Mitral Regurgitation (MR) Causes, Mitral Regurgitation (MR) Symptoms ,ACC/AHA guideline for Mitral Regurgitation (MR) Physical findings Treatment of Mitral Regurgitation
Mitral regurgitation is the regurgitation or back flow of blood from left ventricle to left atrium during left venticular systole. It is also called Mitral incompetence. A backward flowing, as in the return of solids or fluids to the mouth from the stomach or the backflow of blood through a defective heart valve.
- Chronic mitral regurgitation (MR) is a relatively common valvular disorder that can progress to ventricular decompensation and the need for mitral valve surgery.
- Commonest cause of MR (Mitral Regurgitation) is chronic rheumatic heart disease.
- MR may also occur due to congenital malformation, IHD, MI leading to papillary muscle dysfunction, LV dilatation, calcification of the mitral valve, infective endocarditis, MVP (mitral valve prolapse).
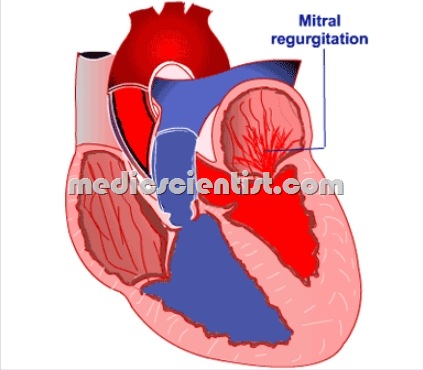
Mitral Regurgitation (MR) Pathophysiology
- Due to mitral regurgitation, some volume of blood From LV goes into LA resulting in LA enlargement.
- ue to this extra volume of blood coming from LA to V in the next diastole the volume of LV increases.
- Gradually LV volume and pressure increase. There”ore, there is dilatation of mitral valve ring resulting further incompetence of the mitral valve.
Acute MR —
- There are two major hemodynamic changes with acute MR and LV volume overload:
- It may result from connective tissue disorders (e.g., Marfan’s disease), congenital anomalies of the valve,rheumatic valvulitis, or other degenerative conditions , infective endocarditis, ischemic damage to the valve or its supporting chordae, .
- The low resistance runoff into the left atrium results in an increase in ejection fraction and a reduction in systolic volume.
- The ventricle utilizes its preload reserve, resulting in an increase in total stroke volume via the Frank-Starling mechanism.
Chronic compensated MR —
- The major change that occurs during the evolution from acute to chronic MR is an enlargement of the ventricle
- An enlarged compliant atrium contributes to a decline in pulmonary venous pressures.
- The systolic unloading that is characteristic of acute MR is gradually replaced by normal systolic wall stresses as end-systolic volume increases
- Despite LV chamber enlargement, preload at the level of the sarcomere returns to normal or near normal levels .
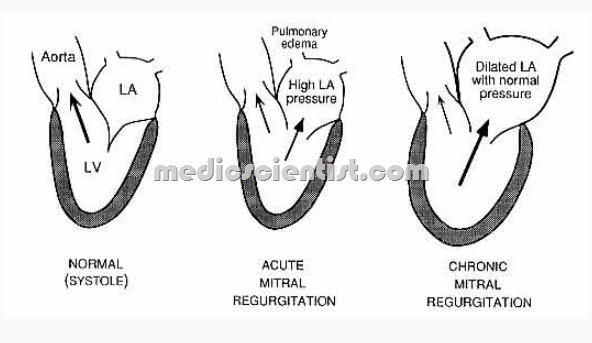
Mitral Regurgitation (MR) Symptoms
- Patients with severe chronic MR often experience exercise intolerance, dyspnea,
- or fatigue during the transition from a compensated to a decompensated stage.
- Fatigue
- Exertional dyspnoea
- Orthopnea
- Features of – LVF
- Pulmonary edema
- RV failure
- Systemic embolism.
- Most experts and the ACC/AHA guidelines recommend that patients with chronic MR who become symptomatic are candidates for corrective mitral surgery, even if the symptoms improve with medical therapy
ACC/AHA guideline summary: Mitral valve surgery (repair or valve replacement) in patients with nonischemic mitral regurgitation (MR)
Class I –
- Symptomatic severe acute MR.
- Asymptomatic severe chronic MR with LVEF of 30 to 60 percent and/or end-systolic dimension 40 mm.
- Severe symptomatic chronic MR (NYHA class II-IV) in the absence of severe left ventricular dysfunction (left ventricular ejection fraction [LVEF] less than 30 percent or end-systolic dimension greater than 55 mm).
Class IIa —
- Asymptomatic patients with severe chronic MR and preserved left ventricular function who have new onset atrial fibrillation or pulmonary hypertension defined as a pulmonary artery systolic pressure >50 mmHg at rest or >60 mmHg with exercise.
- Mitral valve repair in experienced surgical centers in asymptomatic severe chronic MR with preserved left ventricular function (LVEF >60 percent and end-systolic dimension less than 40 mm) if the estimated likelihood of successful repair without residual MR is greater than 90 percent.
