Article Contents ::
- 1 Details About Generic Salt :: Perphena
- 2 Main Medicine Class:: Antipsychotic,Phenothiazine,Antiemetic
- 3
(per-FEN-uh-zeen)
Trilafon, Apo-Perphenazine, Phenazine, PMS-Perphenazine
Class: Antipsychotic/Phenothiazine/Antiemetic
Action Effects apparently caused by postsynaptic dopamine receptor blockade in CNS.
Indications Management of psychotic disorders; control of severe nausea/vomiting; intractable hiccoughs in adults. Unlabeled use(s): Treatment of Tourette’s syndrome; control of acute agitation in elderly; useful in controlling some symptoms of dementia such as agitation, hyperactivity, hallucinations, suspiciousness, hostility and uncooperative behaviors; treatment of hemiballismus (violent writhing/movement of one side of body).
Contraindications Comatose or severely depressed states; allergy to any phenothiazine; presence of large amounts of other CNS depressants; bone marrow depression or blood dyscrasias; liver damage; subcortical brain damage.
Route/Dosage
Psychiatric
ADULT: Nonhospitalized patients: PO 4 to 8 mg tid, reduce as soon as possible to minimum effective dosage.
Hospitalized patients: PO 8 to 16 mg bid to qid; avoid dosages > 64 mg/day.
Nausea/Vomiting/Hiccoughs
ADULTS: PO 8–16 mg/day in divided doses. (Give elderly and debilitated patients lower doses. Administer to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
IM
Doses range from 5 to 10 mg/injection, usually given q 6 hr. Do not exceed 30 mg/day. Administer by deep injection to seated or recumbent patient. IM administration usually reserved for instances in which patient is unwilling or unable to take oral medication.
ORAL LIQUID CONCENTRATE AND IV FORM
See Administration/Storage.
Interactions
Alcohol: May result in increased CNS depression and may precipitate extrapyramidal reaction. Anticholinergics: May reduce therapeutic effects of perphenazine and worsen anticholinergic effects. Concomitant administration may worsen schizophrenic symptoms and lead to tardive dyskinesia (see Precautions). Barbiturate anesthetics: Frequency and severity of neuromuscular excitation and hypotension may increase. Guanethidine: Hypotensive action of guanethidine may be inhibited. Metrizamide: Possibility of seizure may be increased when subarachnoid metrizamide injection is used.
Lab Test Interferences May discolor urine pink to red-brown. False-positive pregnancy tests may occur but are less likely to occur with serum test. Increases in protein-bound iodine have been reported.
Adverse Reactions
CV: Orthostatic hypotension; hypertension; tachycardia; bradycardia; syncope; cardiac arrest; circulatory collapse; lightheadedness; faintness; dizziness; ECG changes. CNS: Pseudoparkinsonism dystonia; dyskinesia, motor restlessness; oculogyric crisis; dystonias; hyperreflexia; tardive dyskinesia; drowsiness; headache; fatigue; abnormalities of the cerebrospinal fluid proteins; paradoxical excitement or exacerbation of psychotic symptoms; catatonic-like states; weakness; tremor; paranoid reactions; lethargy; seizures; hyperactivity; nocturnal confusion; bizarre dreams; vertigo; insomnia. DERM: Photosensitivity; skin pigmentation; dry skin; exfoliative dermatitis; urticarial rash; maculopapular hypersensitivity reaction; seborrhea; eczema. EENT: Pigmentary retinopathy; glaucoma; photophobia; blurred vision; mydriasis; increased intraocular pressure; dry mouth or throat; nasal congestion. GI: Dyspepsia; adynamic ileus (may result in death); nausea; vomiting; constipation. GU: Urinary hesitancy or retention; impotence; sexual dysfunction; menstrual irregularities. HEMA: Agranulocytosis; eosinophilia; leukopenia; hemolytic anemia; thrombocytopenic purpura. HEPA: Jaundice. META: Hyperglycemia; hypoglycemia; decreased cholesterol. RESP: Laryngospasm; bronchospasm; dyspnea. OTHER: Increases in appetite and weight; polydipsia; breast enlargement; galactorrhea; increased prolactin levels.
Precautions
