Article Contents ::
- 1 Diagnosis Systemic Sclerosis —
- 2 History
- 3 Systemic Sclerosis Physical Exam
- 4 Systemic Sclerosis Clinical manifestations Symptoms
- 5 Systemic Sclerosis Lab investigations
- 6 Imaging investigations —
- 7 Systemic Sclerosis Management
- 8 Causes of Raynaud’s phenomenon
- 9 Management of Raynaud’s phenomenon
- 10 Management Treatment of Systemic Sclerosis —-
- 11 Additional Therapies
Diagnosis Systemic Sclerosis —
Scleroderma (systemic sclerosis [SSc]) is a chronic disease of unknown cause characterized by diffuse fibrosis of skin and visceral organs and vascular abnormalities
History
- Raynaud phenomenon is frequently the initial complaint.
- Skin thickening, “puffy hands,” and gastroesophageal reflux disease (GERD) are often noted early in the disease process.
Systemic Sclerosis Physical Exam
- · •BP
- · •Skin:
- o Tightness, swelling, thickening of digits
- o Subcutaneous calcinosis
- o Scaling of skin
- o Pruritus
- o Narrowed oral aperture
- o Hypopigmentation
- o Hyperpigmentation
- o Digital ulcerations
- · •Peripheral vascular system:
- o Raynaud phenomenon (differentiate from Raynaud disease, generally affecting younger individuals and without digital ulcers)
- o Telangiectasia
- · •Joints, tendons, and bones:
- o Sclerodactyly
- o Polyarthralgia
- o Joint stiffness
- o Hand swelling
- o Friction rub on tendon movement
- o Flexion contractures
- · •Muscle:
- o Proximal muscle weakness
- o Weakness
- · •GI tract:
- o Xerostomia
- o Weight loss
- o Nausea and vomiting
- o Malabsorptive diarrhea
- o Esophageal reflux owing to dysmotility (most common systemic sign in diffuse disease)
- o Dysphagia
- · •Kidney:
- o May develop scleroderma renal crisis: Acute renal failure
- o Hypertension
- · •Pulmonary:
- o Dry crackles at lung bases
- o Dyspnea
- · •Nervous system:
- o Trigeminal neuropathy
- o Peripheral neuropathy
- · •Cardiac (progressive disease):
- o Secondary cor pulmonale
- o Conduction abnormalities
- o Cardiomyopathy
Systemic Sclerosis Clinical manifestations Symptoms
- Pain (67 percent)
- Sleep difficulties (66 percent)
- Skin discoloration (47 percent)
- Fatigue (76 percent)
- Stiff joints (74 percent)
- Loss of strength (68 percent)
- 1. Raynaud’s phenomenon
- – Precipitated by cold, vibration, emotional stress.
- – There is pallor, followed by cyanosis, followed by redness on rewarming.
- – There is coldness and numbness of finger with pain and tingling.
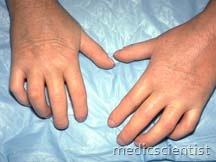
- 2. Swelling of fingers, hands, forearms, feet, legs, face
- 3. There is redness and thickening of skin
- 4. Skin may become thin and atrophic
- 5. Pigment, ulcers may be found on skin
- 6. Polyarthritis
- 7. Muscle weakness
- 8. Peptic ulcer
- 9. Dysphagia
- 10. Malabsorption syndrome
- 11. Dyspnoea, cough
- 12. Interstitial fibrosis
- 13. Pulmonary hypertension
- 14. RVF
- 15. Pericarditis
- 16. Heart failure
- 17. Heart block and arrhythmias
- 18. Renal failure
- 19. Hypertension, malignant hypertension
- 20. Sjogren’s syndrome-chronic autoimmune disease with xerostomia (dry mouth) and xerophthalmia (dry eyes)
- 21. Hypothyroidism.
Systemic Sclerosis Lab investigations
- · ESR increased
- · Anaemia
- · Anti-nuclear antibodies ANA detected. ,
- Nail fold capillary microscopy
- CBC
- Creatinine
- Urinalysis
- Antinuclear antibodies (ANAs), Scl-70 in systemic disease, and anticentromere antibodies in CREST variant
- ECG
- Cardiac echo
- Pulmonary function tests (PFTs)
Imaging investigations —
- Radiographic evidence of soft tissue atrophy and acro-osteolysis
- Can see overlap syndromes such as rheumatoid arthritis
- Barium enema:
- Colonic diverticula
- Megacolon
- Chest radiograph:
- Diffuse reticular pattern
- Bilateral basilar pulmonary fibrosis
Systemic Sclerosis Management
- · Blood Pressure monitoring
- · Blood counts
- · Urine analysis
- · Renal function tests
- · Pulmonary function tests
- · Immunosuppressive drugs-Colchicine, D-penicHlamine, Interferon alpha, chlorambucil
- · Minocycline
- · Etanercept
- · Anti platlet thera py
- · Glucocorticoids
- · Skin care.
Causes of Raynaud’s phenomenon
- · Systemic sclerosis
- · Connective tissue diseases
- · Thoracic outlet syndromes-cervical rib
- · Shoulder hand syndrome
- · Trauma
- · Vibratory machine operators
- · Cold injury
- · Cold agglutinins.
Management of Raynaud’s phenomenon
- · Warm clothes
- · Avoid amphetamine, ergotamine
- · Avoid beta blockers
- · Prazosin may be useful
- · Nifedipine, Diltiazem, Amlodipine may relieve
- symptoms
- · Sildenafil
- · Losartan (ARB)
- · IV Iloprost (Prostacyclin)
- · IV Epoprostenol
- · Pentoxiphylline
- · Surgical cervical sympathectomy
- · Anti biotics
- · Cyclophosphamide
- · Dialysis in CRF.
Management Treatment of Systemic Sclerosis —-
There is no specific therapy. General supportive therapy is indicated. A great number of drugs including corticosteroids, vasodilators, d-penicillamine, and immunosuppressive agents have been tried
- Alveolitis: Immunosuppressants and alkylating agents (e.g., cyclophosphamide)
- Angiotensin-converting enzyme inhibitors for preservation of renal blood flow and for treatment of hypertensive renal crisis
- Antacids, proton pump inhibitors: For gastric reflux
- Antibiotics: For secondary infections in bowel and active skin infections
- Avoidance of caffeine, nicotine, and sympathomimetics may ease Raynaud symptoms.
- Consider immunosuppressives for treatment of life-threatening or potentially crippling scleroderma or interstitial pneumonitis.
- Corticosteroids: For disabling myositis, pulmonary alveolitis, or mixed connective tissue disease (not recommended in high doses owing to increased incidence of renal failure)
- Dipyridamole or aspirin: Antiplatelet therapy
- Hydrophilic skin ointments: Skin therapy
- Intestinal dysfunction: Metoclopramide
- Nitrates and dihydropyridine calcium channel blockers for Raynaud phenomenon
- NSAIDs: For joint or tendon symptoms
- PDE-5 antagonists (e.g., sildenafil), prostanoids, and endothelin-1 antagonists are changing management of pulmonary hypertension.
- Penicillamine: To reduce skin thickening and delay the rate of new visceral involvement (use is now controversial; newer therapies such as relaxin may be better)
- Precautions/contraindications/interactions: Refer to the manufacturer’s literature for each drug.
- Topical clindamycin, erythromycin, or silver sulfadiazine cream may prevent recurrent infectious cutaneous ulcers.
Additional Therapies
- Physical therapy to maintain function and promote strength
- Heat therapy to relieve joint stiffness
