Article Contents ::
- 1 Systemic Sclerosis (Scleroderma)
- 2 Diffuse cutaneous scleroderma
- 3 Limited cutaneous scleroderma
- 4 Systemic sclerosis sine scleroderma
- 5 en Coup de saber
- 6 Mixed connective tissue disease (MCTD)
- 7 Classification of localized scleroderma
- 8 Classification of systemic sclerosis
- 9 Systemic Sclerosis Epidemiology
- 10 Systemic Sclerosis Pathology
- 11 Systemic Sclerosis Prognosis
- 12 Systemic Sclerosis Complications
Systemic Sclerosis (Scleroderma)
- Systemic Sclerosis Classification Epidemiology Pathology Prognosis and Complications
It is a chronic multisystem disorder. There is thickening of the skin due to accumulation of connective tissue affecting the structure and function of gastrointestinal system (GIT), lungs, heart, kidneys and other organs. There is vascular damage, and other immune processes resulting in damage of connective tissues. Skin and internal organs are involved to different extents.
Diffuse cutaneous scleroderma
- There is symmetric skin thickening of upper and lower limbs, face and trunk.
- Kidney may be inyolved.
Limited cutaneous scleroderma
- There is symmetric skin thickening of distal extremities a nd face.
- Features of CREST syndrome are present – calcinosis, Raynaud’s phenomenon, oesophageal dysmotility, sclerodactyly, telangiectasia.
- There is pulmonary arterial hypertension. Biliary cirrhosis.
Systemic sclerosis sine scleroderma
- There is systemic sclerosis without any skin involvement.
- Localized scleroderma, occurs in young women and children.
en Coup de saber
- There is a linear scleroderma of face on the forehead with hemiatrophy of the same side of face.
- The linear lesion resembles a wound from a sword, hence called en coup de saber.
Mixed connective tissue disease (MCTD)
- There is SLE, scleroderma, polymyositis, rheumatoid arthritis, high titres of RNP (ribonucleo protein).
- There is eosinophilia myalgia syndrome.
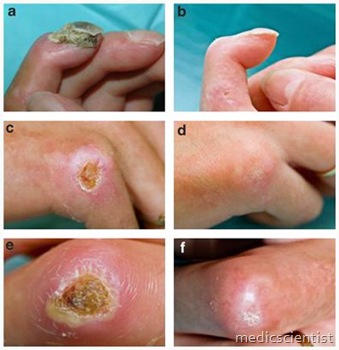
Classification of localized scleroderma
- Bullous morphea Bullous involvement May occur in other forms of localized scleroderma
- Deep morphea Least common form of localized scleroderma in children Most disabling form of localized scleroderma Primary site of involvement is the panniculus (subcutaneous tissue)
- Generalized morphea Multiple plaques that are confluent or affect three or more anatomic sites Often located on the trunk or limbs Similar clinical and histologic features as plaque morphea
- Linear scleroderma Most common form of localized scleroderma in children One or more elongated sclerotic areas of skin Lesions are typically asymmetric and oriented along the affected limb Associated with growth impairment of the involved extremity Lesions on the face or scalp are called en coup de sabre
- Plaque morphea One or more circumscribed patches of skin with sclerotic changes in two or less anatomic sites Involvement is confined to the superificial panniculus (subcutaneous tissue)
Classification of systemic sclerosis
- Diffuse cutaneous scleroderma Raynaud’s phenomenon followed, within one year, by puffy or hidebound skin changes Truncal and acral skin involvement; tendon friction rubs Nailfold capillary dilatation and capillary drop-out Early and significant incidence of renal, interstitial lung, diffuse gastrointestinal, and myocardial disease Anti-Scl-70 (30 percent) and anti-RNA polymerase-I, II, or III (12 to 15 percent) antibodies
- Environmentally induced scleroderma Generally diffuse distribution of skin sclerosis and a history of exposure to an environmental agent suspected of causing scleroderma
- Limited cutaneous scleroderma Raynaud’s phenomenon for years, occasionally decades Skin involvement limited to hands, face, feet, and forearms (acral distribution) Dilated nailfold capillary loops, usually without capillary drop-out A significant (10 to 15 percent) late incidence of pulmonary hypertension, with or without skin calcification, gastrointestinal disease, telangiectasias (CREST syndrome), or interstitial lung disease Renal disease rarely occurs Anticentromere antibody (ACA) in 70 to 80 percent
- Overlap syndromes Features of systemic sclerosis which coexist with those of another autoimmune rheumatic disease such as systemic lupus erythematosus, rheumatoid arthritis, dermatomyositis, vasculitis, or Sjögren’s syndrome.
- Pre-scleroderma Raynaud’s phenomenon Nailfold capillary changes and evidence of digital ischemia Specific circulating autoantibodies – anti-topoisomerase-I (Scl-70), anti-centromere (ACA), or anti-RNA polymerase-I, II, or III
- Scleroderma sine scleroderma Presentation with pulmonary fibrosis or renal, cardiac, or gastrointestinal disease No skin involvement Raynaud’s phenomenon may be present Antinuclear antibodies may be present – anti-Scl-70, ACA, or anti-RNA polymerase-I, II, or III
Systemic Sclerosis Epidemiology
- Predominant age:
- Young adult (16–40 years); middle-aged (40–75 years), peak onset 30–50 years
- Symptoms usually appear in the 3rd–5th decades.
- Predominant sex: Female > Male (4:1)
- · Most common in 3rd to 5thdecade.
- · More common in women.
- · Antinuclear antibodies (ANA), Human leucocyte antigen (HLAL Anticentromere antibodies (ACA) are all associated with the disease.
- · It is more common in coal and gold miners.
- · On ingestion of rapeseed oil, mixed in cooking oil, a scleroderma-like syndrome develops with the following features:
- – Interstitial pneumonitis
- – Eosinophilia
- – Arthralgias
- – Arthritis
- – Myositis
- – Skin thickening
- – Raynaud’s phenomenon
- – Pulmonary hypertension
- – Resorption of digits.
- · It can also occur due to silicon breast implants.
Systemic Sclerosis Pathology
- There is accumulation of collagen and other extracellular matrix proteins.
- Immunologic mechanisms are involved.
- There is vascular injury to blood vessels of skin, GIT, kidneys, heart and lungs.
Systemic Sclerosis Prognosis
- Possible improvement, but incurable
- Prognosis is poor if cardiac, pulmonary, or renal manifestations present early.
Systemic Sclerosis Complications
- Arrhythmia
- Cardiomyopathy
- Death
- Disability
- Esophageal dysmotility
- Flexion contractures
- Megacolon
- Obstructive bowel
- Pneumatosis intestinalis
- Possible association with lung and other cancers
- Pulmonary hypertension
- Reflux esophagitis
- Renal failure
- Respiratory failure
