Malaria and Babesiosis (protozoan )Signs and Symptoms Clinical findings with Diagnosis Treatment Malaria is a protozoan disease.
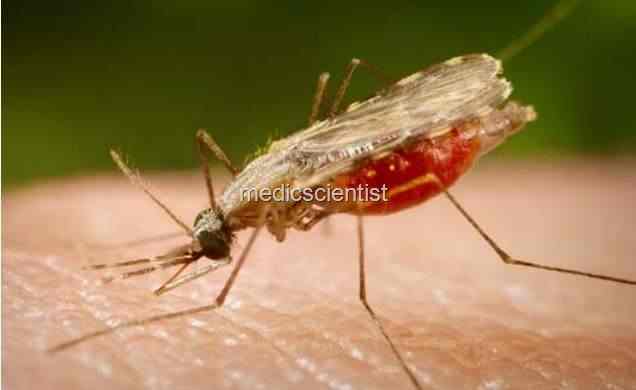 |
| Transmission is by bite of infected Anopheles mosquito |
Transmission is by bite of infected Anopheles mosquito.
- There are 4 species of the genus Plasmodium causing malaria.
- · P. falciparum
- · P. vivax
- · P. ovale
- · P. malariae.
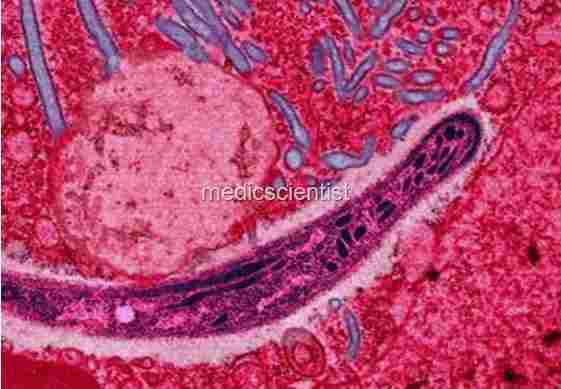 |
| Malaria is a protozoan disease |
Death in malaria is due to
- P. falciparum infection.
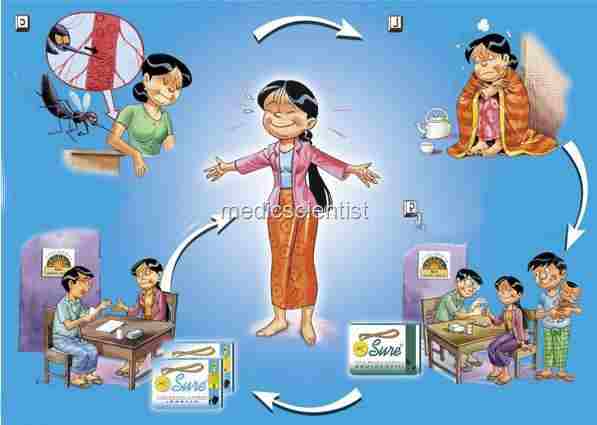
- Female anopheles mosquito has sporozoites of Plasmodium in the salivary glands. Sporozoites are transferred to man when the mosquito bites a man.
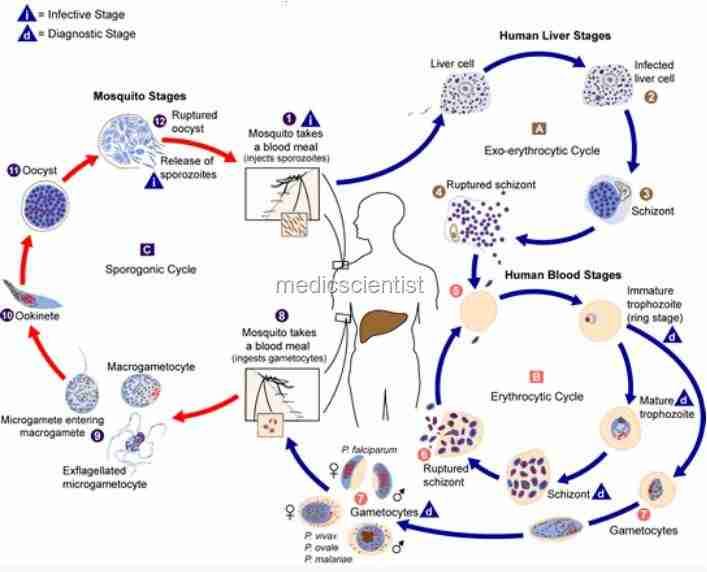 |
| Malaria is a protozoan disease Life cycle |
These sporozoites which are motile are carried to the liver via the bloodstream.
