Article Contents ::
- 1 How to Approach Patient of Liver Disease
- 2 Approach Patient of Liver Disease
- 3 DISEASES OF THE LIVER
- 4 Presenting features are:
- 5 Evaluation of patients of liver disease
- 6 CLINICAL HISTORY of liver disease
- 7 liver disease PHYSICAL EXAMINATION —
- 8 P Y le LEA IATIO OF PATIENTS
- 9 Hepatic failure
- 10 Skin changes in liver disorders
- 11 LABORATORY TESTING IN A PATIENT WITH LIVER DISEASE
- 12 Disease
- 13 Diagnostic test
- 14 DIAGNOSTic IMAGING
- 15 LIVER BIOPSY
- 16 Grading and Classification —
How to Approach Patient of Liver Disease
Approach Patient of Liver Disease
- Liver is the largest organ of the body weighing about 1 Kg.
- It is present in the right upper quadrant of the abdomen under the right lower rib cage and projects into the left upper quadrant.
- 20% of the blood flow is from hepatic artery and rich in oxygen.
- 80% of its blood is rich in nutrients from the portal vein from stomach, intestine, pancreas, and spleen.
- Cells of liver are called hepatocytes.
- Other cells are cells of reticulo-endothelial system of liver called Kupffer cells, fat cells, endothelial cells, blood vessels, bile ductular cells and supporting structures. .
- Liver cells are organized in lobules with central veins in the centre of lobule and portal areas at the borders.
- Portal areas of the liver consist of small veins, arteries, bile ducts and Iymphatics. Blood flows from portal areas through sinusoids to the hepatic veins (central veins). Bile flows from central vein to portal area.
- The hepatocytes synthesize serum proteins like albumin, coagulation factors, hormonal and growth factors, produce bile acids, cholesterol, and regulate nutrients like glucose, glycogen, lipids, cholestero.L.amino acids, and excrete bilirubin, anions and cations in the bile or urine.
- Therefore, function of the liver is tested by measurement of serum bilirubin, albumin, prothrombin time.
DISEASES OF THE LIVER
- 1. Hepatocellular – viral hepatitis, alcoholic liver disease.
- 2. Cholestatic – gall stones, malignancy, biliary cirrhosis, drug-induced.
- 3. In viral hepatitis, hepatocellular damage as well
- as cholestatic disease is seen.
Presenting features are:
- 1. Jaundice
- 2. Itching
- 3. Fatigue and weakness
- 4. Right upper quadrant pain
- 5. Abdominal distention
- 6. Intestinal bleeding.
Evaluation of patients of liver disease
- 1. For etiology
- 2. For severity
- 3.For staging. Diagnosis is :
- 4. Category – Hepatocellular or cholestatic or both.
- 5. Grading – Active, Inactive, Mild, Moderate, Severe.
- 6. Staging – Acute or chronic, early or late, cirrhotic or precirrhotic, or end-stage.
CLINICAL HISTORY of liver disease
- A complete medical history is the single most important part of the evaluation of the patient with elevated LFTs.
- Important considerations include: The use of or exposure to any chemical or medication (including prescription and over-the-counter medications as well as herbal therapies) which may be temporally related to the onset of LFT abnormalities
- The duration of LFT abnormalities
- The presence of any accompanying symptoms such as jaundice, arthralgias, myalgias, rash, anorexia, weight loss, abdominal pain, fever, pruritus, and changes in the urine and stoo
- Fatigue, weakness, nausea, loss of appetite, malaise, jaundice, dark urine, light stools, itching, pain in abdomen, bloating of abdomen.
- · Fatigue occurs during the afternoon. Nausea occurs by the site of food.
- · Jaundice is not detectable when serum bilirubin is less than 2.5 mg/dl.
- · Jaundice without dark urine indicates indirect or unconjugated bilirubinemia as in hemolytic ‘ anaemia and Gilbert’s syndrome and Crigler Najjar syndrome.
- History: Alcohol use, herbal drugs, birth control pills, sexual activity, travel, exposure, surgery, blood transfusion, exposure to blood or needle, family history of liver disease.
- Sexual exposure is important for hepatitis B but not for hepatitis C.
- Mother to child transmission occurs in hepatitis Band C.
liver disease PHYSICAL EXAMINATION —
- The physical examination should focus upon findings suggesting the presence of liver disease.
- Specific findings may provide clues toward diagnosis of an underlying cause.
- Temporal and proximal muscle wasting suggest longstanding diseases
- Stigmata of chronic liver disease include spider nevi, palmar erythema, gynecomastia, caput medusae
- Dupuytren’s contractures, parotid gland enlargement, and testicular atrophy are commonly seen in advanced Laennec’s cirrhosis and occasionally in other types of cirrhosis
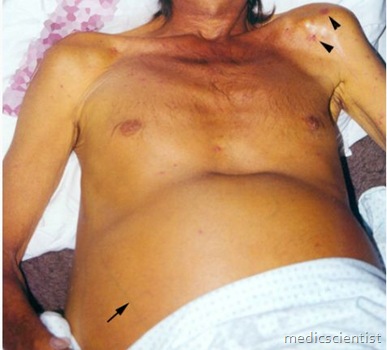
- An enlarged left supraclavicular node (Virchow’s node) or periumbilical nodule (Sister Mary Joseph’s nodule) suggest an abdominal malignancy
- Jugular venous distension, a sign of right sided heart failure, suggests hepatic congestion
- A right pleural effusion, in the absence of clinically apparent ascites, may be seen in advanced cirrhosis
- Familial causes of liver disease are:
- 1. Wilson’s disease.