Pregnancy: Pregnancy category undetermined. Lactation: Undetermined. Children: Not recommended in children < 12 yr. Elderly: More susceptible to effects; consider lower dose. Special-risk patients: Use caution in patients with cardiovascular disease or mitral insufficiency, history of glaucoma, EEG abnormalities or seizure disorders, prior brain damage, hepatic or renal impairment. Antiemetic effects: Because of suppression of cough reflex, aspiration of vomitus possible. CNS effects: May impair mental or physical abilities, especially during first few days of therapy. Hepatic effects: Jaundice usually occurs between second and fourth weeks of treatment; considered hypersensitivity reaction. Usually reversible. Neuroleptic malignant syndrome: Has occurred with agents of this class; is potentially fatal. Signs and symptoms are hyperpyrexia, muscle rigidity, altered mental status, irregular pulse, irregular blood pressure, tachycardia, and diaphoresis. Pulmonary: Cases of bronchopneumonia, some fatal, have occurred. Sudden death: Has been reported; predisposing factors may be seizures or previous brain damage. Flare-ups of psychotic behavior may precede death. Tardive dyskinesia: Syndrome of potentially irreversible involuntary body and facial movements may develop. Prevalence highest in elderly, especially women. Use smallest effective doses for shortest possible time period.
PATIENT CARE CONSIDERATIONS
Administration/Storage
Administer tablets with meals or with full glass of milk or water.
Protect from light.
Oral Liquid Concentrate
Dilute just prior to administration in 60 ml of one of following diluents: Water, saline, homogenized milk, carbonated orange beverage, and pineapple, apricot, prune, orange, V-8, tomato, or grapefruit juices.
Do not mix with caffeinated beverages or with drinks containing tannins (tea) or pectinates (apple juice), because physical incompatibilities may occur.
Shake concentrate before use.
Dilute each 5 ml of concentrate with at least 60 ml of fluid.
Protect from light; store at room temperature.
IV
Give as diluted solution by fractional injection of slow-drip infusion. Slow infusion method is preferred for surgical patients.
Dilute solution to 0.5 mg/ml (1 ml mixed with 9 ml of saline solution) and give £ 1 mg per injection at not less than 1 to 2 min intervals. Do not exceed 5 mg.
IM
Administer injectable form by deep IM to sitting or recumbent patients.
Assessment/Interventions
Obtain patient history, including drug history and any known allergies.
Monitor for potential signs of pseudoparkinsonism, dystonia, dyskinesia, or akathisia and report to physician.
Monitor for evidence of tardive dyskinesia (eg, involuntary dyskinetic movements of tongue, lip, mouth, face, or jaw), and report to physician.
Be alert for evidence of orthostatic hypotension; take orthostatic BP and report to physician.
Report any significant unexplained temperature increase to physician.
When coadministering anticholinergic drugs, be alert for possible decreased therapeutic effects of perphenazine and increased anticholinergic effects.
OVERDOSAGE: SIGNS & SYMPTOMS
CNS depression, hypotension, extrapyramidal symptoms, agitation, convulsions, fever, hypothermia, ECG changes, cardiac arrhythmias
Patient/Family Education
Instruct patient to report the following symptoms to physician: Dizziness, drooling, restlessness, tremors, stiffness, muscle spasms or involuntary face, tongue, mouth, or lip movements.
Caution patient to avoid sudden position changes to prevent orthostatic hypotension.
Instruct patient to avoid intake of alcoholic beverages or other CNS depressants.
Advise patient to use caution driving or performing other tasks requiring mental alertness.
Caution patient to avoid exposure to sunlight and to use sunscreen or wear protective clothing to avoid photosensitivity reaction.
- 4 Drugs Class ::
- 5 Disclaimer ::
- 6 The Information available on this site is for only Informational Purpose , before any use of this information please consult your Doctor .Price of the drugs indicated above may not match to real price due to many possible reasons may , including local taxes etc.. These are only approximate indicative prices of the drug.
Details About Generic Salt :: Perphena
| (per-FEN-uh-zeen) |
Trilafon,  Apo-Perphenazine, Phenazine, PMS-Perphenazine Apo-Perphenazine, Phenazine, PMS-Perphenazine |
| Class: Antipsychotic/Phenothiazine/Antiemetic |