- In the liver, the sporozoites invade the hepatic cells and begin asexual reproduction. This multiplication of the sporozoites in liver cells is called intrahepatic or preerythrocytic schizogony or merogony.
- Thus a single sporozoite can produce more then– 10,000 merozoites. The liver cell swells and bursts and motile merozoites are discharged into the blood stream. These invade the RBC’s and multiply 20 times every 2-3 days. When these are about SO/IJL of blood, then symptoms begin.
- In P. vivax and P. ovale there are dormant or resting forms which stay in the liver from 3 weeks to a year or longer. They can multiply at any time and cause relapses. These dormant forms are called hypnozoites.
Merozoites enter the blood stream from the liver and invade (enter) RBC’s and become trophozoites.
- In people with Duffy blood group negative (No FyFy antigen) there is resistance to P. vivax malaria.
- In the RBCs, the trophozoites are seen as ring forms. Then the trophozoite becomes amoebae-shaped.
- By 48 hours (vivax) or 72 (malariae) hours, the trophozoite consumes all the hemoglobin and occupies most of the RBC. It is now a schizont which divides into daughter merozoites.
- RBC ruptures and 6 to 30 daughter merozoites are released in the blood. These can invade fresh RBC’s.
- After several asexual cycles as in P. falciparum or soon after release from liver as in P. vivax, ovale, malariae, some of the parasites change into gametocytes.
- The male and female gametocytes are sucked with blood by the bite of the Anopheles mosquito.
- The male and female gametocytes form a zygote in the gut of the mosquito. The zygote changes to an oocyst.
- The oocyst bursts to liberate sporozoites which migrate to the salivary gland of the mosquito. When the mosquito bites another human being then the parasite is inoculated into that person, and the cycle begins again.
- The parasite degrades hemoglobin, and deforms the RBC.
- P. vivax, P. ovale and P. malariae produce lower levels of parasitemia <2% but P. falciparum infects RBCs of all ages and produces high levels of parasitemia.
- The parasites may persist in the blood for many months.
- P. malariae persists in the blood for many years, if treatment is not given.
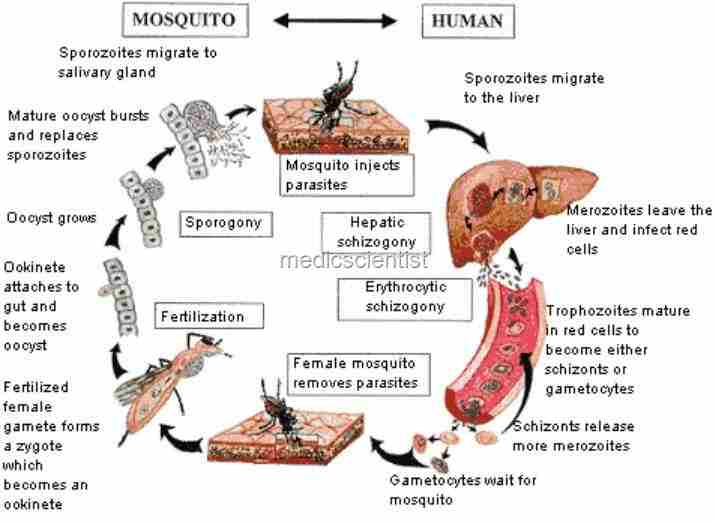 |
| Malaria is a protozoan disease lifecycle |
Epidemiology Malaria
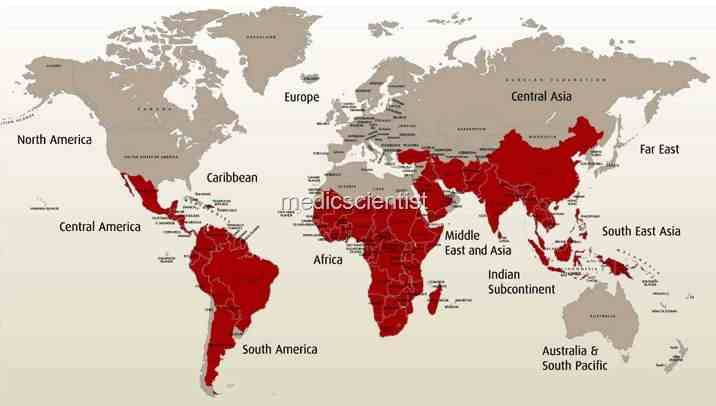 |
| Epidemiology Malaria |
- Malaria is a disease of tropical countries. P. falciparum is found in Africa and India. P. vivax is very common in India.