- 2. Hemachromatosis – suggested by cirrhosis, diabetes and liver disease in adult.
- 3. Alpha 1 antitrypsin deficiency
- 4. Benign intrahepatic cholestasis.
P Y le LEA IATIO OF PATIENTS
- 1. Icterus or jaundice
- 2. Hepatomegaly
- 3. Hepatic tenderness
- 4. Splenomegaly
- 5. Spider angiomata
- 6. Palmar erythema
- 7. Excoriations
- 8. Muscle wasting
- 9. Ascites, edema
- 10. Dilated abdominal veins
- 11. Hepatic fetor (foul breaths)
- 12. Asterixis (flapping tremor)
- 13. Mental confusion, stupor, coma.
- Jaundice is seen in the sclera in daylight, in the skin and in mucus membrane below tongue.
Hepatic failure
- Hepatic failure is indicated by presence of signs and symptoms of hepatic encephalopathy in a patient of severe acute or chronic liver disease.
- Features of hepatic failure:
- 1. Change in sleep patterns
- 2. Change in personality
- 3. Irritability
- 4. Mental dullness
- 5. Confusion, disorientation
- 6. Stupor, coma
- 7. Asterixis / flapping tremors of body and tongue
- 8. Fetor hepaticus – sweet ammonia odour in breath
- 9. Trail making test is positive i.e. patient is unable to connect 25 numbered circles using a pencil within 30 seconds
- 10. Ascites with umbilical hernia
- 11. Prominent veins over abdomen and caput medusa – veins radiating from umbilicus
- 12. Widened pulse pressure – Hyperdynamic circulation – sodium and fluid retention – increased cardiac output – reduced peripheral resistance.
- 13. Hepatopulmonary syndrome – Liver disease with hypoxemia and pulmonary arteriovenous shunting. There is dyspnoea and shortness of breath and oxygen desaturation in the upright or sitting position.
Skin changes in liver disorders
- · Hyperpigmentation – Cholestatic liver disease
- · Xanthelasma
- · Tendon xanthomata
- · Gray pigmentation in hemochromatosis
- · Mucocutaneous vasculitis with purpura in cryoglobulinemia of hepatitis C or B.
- Eye changes in liver disorders Jaundice.
- Kayser-Fleischer ring in Wilson’s disease – a golden brown copper pigment in Disemet’s membrane at the periphery of the cornea, seen by slit lamp.
- Metastatic liver disease and primary hepatocellular carcinoma
- Features are:
- · Cachexia
- · Wasting
- · Hepatomegaly
- · Hepatic bruit
- · Hepatic failure.
LABORATORY TESTING IN A PATIENT WITH LIVER DISEASE
- Liver panel tests are:
- 1. Serum alanine transferase – ALT (SGPT)
- 2. Serum aspartate aminotransferase – AST (SGOT)
- 3. Alkaline phosphatase
- 4. Direct and total serum bilirubin
- 5. Serum albumin
- 6. Prothrombin time
- 7. GGT (Gamma Glutamyl Transpeptidase)
- 8. Anti mitochondrial antibody – AMA – Autoimmune marker in primary biliary cirrhosis
- 9. P-ANCA – peripheral anti neutrophil cytoplasmic antibody in sclerosing cholangitis
- 10. ANA – antinuclear antibody
- 1 L ASMA – anti smooth muscle antibody; liver, kidney, microsomal antibody.
-
Disease
- Hepatitis A
- Hepatitis B – Acute
- Hepatitis B – Chronic Hepatitis C
- Hepatitis D
- Hepatitis E
- Autoimmune hepatitis Primary biliary cirrhosis Primary sclerosing cholangitis Drug-induced
- Alcoholic
- Alpha-l antitrypsin disease Wilson’s disease Hemochromatosis Hepatocellular cancer
Diagnostic test
- Anti HAV IgM
- HBsAg and anti HBc IgM HBsAg and HBeAg,
- HBV DNA Anti HCV and HCV RNA HBsAg and Anti HDV
- Anti HEV
- ANA or SMA
- AMA – Anti-mitochondrial antibody P – ANCA
- History
- History and histology
- Reduced alpha 1 antitrypsin levels
- Decreased serum ceruloplasmin, increased urinary copper Increased iron saturation and serum ferritin
- Increased alpha fetoprotein level more’than 500, Ultrasound and CT Scan
DIAGNOSTic IMAGING
- 1. Ultrasound
- 2. Computed Tomography (CT)
- 3. Magnetic resonance imaging (MRI)
- 4. Magnetic resonance cholangiopancreato-graphy (MRCP)
- 5. Endoscopic retrograde cholangiopancreatography (ERCP)
- 6. Doppler, ultrasound and MRI for hepatic vasculature
LIVER BIOPSY
- For chronic liver diseases:
- • Diagnosis
- · Severity
- · Prognosis
- · Monitoring treatment
Grading and Classification —
- 1. Child-Pugh classification – Serum bilirubin, serum albumin, ProthrombinTime, ascites, hepatic encephalopathy are taken into account and A-BC staging is done.
- 2. Liver biopsy is done and amount of fibrosis is staged from 0 to 4+ (histology activity index) or on Ishak scale from 0 to 6+.
- 3. MELD score – model for end-stage liver disease for assessment for liver transplantation.
