Article Contents ::
Nephrotic Syndrome
Nephrotic syndrome is characterized by proteinuria > 3 to 3.5 g / 24 hrs., Associated with many types of kidney disease hypoalbuminemia, edema, hyperlipidemia, Iipiduria, and hypercoagulability. Nephrotic syndrome is a disease of glomerular basement membrane, . podocyte-slit diaphragm. A condition marked by increased glomerular permeability to proteins, resulting in massive loss of proteins in the urine, edema, hypoalbuminemia, hyperlipidemia, and hypercoagulability.
Causes of nephrotic syndrome
- are minimal change disease, focal and segmental glomerular sclerosis,
- · membranous glomerulopathy, membrano-proliferative glomerulonephritis, diabetic nephropathy, and amyloidosis.
- Nephrotic syndr.ome responds well to glucocorticoids. The chief feature of nephrotic syndrome is proteinuria. Hypoalbuminemia is due to loss of protein in urine, increased renal ca.tabolism, increased hepatic synthesis of albumin. ,
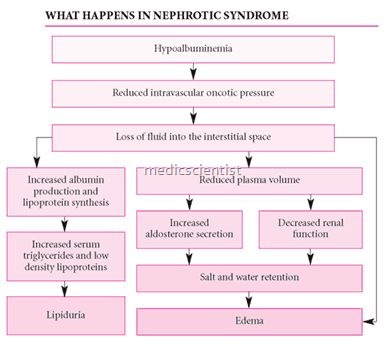
- Edema is due to hypoalbuminemia, decreased intravascular oncotic pressure, leakage of extra cellular fluid (ECF) to interstitial spaces, decrease of intravascular volume, activation of renin- angiotensin-aldosterone axis and the sympathetic nervous system, and release of vasopressin, and suppression of atrial natriuretic peptide release, renal salt and water retention.
- Hyperlipidemia is due to increased hepatic lipoprotein synthesis, leading to atherosclerosis and worsening of renal disease.
- Hypercoagulability is due to increased urinary loss of antithrombin III, protein C and 5, hyperfibrinogenemia, increased platelet aggregation. This leads to peripheral arterial and venous thrombosis, renal vein thrombosis, pulmonary thromboembolism.
- Renal vein thrombosis occurs in nephrotic syndrome if it is due to membranous glomerulopathy, membranoproliferative glomerulopathy, amyloidosis.
- There is protein malnutrition.
- There is macrocytic hypochromic anaemia .
- There is hypocalcemia and vitamin D deficiency and secondary hyperparathyroidism. There is also increased incidence of infections.
Physical Exam in Nephrotic Syndrome
- A complete physical exam may discover clues to systemic disease as a potential cause and/or may suggest the severity of disease:
- Fluid retention: Abdominal distention, abdominal fluid shift, extremity edema, puffy eyelids, scrotal swelling, weight gain, shortness of breath:
- Pericardial rub and decreased breath sounds with pleural effusions may develop.
- Hypertension
- Orthostatic hypotension
History of Nephrotic Syndrome
- Look for signs or symptoms of systemic disease:
- Joint complaint, rash, edema, infectious complaint, fevers, anorexia, oliguria, foamy urine, acute flank pain, hematuria, etc.
- Look for a recent drug history that may be causative, especially nonsteroidal anti-inflammatory drugs (NSAIDs).
- Assess for risk factors.
Nephrotic Syndrome Risk Factors
- Drug addiction (e.g., heroin [FSGS])
- Hepatitis B and C, HIV, other infections
- Cancer (usually MGN, may be MCD)
- Chronic analgesic use/abuse
- Preeclampsia
- Immunosuppression
- Nephrotoxic drugs
- Vesicoureteral reflux (FSGS)
Symptoms :
- Patients with nephrotic syndrome may initially present with fluid retention in the legs or symptoms caused by blood clotting (e.g., in the renal vein).
- The hyperlipidemia that often accompanies the syndrome may lead to symptoms caused by atherosclerosis.
Treatment of Nephrotic Syndrome
- Treat the etiology.
- General measures for proteinuria. Control of complications
- For proteinuria – ACE inhibitors, ARBs (Angiotensin Receptor Blockers), NSAIDs.
- These drugs lower the intraglomerular pressure and prevent glomerulosclerosis and also decreased protein loss.
- ACE (Angiotensin converting enzyme) inhibitors and ARBs (Angiotensin receptor blockers) are also very useful in diabetic nephropathy.
- NSAIDs can however cause hyperkalemia, salt water retention, acute renal failure.
- Salt restriction 1 – 2 g/day, loop diuretics (weight reduction should not be > 1 kg/day by removal of edema fluid).
- Lipid-lowering drugs.
- Anticoagulation in patients with thrombosis. Diet: moderate amounts of proteLrYi~e. 0.8 g/ kg/day plus 1 g for each grafT. protein lost in urine, vitamin D supplements.
- Many of the nephrotic diseases will require escalation in therapy above steroids.
- These include rapidly relapsing forms as well as MGN, LN, and IgA nephropathy:
Admission Criteria
- Respiratory distress, sepsis/severe infection, thromboses, renal failure, hypertension, or other complications
Discharge Criteria
- Hemodynamically stable patients without complications may be managed as outpatients.
