Article Contents ::
- 1 Acute Respiratory Distress Syndrome ARDS
- 2 Criteria of ARDS
- 3 All criteria
- 4 ARDS criteria
- 5 Predisposing factors
- 6 Risk Factorsfor Acute Respiratory Distress Syndrome (ARDS)
- 7 Clinical feature of ARDS
- 8 Physical Exam in ARDS
- 9 X-ray:
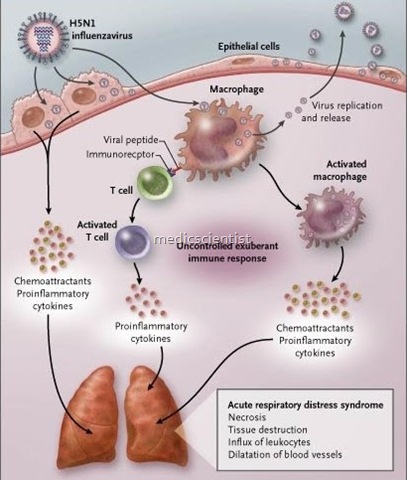
- 10 Pathophysiology of Acute Respiratory Distress Syndrome (ARDS)
- 11 Causes of Acute Respiratory Distress Syndrome (ARDS)
- 12 Treatment of Acute Respiratory Distress Syndrome (ARDS)
Acute Respiratory Distress Syndrome ARDS
- There is lung injury manifested as increased permeability of alveolar capillary membrane, diffuse alveolar damage, proteinaceous pulmonary edema.
- Age: ARDS or Acute Respiratory Distress Syndrome may occur in children or adults.
- Syndrome characterized by abrupt onset of diffuse lung injury with severe hypoxemia and bilateral pulmonary infiltrates
- Absence of left atrial hypertensiom (HTN)
- By consensus, PaO2/FiO2 <200
- Most severe form of acute lung injury
- System(s) affected: Pulmonary; Cardiovascular
- Synonym(s): Shock lung; Wet lung; Noncardiac pulmonary edema
- Acute respiratory distress syndrome (ARDS) develops rapidly and includes severe dyspnea and hypoxemia;
- it typically causes respiratory failure.
- Key diagnostic criteria for ARDS include diffuse bilateral pulmonary infiltrates on chest x-ray (CXR); PaO2 (arterial partial pressure of oxygen in mmHg)
Criteria of ARDS
- Severe hypoxemia
- Decreased pulmonary compliance
- Diffuse pulmonary infiltrates on chest X-ray.
- It is a form of noncardiogenic pulmonary edema. Acute Lung Injury (ALI) is a less severe form of ARDS.
All criteria
- Acute onset
- PaO2/FI02 < 300mg Hg
- Chest X-ray – Bilateral infiltrates.
- PAP –< 18 mmHg (Pulmonary artery pressure is less than 18mmHg).
- No clinical evidence of left atrial hypertension.
ARDS criteria
- Acute onset
- PaO2/FI02 < 200mg Hg
- Bilateral infiltrates.
- PCWP ~ 18 mmHg (Pulmonary capillary wedge pressure is less than 18mmHg).
- No clinical evidence of increased LA pressure.
Predisposing factors
- Severe sepsis, trauma, aspiration of gastric contents. 40% of these will develop ARDS.
- A H/O chronic alcohol abuse increases risk of ARDS.
- ARDS occurs within 5 days of the precipitating event.
- 50% develop within 1 day.
Risk Factorsfor Acute Respiratory Distress Syndrome (ARDS)
- Severe infection (localized or systemic ) most common
- Aspiration of gastric contents
- Shock
- Infection
- Lung contusion
- Nonthoracic trauma
- Toxic inhalation
- Near drowning
- Multiple blood transfusions
Clinical feature of ARDS
- There is : Increased respiratory rate
- Dyspnoea
- In sepsis there is increased ne.
- In pancreatitis, there is increased serum amylase level.
Physical Exam in ARDS
- Flat neck veins
- Hyperdynamic pulses
- Physiologic gallop
- Absence of edema
- Tachypnea and tachycardia during the 1st 12– 24 h; respiratory distress
- Lethargy, obtundation
- Moist, cyanotic skin: Manifestations of underlying disease
X-ray:
- diffuse infiltrates with heterogenous pattern – more in dependent lung.
Pathophysiology of Acute Respiratory Distress Syndrome (ARDS)
- 3 phases:
- Acute exudative phase: Characterized by profound hypoxia and associated with inflammation with infiltration of inflammatory and proinflammatory mediators and diffuse alveolar damage
- Fibrosing alveolitis phase: Coincides with recovery or after ~1–2 weeks; patients continue to be hypoxic and have increased dead space and decreased compliance.
- Resolution may require 6–12 months.
- Heightened inflammatory response Initiation
- Acceleration
- Injury.
Causes of Acute Respiratory Distress Syndrome (ARDS)
- Trauma
- Aspiration of gastric contents –
- Drowning
- Contusion to lungs
- Toxin inhalation
- Sepsis syndrome
- Non-thoracic trauma
- Pancreatitis
- CABG.
- There is mediator and cytokine-release like TNF alpha interleukin-
- 1. Neutrophils cause acceleration of rseponse
- Release of oxygen, metabolites and proteases causes injury leading to MODS (Multiple Organ Dysfunction, Syndrome).
- Pulmonary edema
- Bronchial wall edema
- Narrowing of bronchi leading to :
- Bronchospasm
- High pulmonary vascular resistance
- High pulmonary arteriolar pressure due to
- release of thromboxane A2 and leukotrines.
- There may be recovery or chronic pulmonary disease. Chronic changes in lung often leads to death.
Treatment of Acute Respiratory Distress Syndrome (ARDS)
- No single drug or combination of drugs prevents or treats full-blown ARDS. Treatment is supportive while addressing the underlying cause.
- Supplemental oxygen
- Ventilatory support most often requires endotracheal intubation with emphasis on lower tidal volumes per weight and optimization of positive end-expiratory pressure (PEEP).
- 02 inhalation is not effective.
- Mechanical ventilation should be instituted. Mechanical ventilation can lead to 02 toxicity, barotrauma, pneumothorax, pneumo-mediastinum, SIC emphysema.
- Tidal volume of 10 ml/Kg can lead to barotrauma. Maximum inflation pressure < 35cm H20.
- Tidal volume should be <6 ml/kg.
- FI02 is kept < .6
- Pa02 maintained at 60 mmHg.
- PEEP added 5 cm H20 up to 20 cm H20. Restriction of fluids.
- Inotropic agents: Dobutamine to maintain adequate cardiac output after appropriate fluid resuscitation fails to restore perfusion
- Deep vein thrombosis (DVT) prophylaxis
- Ulcer prophylaxis
- Inhaled B2 agonists may be helpful during the resolution phase.
- Maintain lowest possible intravascular hydrostatic pressure.
- Hypercapnia, respiratory acidosis occurs with mechanical ventilation called permissive hypercapnia.
- Steroids may be given. Give surfactants, nitric oxide inhalation to reduce pulmonary arterial pressure.
- Mortality 50% to 70% Early mortality <3 days Late mortality >3 days