Action Effects apparently caused by postsynaptic dopamine receptor blockade in CNS.

Indications Management of psychotic disorders; control of severe nausea/vomiting; intractable hiccoughs in adults. Unlabeled use(s): Treatment of Tourette’s syndrome; control of acute agitation in elderly; useful in controlling some symptoms of dementia such as agitation, hyperactivity, hallucinations, suspiciousness, hostility and uncooperative behaviors; treatment of hemiballismus (violent writhing/movement of one side of body).

Contraindications Comatose or severely depressed states; allergy to any phenothiazine; presence of large amounts of other CNS depressants; bone marrow depression or blood dyscrasias; liver damage; subcortical brain damage.

Route/Dosage
Psychiatric
ADULT: Nonhospitalized patients: PO 4 to 8 mg tid, reduce as soon as possible to minimum effective dosage.
Hospitalized patients: PO 8 to 16 mg bid to qid; avoid dosages > 64 mg/day.
Nausea/Vomiting/Hiccoughs
ADULTS: PO 8–16 mg/day in divided doses. (Give elderly and debilitated patients lower doses. Administer 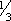 to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
IM
Doses range from 5 to 10 mg/injection, usually given q 6 hr. Do not exceed 30 mg/day. Administer by deep injection to seated or recumbent patient. IM administration usually reserved for instances in which patient is unwilling or unable to take oral medication.
ORAL LIQUID CONCENTRATE AND IV FORM
See Administration/Storage.

Interactions
Alcohol: May result in increased CNS depression and may precipitate extrapyramidal reaction. Anticholinergics: May reduce therapeutic effects of perphenazine and worsen anticholinergic effects. Concomitant administration may worsen schizophrenic symptoms and lead to tardive dyskinesia (see Precautions). Barbiturate anesthetics: Frequency and severity of neuromuscular excitation and hypotension may increase. Guanethidine: Hypotensive action of guanethidine may be inhibited. Metrizamide: Possibility of seizure may be increased when subarachnoid metrizamide injection is used.

Lab Test Interferences May discolor urine pink to red-brown. False-positive pregnancy tests may occur but are less likely to occur with serum test. Increases in protein-bound iodine have been reported.

Adverse Reactions
CV: Orthostatic hypotension; hypertension; tachycardia; bradycardia; syncope; cardiac arrest; circulatory collapse; lightheadedness; faintness; dizziness; ECG changes. CNS: Pseudoparkinsonism dystonia; dyskinesia, motor restlessness; oculogyric crisis; dystonias; hyperreflexia; tardive dyskinesia; drowsiness; headache; fatigue; abnormalities of the cerebrospinal fluid proteins; paradoxical excitement or exacerbation of psychotic symptoms; catatonic-like states; weakness; tremor; paranoid reactions; lethargy; seizures; hyperactivity; nocturnal confusion; bizarre dreams; vertigo; insomnia. DERM: Photosensitivity; skin pigmentation; dry skin; exfoliative dermatitis; urticarial rash; maculopapular hypersensitivity reaction; seborrhea; eczema. EENT: Pigmentary retinopathy; glaucoma; photophobia; blurred vision; mydriasis; increased intraocular pressure; dry mouth or throat; nasal congestion. GI: Dyspepsia; adynamic ileus (may result in death); nausea; vomiting; constipation. GU: Urinary hesitancy or retention; impotence; sexual dysfunction; menstrual irregularities. HEMA: Agranulocytosis; eosinophilia; leukopenia; hemolytic anemia; thrombocytopenic purpura. HEPA: Jaundice. META: Hyperglycemia; hypoglycemia; decreased cholesterol. RESP: Laryngospasm; bronchospasm; dyspnea. OTHER: Increases in appetite and weight; polydipsia; breast enlargement; galactorrhea; increased prolactin levels.

