxacin or Gatifloxacin
- For concomitant meningitis – Vancomycin 1 g 12 hourly IV + Ceftriaxone
- For methicillin-resistant Staph. Aureus – use Vancomycin or Linezolid.
- Antibiotics are given intravenously. Oral antibiotics are started when:
- 1. WBC cpunt is normal.
- 2. There are two readings of normal temperature in 24 hours.
- 3. There is improvement in cough and shortness of breath is elieved.
Duration of Antibiotic treatment:
- Antibiotics are given for 10 – 14 days. Azithromycin is given for 5 days.
ASPIRATION PNEUMONIA
- Aspiration pneumonia is due to foreign objects or substances entering the lower respiratory tract.
- In the supine position the most prone areas are the posterior segments of the upper lobes and the superior segments of the lower lobes.
- Common in the elderly
- Organisms responsible are Enterobacter, S. aureus, S. pneumonae, H influenzae.
- In aspiration pneumonia, gastric contents or oropharyngeal flora are aspirated into the lungs resulting in inflammatory response and bacterial infection.
- Aspiration is common in unconscious patients, neuromuscular diseases.
Clinical features of Aspiration pneumonia
- Gastric acid aspiration results in chemical pneumonitis.
- There is dyspnoea, tachypnoea, bronchospasm, cyanosis, diffuse opacities in lung x-ray.
- Lung abscess is a common complication of aspiration pneumonia.
HOSPITAL ACQUIRED PNEUMONIA
- HAP is defined as pneumonia occurring 48 hours after hospital admission by a new pathogen.
- It has a high morbidity and mortality.
- It occurs in 5 – 10% of patients admitted to medical and surgical wards.
- Incidence is highest in ICU in patients on mechanical ventilation. Patients of ventilator acquired pneumonia (VAP) develop the disease in 4 days of intubation.
Etiopathogenesis of Pneumonia
- Endotracheal intubation, enteral feedings, shock, coma, systemic inflammatory response syndrome, suctioning, lack of cough reflex, nasogastric tube, ·use of H2antagonists, tracheobronchitis, all promote HAP.
- Organisms are Pseudomonas, Acinetobacter, Klebsiella, Enterobacter, and Staph aureus.
- Methicillin-resistant Staph. aureus (MRSA) is a common cause of nosocomial infection.
- Nosocomial infections are due to resistant bacteria because of recent antibiotic therapy, glucocorticoids, malnutrition, mechanical ventilation, neurosurgery, head trauma, ARDS, aspiration, tracheostomy, lung contusion, prolonged ICU stay.
Clinical manifestations of nosocomial infections
- New or enlarging infiltrates on chest X-ray plus fever, leucocytosis, purulent sputum, dyspnoea, hypoxemia, pleuritic chest pain with demonstration of bacteria by smear or culture are important features of HAP.
Diagnosis
- By BAL (broncho alveolar lavage), and FOB (fiberoptic bronchoscopy) .
Treatment
- Vancomycin Linezolid.
Clinical features Pneumonia
- There is recurrent cough and foul-smelling,
- ARTAGENER’S SYNDROME rulent sputum.
- Hemoptysis may occur.
- Dyspnoea with wheezing and Fever.