- P. malariae is found in Africa, rare in India P. ovale is found only in Africa.
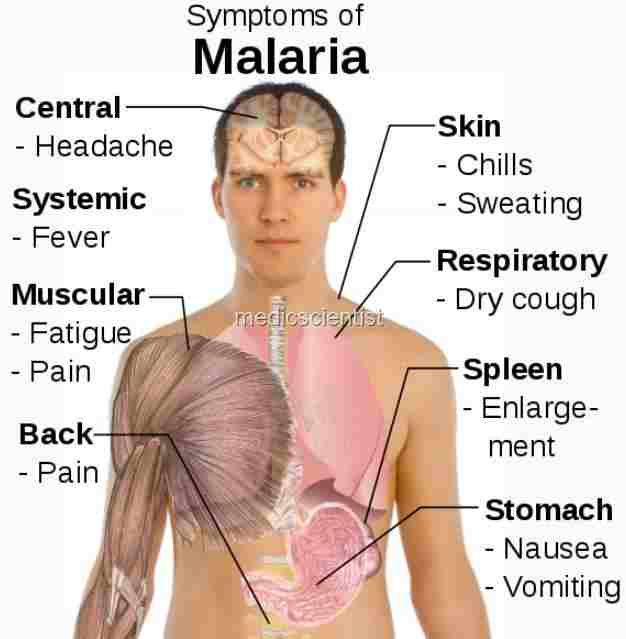 |
| Malaria Fever Clinical FeaturesSymptoms |
Malaria Fever Clinical Features Symptoms
- · Fever
- · Headache
- · Fatigue
- · Abdominal discomfort
- · Muscle aches-due to fever and rigors
- · Nausea and vomiting
- · Orthostatic hypotension
- · Classical fever has spikes, chills, rigors at regular intervals as in infection with P. vivax or P.ovale. The fever is irregular at first.
- · In children, there may be fever above 400C with tachycardia and delirium.
- · In Falciparum malaria there may be febrile convulsions.
Malaria Fever Physical signs
- · Fever
- · Anaemia
- · Splenomegaly
- · Hepatomegaly
- · Mild jaundice
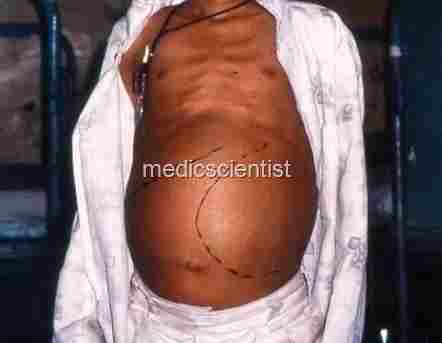 |
| Malaria Fever TROPICAL SPLENOMEGALY |
Malaria Fever TROPICAL SPLENOMEGALY Characterized by :
- Chronic malaria,
- Hypergammaglobulinaemia,
- Abnormal immune responses,
- Normocytic normochromic anaemia,
- Splenomegaly, Hepatomegaly,
- Dragging pain in abdomen,
- Pancytopenia,
- Sometimes death due to sepsis.
QUARTAN MALARIAL NEPHROPATHY
- P. malariae infections may cause immune complex injury to renal glomeruli resulting in nephrotic syndrome.
- There are basement membrane deposits. Mortality may be high.
- Burkitt’s Lymphoma and Epstein-Barr virus infection are more common in malaria infested Africa.