Precautions
Pregnancy: Pregnancy category undetermined. Lactation: Undetermined. Children: Not recommended in children < 12 yr. Elderly: More susceptible to effects; consider lower dose. Special-risk patients: Use caution in patients with cardiovascular disease or mitral insufficiency, history of glaucoma, EEG abnormalities or seizure disorders, prior brain damage, hepatic or renal impairment. Antiemetic effects: Because of suppression of cough reflex, aspiration of vomitus possible. CNS effects: May impair mental or physical abilities, especially during first few days of therapy. Hepatic effects: Jaundice usually occurs between second and fourth weeks of treatment; considered hypersensitivity reaction. Usually reversible. Neuroleptic malignant syndrome: Has occurred with agents of this class; is potentially fatal. Signs and symptoms are hyperpyrexia, muscle rigidity, altered mental status, irregular pulse, irregular blood pressure, tachycardia, and diaphoresis. Pulmonary: Cases of bronchopneumonia, some fatal, have occurred. Sudden death: Has been reported; predisposing factors may be seizures or previous brain damage. Flare-ups of psychotic behavior may precede death. Tardive dyskinesia: Syndrome of potentially irreversible involuntary body and facial movements may develop. Prevalence highest in elderly, especially women. Use smallest effective doses for shortest possible time period.
|
PATIENT CARE CONSIDERATIONS |
|

Administration/Storage
- Administer tablets with meals or with full glass of milk or water.
- Protect from light.
Oral Liquid Concentrate
- Dilute just prior to administration in 60 ml of one of following diluents: Water, saline, homogenized milk, carbonated orange beverage, and pineapple, apricot, prune, orange, V-8, tomato, or grapefruit juices.
- Do not mix with caffeinated beverages or with drinks containing tannins (tea) or pectinates (apple juice), because physical incompatibilities may occur.
- Shake concentrate before use.
- Dilute each 5 ml of concentrate with at least 60 ml of fluid.
- Protect from light; store at room temperature.
IV
- Give as diluted solution by fractional injection of slow-drip infusion. Slow infusion method is preferred for surgical patients.
- Dilute solution to 0.5 mg/ml (1 ml mixed with 9 ml of saline solution) and give £ 1 mg per injection at not less than 1 to 2 min intervals. Do not exceed 5 mg.
IM
- Administer injectable form by deep IM to sitting or recumbent patients.

Assessment/Interventions
- Obtain patient history, including drug history and any known allergies.
- Monitor for potential signs of pseudoparkinsonism, dystonia, dyskinesia, or akathisia and report to physician.
- Monitor for evidence of tardive dyskinesia (eg, involuntary dyskinetic movements of tongue, lip, mouth, face, or jaw), and report to physician.
- Be alert for evidence of orthostatic hypotension; take orthostatic BP and report to physician.
- Report any significant unexplained temperature increase to physician.
- When coadministering anticholinergic drugs, be alert for possible decreased therapeutic effects of perphenazine and increased anticholinergic effects.
| OVERDOSAGE: SIGNS & SYMPTOMS |
| |
CNS depression, hypotension, extrapyramidal symptoms, agitation, convulsions, fever, hypothermia, ECG changes, cardiac arrhythmias |
|

Patient/Family Education
- Instruct patient to report the following symptoms to physician: Dizziness, drooling, restlessness, tremors, stiffness, muscle spasms or involuntary face, tongue, mouth, or lip movements.
- Caution patient to avoid sudden position changes to prevent orthostatic hypotension.
- Instruct patient to avoid intake of alcoholic beverages or other CNS depressants.
- Advise patient to use caution driving or performing other tasks requiring mental alertness.
- Caution patient to avoid exposure to sunlight and to use sunscreen or wear protective clothing to avoid photosensitivity reaction.
Drugs Class ::
| (per-FEN-uh-zeen) |
Trilafon,  Apo-Perphenazine, Phenazine, PMS-Perphenazine Apo-Perphenazine, Phenazine, PMS-Perphenazine |
| Class: Antipsychotic/Phenothiazine/Antiemetic |

Action Effects apparently caused by postsynaptic dopamine receptor blockade in CNS.

