Article Contents ::
- 1 Sarcoidosis
- 2 Sarcoidosis Diagnosis Characterized by :
- 3 Organs most commonly involved:
- 4 Course of Disease may be
- 5 Sarcoidosis Etiology
- 6 Sex
- 7 Age
- 8 Sarcoidosis Pathophysiology and Immunopathogenes’s
- 9 Sarcoidosis Clinical symptoms
- 10 Constitutional symptoms are present:
- 11 Heerfordt- Waldenstrom syndrome:
- 12 Lungs
- 13 Necrotizing sarcoidal granulomatosis
- 14 Lymph node enlargement
- 15 Lymphadenopathy – (usually of hilar nodes)
- 16 Skin
- 17 Eyes
- 18 Keratoconjunctivitis sicca syndrome
- 19 Upper respiratory tract
- 20 Symptoms
- 21 Bone marrow / Spleen
- 22 Liver
- 23 Kidney
- 24 Nervous system
- 25 Musculoskeletal system
- 26 Heart
- 27 Endocrine and Reproductive system
- 28 Pregnancy
- 29 Parotids involvement
- 30 Gastrointestinal system (GIT)
- 31 Death
- 32 Diagnosis Test —
- 33 Sarcoidosis INVESTIGATIONS
- 34 Chest x-ray
- 35 X-Ray findings
- 36 Lung function tests
- 37 Sarcoidosis TREATMENT
- 38 First Line TREATMENT
- 39 Second Line TREATMENT
Sarcoidosis
It is a chronic, multisystem disorder of unknown cause.
- chronic multisystem disease of unknown etiology, characterized by noncaseating (hard) granulomas and lymphocytic alveol,
- Sarcoidosis is a noninfectious, multisystem granulomatous disease of unknown cause, commonly affecting young and middle-aged adults.
- Almost any other organ may be involved, including liver, spleen, lymph nodes, heart, and CNS.
- Also can be diagnosed in asymptomatic patients with abnormal CXRs
- Frequently presents with hilar adenopathy, pulmonary infiltrates, ocular and skin lesions
- Systems affected: Primarily Pulmonary but also Cardiovascular; GI; Hematologic/Lymphatic; Endocrine; Renal; Neurologic; Dermatologic; Ophthalmologic; Musculoskeletal
Sarcoidosis Diagnosis Characterized by :
- · T Iymphocytes and phagocytes
- · Granulomas (non-caseating) in various organs.
- No definitive test for diagnosis, but diagnosis is suggested by the following:
- Clinical and radiographic manifestations
- Exclusion of other diagnoses
- Histopathologic detection of noncaseating granulomas
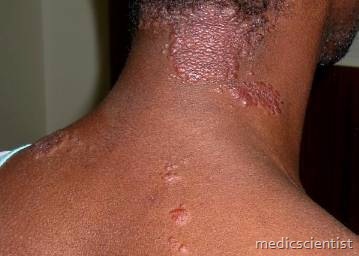
Organs most commonly involved:
- · Lung
- · Skin
- · Eye
- · Liver
Course of Disease may be
- · Acute ,
- · Sub-acute
- · Chronic.
Sarcoidosis Etiology
- · Cause unknown
- · Self-antigens may be responsible for disease
- · Disease is due to exaggerated cellular immune response.
Sex
- · Females may be more susceptible
- · Male: Female 1: 1, both sexes equally affected usually.
Age
- · Common between 20 – 40 years
- · Children and elderly can also be affected.
Sarcoidosis Pathophysiology and Immunopathogenes’s
- · Accumulation of CD4 + TH11ymphocytes in or- gan
- · Granulomas
- Thought to be due to exaggerated cell-mediated immune response to unknown antigen(s)
- In the lungs, the initial lesion is CD4+ T-cell alveolitis, causing noncaseating granulomata, which may resolve or undergo fibrosis.
