Article Contents ::
- 1 Porphyrias
- 2 Porphyrias are classified as :
- 3 The hepatic porphyrias present with neurologic features:
- 4 The erythropoie.tic porphyrias present with:
- 5 Porphyrias Classification of the human porphyrias
- 6 Causes of porphyrias :
- 7 Risk Factors
- 8 HEPATIC PORPHYRIAS
- 9 ALA-dehydratase deficient porphyria
- 10 Acute intermittent porphyria
- 11 Hereditary corpoporphyria
- 12 Treatment:
- 13 Variegate porphyria
- 14 Congenital porphyria
- 15 Treatment:
Porphyrias
The porphyrias are inherited disorders. porphyrias are metabolic disorders caused by altered activities of enzymes within the heme biosynthetic pathway
- Acute intermittent porphyria: Pyrroloporphyria; neuropsychiatric–abdominal
- -Aminolevulinic aciduria; neuropsychiatric–abdominal
- Congenital erythropoietic porphyria: Günther disease; severe dermatologic
- Hereditary coproporphyria: Neuropsychiatric, occasionally dermatologic
- Other rare genetic variants reported
- Porphobilinogen synthetase deficiency:
- Porphyria cutanea tarda: Dermatologic
- Protoporphyria: Erythropoietic or hepatoerythropoietic; mild dermatologic
- Variegate porphyria: South African porphyria; prevalence in South Africa is 1/400.
Each involves a specific enzyme of heme biosynthesis.
Porphyrias are classified as :
- · Hepatic – (neuropathic features)
- · Erythropoietic – (skin involvement).
The hepatic porphyrias present with neurologic features:
- · Neuropathic abdominal pain
- · Neuropat~y
- · Mental disturbances.
The erythropoie.tic porphyrias present with:
- · Cutaneous sehsitivity
- · Scarring and pigmentation of skin.
Porphyrias Classification of the human porphyrias
- as hepatic or erythropoietic and as acute or cutaneous, the affected enzymes, patterns of inheritance and their major biochemical features
| Disease | Classification | Enzyme affected* | Inheritance | Major biochemical findings | ||||
| Tissue site | Clinical features | Urine | Plasma | Erythrocytes | Feces | |||
| -minolevulinic acid dehydratase porphyria (ADP) | Hepatic | Acute | ALAD | Autosomal recessive | ALA, copro-porphyrin III | ALA, copro-porphyrin III | Zinc proto-porphyrin & low ALAD activity | |
| Acute intermittent porphyria (AIP) | Hepatic | Acute | PBGD | Autosomal dominant | ALA, PBG, copro-porphyrin | Low PBGD activity | ||
| Hereditary coproporphyria (HCP) | Hepatic | Acute & cutaneous | CPO | Autosomal dominant | ALA, PBG, copro-porphyrin III | Copro-porphyrin III | ||
| Variegate porphyria (VP) | Hepatic | Acute & cutaneous | PPO | Autosomal dominant | ALA, PBG, copro-porphyrin III | Fluorescence peak at 626 nm | Copro-porphyrin III & protoporphyrin | |
| Porphyria cutanea tarda (PCT) | Hepatic | Cutaneous | UROD | Autosomal dominant | Uroporphyrin & hepta-carboxyl-porpyrin | Uroporphyrin & hepta-carboxyl-porpyrin | Isocopro-porphyrin | |
| Hepato-erythropoietic porphyria (HEP) | Hepatic | Cutaneous | UROD | Autosomal recessive | Uroporphyrin & hepta-carboxyl-porpyrin | Uroporphyrin & hepta-carboxyl-porpyrin | Zinc proto-porphyrin & low UROD activity | Isocopro-porphyrin |
| Congenital erythropoietic porphyria (CEP) | Erythro-poietic | Cutaneous | UROS | Autosomal recessive | Uroporphyrin I & copro-porphyrin I | Uroporphyrin I & copro-porphyrin I | Uroporphyrin I & copro-porphyrin I | Copro-porphyrin I |
| Erythropoietic protoporphyria (EPP) – classic form | Erythro-poietic | Cutaneous | FECH | Autosomal dominant | Protoporphyrin | Free protoporphyrin | Protoporphyrin | |
| EPP – variant form | Erythro-poietic | Cutaneous | ALAS2 | X-linked recessive | Protoporphyrin | Free & zinc protoporphyrin | Protoporphyrin | |
Causes of porphyrias :
- · Environmental
- · Physiological
- · Genetic.
- The porphyrias are diagnosed and classified by chromatography and demonstration of specific enzyme deficiency or gene defect
Risk Factors
- Drugs (e.g., barbiturates and sulfas in acute intermittent porphyria)
- Estrogens (especially oral contraceptives)
- Fasting
- Heavy alcohol use
- Hexachlorobenzene exposure
- Infection
- Liver disease
- Multiple precipitating factors, especially in acute intermittent porphyria, variegate porphyria, hereditary coproporphyria
- Steroids
HEPATIC PORPHYRIAS
- There is rapid onset of neurologic manifestations. There is elevated levels of plasma and urinary ALA (Urinary gamma amino levulinic acid and PBG-Porphobilinogen).
ALA-dehydratase deficient porphyria
- Clinical features are abdominal pain and neuropathy.
Acute intermittent porphyria
- This is a common porphyria.
- The disease is activated by drugs, low calorie diet, steroids, alcohol.
- It presents with :
- Abdominal pain Diarrhea
- Fever
- Vomiting
- Hypertension
- Pain in the limbs Muscle weakness Mental symptoms Peripheral neuropathy.
Treatment: Narcotic analgesics, IV glucose, phenothiazines Porphyria cutanea tarda There is :
- Cutaneous photosensitivity
- Vesicles and bullae on exposed skin Hyperpigmentation
- It is precipitated by alcohol, iron, estrogens Treatment: Repeated phlebotomy (450 ml of blood is removed by cutting a vein), chloroquine, hydrochloroquine(HCQ) .
Hereditary corpoporphyria
- Common in women
- There is photosensitivity of skin
Treatment:
- phlebotomy and chloroquine
Variegate porphyria
- Presents with neurological symptoms and photosensitivity
- ERYTHROPOIETIC PORPHYRIAS X-linked sideoblastic anaemia
- There is refractory anaemia, hypersplenism, hemosiderosis
Treatment: is pyridoXine supplementation
Congenital porphyria
- Also known as Gunther’s Disease.
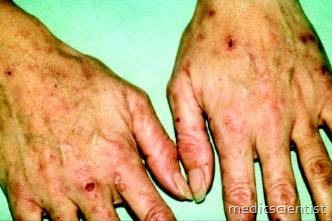
- Very rare and associated with hemolytic anaemia. Cutaneous lesions – hyperpigmentation, thickening of skin, disfigurement of face and hands.
- Teeth reddish brown.
Treatment:
- is splenectomy, protection from sunlight, beta carotene, bone marrow transplant, stem cell therapy