Indications Management of psychotic disorders; control of severe nausea/vomiting; intractable hiccoughs in adults. Unlabeled use(s): Treatment of Tourette’s syndrome; control of acute agitation in elderly; useful in controlling some symptoms of dementia such as agitation, hyperactivity, hallucinations, suspiciousness, hostility and uncooperative behaviors; treatment of hemiballismus (violent writhing/movement of one side of body).

Contraindications Comatose or severely depressed states; allergy to any phenothiazine; presence of large amounts of other CNS depressants; bone marrow depression or blood dyscrasias; liver damage; subcortical brain damage.

Route/Dosage
Psychiatric
ADULT: Nonhospitalized patients: PO 4 to 8 mg tid, reduce as soon as possible to minimum effective dosage.
Hospitalized patients: PO 8 to 16 mg bid to qid; avoid dosages > 64 mg/day.
Nausea/Vomiting/Hiccoughs
ADULTS: PO 8–16 mg/day in divided doses. (Give elderly and debilitated patients lower doses. Administer 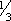 to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
IM
Doses range from 5 to 10 mg/injection, usually given q 6 hr. Do not exceed 30 mg/day. Administer by deep injection to seated or recumbent patient. IM administration usually reserved for instances in which patient is unwilling or unable to take oral medication.
ORAL LIQUID CONCENTRATE AND IV FORM
See Administration/Storage.

Interactions
Alcohol: May result in increased CNS depression and may precipitate extrapyramidal reaction. Anticholinergics: May reduce therapeutic effects of perphenazine and worsen anticholinergic effects. Concomitant administration may worsen schizophrenic symptoms and lead to tardive dyskinesia (see Precautions). Barbiturate anesthetics: Frequency and severity of neuromuscular excitation and hypotension may increase. Guanethidine: Hypotensive action of guanethidine may be inhibited. Metrizamide: Possibility of seizure may be increased when subarachnoid metrizamide injection is used.

Lab Test Interferences May discolor urine pink to red-brown. False-positive pregnancy tests may occur but are less likely to occur with serum test. Increases in protein-bound iodine have been reported.

Adverse Reactions
CV: Orthostatic hypotension; hypertension; tachycardia; bradycardia; syncope; cardiac arrest; circulatory collapse; lightheadedness; faintness; dizziness; ECG changes. CNS: Pseudoparkinsonism dystonia; dyskinesia, motor restlessness; oculogyric crisis; dystonias; hyperreflexia; tardive dyskinesia; drowsiness; headache; fatigue; abnormalities of the cerebrospinal fluid proteins; paradoxical excitement or exacerbation of psychotic symptoms; catatonic-like states; weakness; tremor; paranoid reactions; lethargy; seizures; hyperactivity; nocturnal confusion; bizarre dreams; vertigo; insomnia. DERM: Photosensitivity; skin pigmentation; dry skin; exfoliative dermatitis; urticarial rash; maculopapular hypersensitivity reaction; seborrhea; eczema. EENT: Pigmentary retinopathy; glaucoma; photophobia; blurred vision; mydriasis; increased intraocular pressure; dry mouth or throat; nasal congestion. GI: Dyspepsia; adynamic ileus (may result in death); nausea; vomiting; constipation. GU: Urinary hesitancy or retention; impotence; sexual dysfunction; menstrual irregularities. HEMA: Agranulocytosis; eosinophilia; leukopenia; hemolytic anemia; thrombocytopenic purpura. HEPA: Jaundice. META: Hyperglycemia; hypoglycemia; decreased cholesterol. RESP: Laryngospasm; bronchospasm; dyspnea. OTHER: Increases in appetite and weight; polydipsia; breast enlargement; galactorrhea; increased prolactin levels.