- · Multinucleated giant cells/Langhans giant cells
- · Schaumann bodies–Conch-like (Shankh)
- · Asteroid bodies.
Sarcoidosis Clinical symptoms
- · Systemic disease
- · Lungs involved-respiratory symptoms mainly
- · May be asymptomatic (discovered on chest xray)
- · May present abruptly (suddenly) or slowly in weeks or months
- · Usually at ages <40 yrs.
- If signs indicate Löfgren syndrome, it is not necessary to perform a biopsy because prognosis is good with observation alone, and biopsy would not change management.
Constitutional symptoms are present:
- · Fever, fatigue, anorexia (loss of appetite), weight loss.
Respiratory symptoms: Cough, Dyspnoea Retrosternal chest discomfort Polyarthritis Lofgren‘s syndrome:
- · Erythema nodosum
- · Bilateral hilar adenopathy
- · Arthritis of ankles, knees, wrists, elbows.
Heerfordt- Waldenstrom syndrome:
- · Fever
- · Parotid enlargement
- · Anterior uveitis
- · Facial nerve palsy.
Lungs
- · Interstitial lung disease
- · Alveoli, small bronchi, small blood vessels in- volved
- · There is dyspnoea, dry cough
- · There are dry rales in lungs
- · Hemoptysis may be present
- · Lung collapse can occur due to : – Endobronchial sarcoidosis
- – Pressure from enlarged lymph nodes
- · Wheezing may be present.
Necrotizing sarcoidal granulomatosis
- · Pulmonary artery – granulomatous arteritis
- · Pleural effusion – usually unilateral
- · Chronic pleural thickening
- · Pneumothorax
- · Hydropneumothorax.
Lymph node enlargement
- · Discreet
- · Firm
- · Rubbery
- · Painless.
Lymphadenopathy – (usually of hilar nodes)
- · Paratracheal lymph node
- · Mediastinal lymph node
- · Cervical
- · Axillary
- · Inguinal
- · Mesenteric
- · Retroperitoneal.
Skin
- · Erythema nodosum
- · Plaques
- · Subcutaneous nodules
- · Maculopapular eruptions
- · Lupus pernio – purple, swollen and shiny patches on nose, cheeks, lips, ears, fingers
- · Clubbing of fingers
- ·Polyarthralgias may occur with skin lesions. Resolves in 2 to 4 weeks.
- Skin lesions are usually seen on face-around eyes and nose, buttocks, extremities, back.
Eyes
- · Can cause blindness
- · Can involve uveal tract, iris, ciliary body, choroid, conjunctiva
- ·Blurred vision, photophobia.
Keratoconjunctivitis sicca syndrome
- • Dry, painful eyes.
Upper respiratory tract
- · Nasal stuffiness
- · Tonsil involvement
- · Tongue involvement
- ·Larynx.
Symptoms
- · Hoarseness of voice
- · Dyspnoea
- · Wheezing
- · Stridor
- · Even complete obstruction of passage.
Bone marrow / Spleen
- · Anaemia
- · Neutropenia
- · Eosinophilia
- · Thrombocytopenia
- · Splenomegaly.
Liver
- · Hepatomegaly
- · Usually mild features
- · Jaundice
- · Portal hypertension.
Kidney
- Rare involvement
- Granulomas produce 1, 25 dihydroxy-vitamin D which can lead to increased calcium absorption in the gut causing nephrolithiasis.
- Tubular, glomerular, renal artery disease can occur.
Nervous system
- · Seventh nerve involvement with facial paralysis sudden, transient (for short period)
- · Optic nerve dysfunction
- · Papilledema
- · Hypothalamic and pituitary abnormalities
- · Chronic meningitis
- · Granulomas (space occupying lesions)
- · Seizures
- · Peripheral neuropathy
- · Spinal disease.
Musculoskeletal system
- · Involvement of bones, joints, muscles
- · Swelling of digits
- · Arthritis
- · Deformities of joints
- · Polymyositis.
