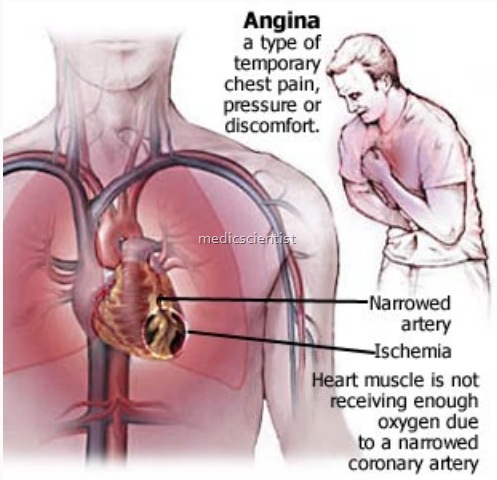
Clinical features of Unstable Angina(UA) / NSTEMI —
- There is chest pain in the substernal lesion or epigastrium radiating to neck, left shoulder and left arm.
- There is severe discomfort or pain.
- Anginal equivalents like dyspnoea and epigastric discomfort are also frequently present.
- There is diaphoresis (increased sweating), pale skin, sinus tachycardia, third and fourth heart sound, basilar rales or crepts, sometime hypotension.
ECG Unstable Angina(UA) / NSTEMI —
- There is ST segment depression
- Rarely there is transient ST segment elevation
- There may be T inversions
- Any new ST segment changes like depression of even 0.05 mV may denote increasing severity.
- New deep T wave inversions (more than 0.3 mV) may be significant, but usually T wave changes are nonspecific.
Cardiac Biomarkers Unstable Angina(UA) / NSTEMI
- CK-MB and troponin (highly specific) are elevated in MI and associated with increased risk of death.
- 7In UA the cardiac biomarkers are not elevated.
- In NSTEMI the cardiac biomarkers are elevated. Minor elevations of troponin can occur in heart failure, myocarditis, pulmonary embolism
- or may be false positive. Therefore it is suggested that when the presentation is of ACS only then troponin test may be done.
- New cardiac markers are C-reactive protein, BNP (B type nitriuretic peptide, CD-40 ligand etc. )
Diagnosis of Unstable Angina(UA) / NSTEMI
- The diagnosis is established by typical ischemic discomfort, history of CAD, old angiography, old MI, ECG changes, elevated cardiac biomarkers like troponin stress testing.
- IQhe cardiac markers are negative on admission then it may be repeated at 6 and 12 hours after presentation.
- AII the patient with elevated cardiac markers and ECG changes should be admitted to the hospital.
- If the patient is pain free and the markers are negative then patient should undergo stress testing in 72 hours. For atients who cannot walk, Dobutamine stress test should be done (non-exercise or- pharmacologicaI stress test). –
- Echocardiography should also be done for most patients.
- For myocardial perfusion, sestamibi or thallium imaging is done. This test shows whether there is myocardial damage and non-viable myocardial.