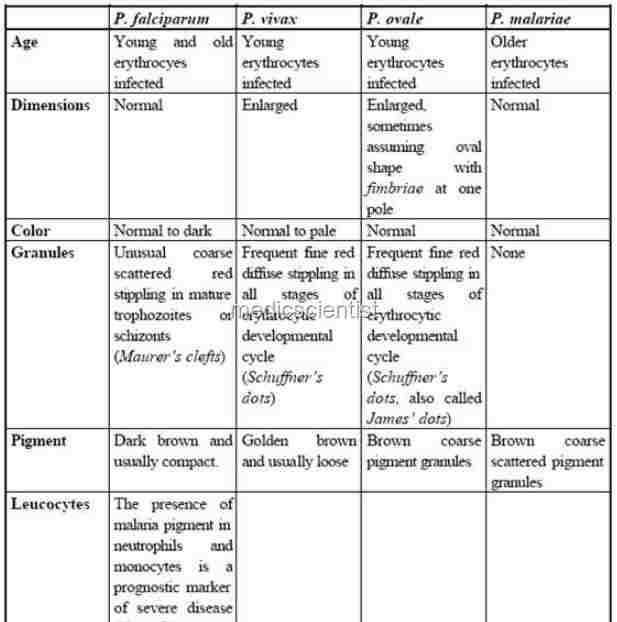 |
| Malaria Fever DIAGNOSIS OF MALARIA |
Malaria Fever DIAGNOSIS OF MALARIA
- Asexual forms of the parasite can be seen in peripheral blood smears.
- Thin and thick smears can be stained with Giemsa or Leishman’s stain.
- Level of parasitemia is denoted by number of parasitized RBCs per 1000 RBCs or per 200 WBCs.
- It is expressed as parasitized RBCs per IJL.
- Other tests are antibody-based diagnostic stick or card tests.
- More than 20% of parasites with visible pigment in falciparum malaria has a very poor prognosis.
- Thick blood film of uneven thickness shows concentration of parasites.
- Staining of parasites with acridine orange is done for rapid diagnosis in patients with low level parasitemia.
- Thick and thin smears are prepared to confirm the diagnosis.
- Smear examination is repeated every 12 hours. Rapid diagnostic tests are acridine orange staining and QBC test.
Malaria Fever Lab findings
- · Normocytic, normochromic anaemia
- · ESR, CRP(C-reactive protein) is increased
- · Platelet count may be reduced
- · PT and APn are prolonged
- · Metabolic acidosis
- · Hypoglycemia and Hyponatremia
- · Jaundice
- · Hypergammaglobulinemia.
 |
| Malaria Fever TREATMENT |
Malaria Fever TREATMENT
- In area with high transmission of malaria, all cases of fever should be treated for malaria.
- When there is doubt about the species, treatment for falciparum malaria is given.
- Drug of choice is chloroquine.
- Quinine is used for resistant malaria. Chloroquine and Quinine tablets are available but parenteral therapy is given for serious patients.
- Other drugs which are safe and effective against resistant falciparum malaria are artemisinin (Artemether and Artesunate).
- These can be given by IV or 1M injection.
- Severe Falciparum malaria is an emergency and may need ICU care, glucocorticoids anticonvulsants, and hemodialysis.
- Travelers should take antimalarial drugs one week before departure, and continue for 4 weeks after leaving the malarial area.
- Mefloquine – 250 mg weekly is used as prophylactic agent.
Doses of Antimalarial Drugs
- . Chloroquine – 10 mg of base /kg followed by 10 mg/kg at 24 hand 5 mgjkg at 48 h.
- . Sulfadoxine j Pyrimethamine – 25/1.25 mg/kg single oral dose (3 tablets for adults).
- . Mefloquine – 15 mg/kg followed 8-12 h later by second dose of 10 mgjkg.
- . Quinine- 10 mg of salt jkg every 8 hours for 7days combined with tetracycline (4 mgjkg qid).
- . Artesunate 12 mg/kg given in divided doses over 3-5 days e.g. 4 mg/kg for 3 days in combination with 25 mg of mefloquine/kg.
- . Artemether – 3.2 mg/kg 1M stat followed by 1.6 mg/kg per day.