Heart
- • LVH
- .’ Arrhythmias
- · Conduction defects (CHB)
- · Sudden death
- · Papillary muscle dysfunction (PMD)
- · Pericarditis
- · CHF
- · Corpulmonale.
Endocrine and Reproductive system
- · Diabetes insipidus
- · Hypopituitarism
- · Addison’s syndrome,
Pregnancy
- · Patient may improve during pregnancy but worsens after del ivery.
Parotids involvement
- • Bilateral non-tender, smooth enlargement.
Gastrointestinal system (GIT)
- • Rare,
Death
- · Occurs due to respiratory disease
- · CHF,
Diagnosis Test —
Sarcoidosis INVESTIGATIONS
- Lymphocytopenia Increased ESR Hyperglobuli.nemia
- Increased ACE (angiotensin converting enzyme) levels,
Chest x-ray
- · Type I-
- · Type II
- bilateral hilar lymphadenopathy
- – bilateral hilar lymphadenopathy with parenchymal changes
- Type III – no hilar lymphadenopathy, only diffuse parenchymal changes
- Type I – acute, reversible
- Type Il, III – chronic, progressive
X-Ray findings
- · Egg-shell calcification of lymph nodes
- · Pleural effusion
- · Cavitation
- Collapse Pneumothorax Cardiomegaly
- Pulmonary hypertension changes,
Lung function tests
- · Decreased lung volumes
- · Airflow limitation,
- Gallium 67 lung scan
- • Diffuse uptake.
- Bronchoalveolar lavage (BAL)
- • IncreasedCD4+THl.
Sarcoidosis TREATMENT
- Therapy of choice is glucocorticoids : Prednisone1 mg/kg for 4-6 weeks, tapered in 3 months.
- Others are:
- Methotrexate – 5-15 mg/week single dose orally.
- Indomethacin
- Chloroquine
- Pentoxifylline
- Allopurinol
- Levamizole
- Azothiaprine
- Cyclophosphamide
- Cyclospori ne,
- There is spontaneous remission or cure in 50% of patients, However glucocorticoids may be given in symptomatic patients or patients with organ derangement,
First Line TREATMENT
- No treatment may be necessary in asymptomatic individuals, but treatment may be needed for specific indications, such as cardiac, CNS, or ocular involvement.
- ›Systemic therapy is clearly indicated for hypercalcemia, cardiac disease, neurologic disease, and eye disease not responding to topical therapy.
- ›Treatment of pulmonary and skin manifestations is done on the basis of impairment. The symptoms that necessitate systemic therapy remain controversial.
- Systemic corticosteroids in the symptomatic individual:
- ›If no relapse, 15–20 mg/d × 8–12 months
- ›If stable, taper by 5 mg/wk to 15–20 mg/d over the next 6 weeks
- ›Relapse is common.
- ›Usually prednisone initially, 40–60 mg/d × 1st 6 weeks
- Contraindications: Patients with known problems with corticosteroids
- In patients with skin or ocular disease, topical steroids may be effective.
- Precautions: Careful monitoring in patients with diabetes mellitus and/or hypertension
- Significant possible interactions: Refer to the manufacturer’s profile of each drug .
Second Line TREATMENT
- Azathioprine: 50–100 mg/d
- Cyclophosphamide: 25–50 mg/d, increasing to goal white blood cell (WBC) count of 4,000–7,000/mm3
- Hydroxychloroquine (Plaquenil): 100–400 mg/d
- Infliximab, a chimeric monoclonal antibody, has been useful in refractory cases. Dose is 3–5 mg/kg IV initially, 2 weeks later, then q4–6wk.
- Methotrexate: 10–15 mg/wk
- Thalidomide has been used for chronic skin lesions. The anti-tumor necrosis factor (TNF) agent infliximab also has been used in some refractory cases
- Use of immunosuppressants such as methotrexate or azathioprine will require regular monitoring of CBC and LFTs.