Class IIb –
- Mitral valve repair for severe MR due to severe left ventricular dysfunction (LVEF <30 percent) in patients with persistent NYHA class III-IV symptoms despite optimal therapy for heart failure, including biventricular pacing if warranted.
Class III –
- Asymptomatic patients with preserved left ventricular function (LVEF >60 percent and end-systolic dimentsion less than 40 mm) if there is significant doubt about the feasibility of repair.
- Isolated mitral valve surgery for mild to moderate MR.
Mitral Regurgitation (MR) Physical findings
- Arterial pulse may be high volume or in cases of LVF and RVF low volume.
- JVP shows prominent a waves, prominent v waves, or absent a waves as in AF.
- stolic thrill is al able at a ex.
- LV apical impulse hyperdynamic and displaced down and out.
- P2 palpable
- S1 absent or soft Wide split of S2
- P2 loud Signs of PH ma be present-ie loud P2J ejection systolic murmur in left parasternal area, narrow split of S2, RV heave etc.)
- S3 – low pitched, 0.12 to 0.17 seconds after A2 due to sudden tensing of the papillary muscles, chordae tendineae, and valve leaflets.
- S4 is heard in acute severe MR.
- There is typically a systolic murmur grade III or more, holosystolic, may be decrescendo. It is pansystolic or holosystolic ie it extends from 51 to 52 and even engulfs the second heart sound so that the second heart sound is not audible.
- The systolic murmur is best heard at the apex and radiates to axilla.
- If the posterior mitral leaflet is involved, the murmur radiates to the base of heart.
- A musical high-pitched cooing or seagull quality of the systolic murmur occurs in rupture of valve apparatus.
- · There is a short rumbling diastolic murmur – flow murmur (functional murmur of M5).
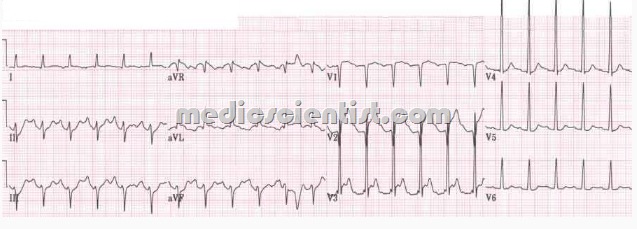
Mitral Regurgitation (MR) ECG
- LAE,
- RAE,
- AF,
- LVH.
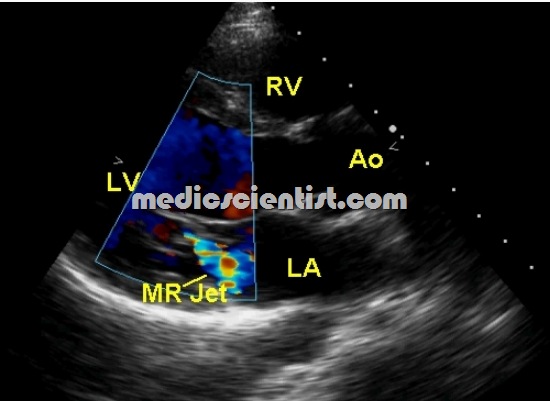
Mitral Regurgitation (MR) Echocardiogram
- · Color flow doppler gives estimation of MR
- · Vegetations
- · LV dilatation
- · Aneurysm
- · MVP may be present.
- · LAE
- · LVH
- · Mitral annular calcification
- · Damaged valve apparatus
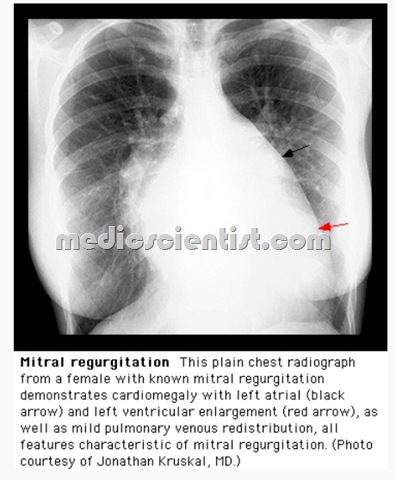
Mitral Regurgitation (MR) X-ray —
- · LA hypertrophy,
- Kerley B lines, calcification of mitral annulus.
- LVH, pulmonary venous congestion,
- Rest
- Reduced sodium intake
- Vasodilators ex. sodium nitroprusside, hydrallazine, NTG, ACE-I
- Digitalis
- NTG (Nitroglycerine) – Oral and IV
- ACE Inhibitors (Angiotensin converting enzymeI)
- Anticoagulants (Warfarin, nicoumalone) Leg binders for venous thrombi Endocarditis prophylaxis
Surgical management for Mitral Regurgitation (MR)
- · Indications of surgery are severe MR, limitation of activity, and progressive LVD.
- · LV EF declining progressively.
- If LVEF less than 30%, surgery is contraindicated.
- · Surgery of choice is mitral valve replacement with a prosthesis.
- · Mitral valvuloplasty or repair of annulus is done in patients of MVP, infective endocarditis, ruptured chordae.
- · After mitral valve replacement long-term, lifelong anticoagulation is done.