- . Atovaquone + Proguanil – adults of >40 kg, each dose comprises 4 tablets (each tablet containing Atovaquone 250 mg and Proguanil 100 mg) taken once daily for 3 days with food.
- . Lumefantrine + Artemether.
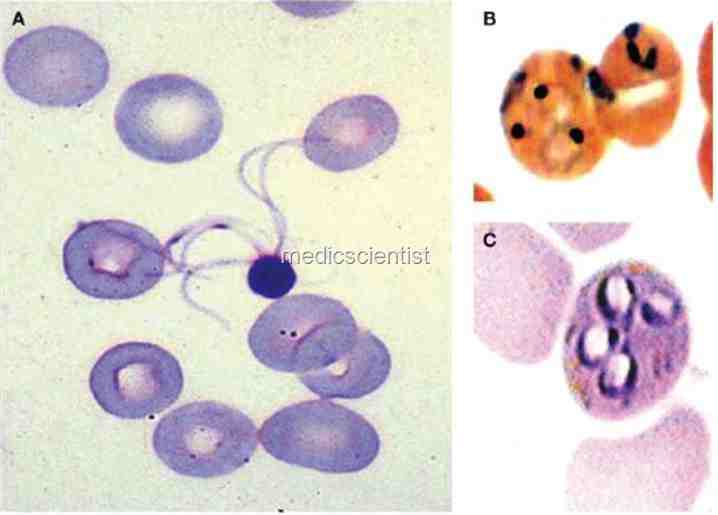 |
| Malaria and Babesiosis (protozoan ) a,b- Malaria c-Babsiosis |
- The disease is transmitted by deer ticks, and occurs most often in New England in the U.S. It has also been reported elsewhere.
- A rare, usually self-limited disease caused by an intraerythrocytic protozoan, Babesia microti, and perhaps other Babesia species.
- Severe forms are most likely to occur in elderly people and in people without functioning spleens.
- Rarely, the infection is transmitted by blood transfusion from an asymptomatic carrier
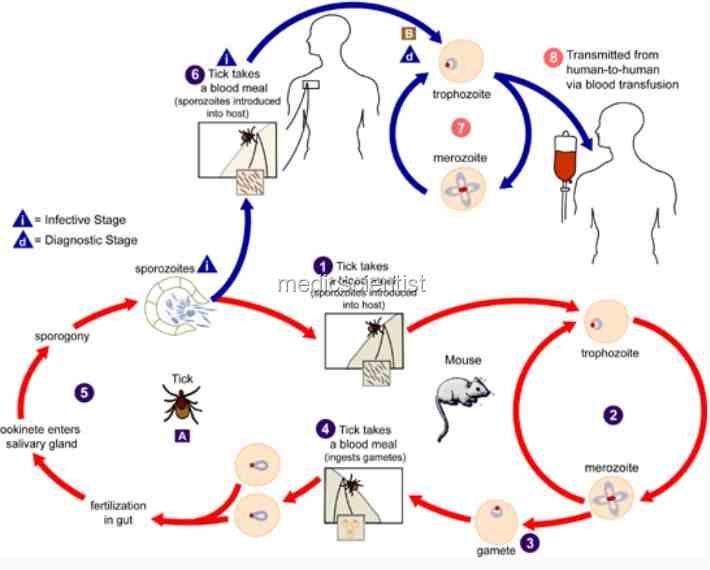 |
| BABESIOSIS lifecycle |
- This is a protozoan disease of animals transmitted by ticks. Humans are accidentally infected.
- There is fever with chills, sweating, muscle pain, and fatigue.
- There is hemolytic anaemia and hepatosplenomegaly. Babesia organisms enter the RBCs like malarial parasite.
BABESIOSIS Diagnosis —
- The diagnosis is suggested when a patient with an appropriate outdoor exposure presents with typical symptoms,some time plus hemolytic anemia.
- Thick and thin blood smears and other laboratory techniques (e.g., the polymerase chain reaction) may be used for definitive confirmation.
BABESIOSIS Treatment
- May not be required as the disease is often selflimiting.
- Symptoms may persist for months.
- Quinine, Clindamycin and Atovaquone are effective.