Precautions
Pregnancy: Pregnancy category undetermined. Lactation: Undetermined. Children: Not recommended in children < 12 yr. Elderly: More susceptible to effects; consider lower dose. Special-risk patients: Use caution in patients with cardiovascular disease or mitral insufficiency, history of glaucoma, EEG abnormalities or seizure disorders, prior brain damage, hepatic or renal impairment. Antiemetic effects: Because of suppression of cough reflex, aspiration of vomitus possible. CNS effects: May impair mental or physical abilities, especially during first few days of therapy. Hepatic effects: Jaundice usually occurs between second and fourth weeks of treatment; considered hypersensitivity reaction. Usually reversible. Neuroleptic malignant syndrome: Has occurred with agents of this class; is potentially fatal. Signs and symptoms are hyperpyrexia, muscle rigidity, altered mental status, irregular pulse, irregular blood pressure, tachycardia, and diaphoresis. Pulmonary: Cases of bronchopneumonia, some fatal, have occurred. Sudden death: Has been reported; predisposing factors may be seizures or previous brain damage. Flare-ups of psychotic behavior may precede death. Tardive dyskinesia: Syndrome of potentially irreversible involuntary body and facial movements may develop. Prevalence highest in elderly, especially women. Use smallest effective doses for shortest possible time period.
|
PATIENT CARE CONSIDERATIONS |
|

Administration/Storage
- Administer tablets with meals or with full glass of milk or water.
- Protect from light.
Oral Liquid Concentrate
- Dilute just prior to administration in 60 ml of one of following diluents: Water, saline, homogenized milk, carbonated orange beverage, and pineapple, apricot, prune, orange, V-8, tomato, or grapefruit juices.
- Do not mix with caffeinated beverages or with drinks containing tannins (tea) or pectinates (apple juice), because physical incompatibilities may occur.
- Shake concentrate before use.
- Dilute each 5 ml of concentrate with at least 60 ml of fluid.
- Protect from light; store at room temperature.
IV
- Give as diluted solution by fractional injection of slow-drip infusion. Slow infusion method is preferred for surgical patients.
- Dilute solution to 0.5 mg/ml (1 ml mixed with 9 ml of saline solution) and give £ 1 mg per injection at not less than 1 to 2 min intervals. Do not exceed 5 mg.
IM
- Administer injectable form by deep IM to sitting or recumbent patients.

Assessment/Interventions
- Obtain patient history, including drug history and any known allergies.
- Monitor for potential signs of pseudoparkinsonism, dystonia, dyskinesia, or akathisia and report to physician.
- Monitor for evidence of tardive dyskinesia (eg, involuntary dyskinetic movements of tongue, lip, mouth, face, or jaw), and report to physician.
- Be alert for evidence of orthostatic hypotension; take orthostatic BP and report to physician.
- Report any significant unexplained temperature increase to physician.
- When coadministering anticholinergic drugs, be alert for possible decreased therapeutic effects of perphenazine and increased anticholinergic effects.
| OVERDOSAGE: SIGNS & SYMPTOMS |
| |
CNS depression, hypotension, extrapyramidal symptoms, agitation, convulsions, fever, hypothermia, ECG changes, cardiac arrhythmias |
|

Patient/Family Education
- Instruct patient to report the following symptoms to physician: Dizziness, drooling, restlessness, tremors, stiffness, muscle spasms or involuntary face, tongue, mouth, or lip movements.
- Caution patient to avoid sudden position changes to prevent orthostatic hypotension.
- Instruct patient to avoid intake of alcoholic beverages or other CNS depressants.
- Advise patient to use caution driving or performing other tasks requiring mental alertness.
- Caution patient to avoid exposure to sunlight and to use sunscreen or wear protective clothing to avoid photosensitivity reaction.
Indications for Drugs ::
| (per-FEN-uh-zeen) |
Trilafon,  Apo-Perphenazine, Phenazine, PMS-Perphenazine Apo-Perphenazine, Phenazine, PMS-Perphenazine |
| Class: Antipsychotic/Phenothiazine/Antiemetic |

Action Effects apparently caused by postsynaptic dopamine receptor blockade in CNS.

Indications Management of psychotic disorders; control of severe nausea/vomiting; intractable hiccoughs in adults. Unlabeled use(s): Treatment of Tourette’s syndrome; control of acute agitation in elderly; useful in controlling some symptoms of dementia such as agitation, hyperactivity, hallucinations, suspiciousness, hostility and uncooperative behaviors; treatment of hemiballismus (violent writhing/movement of one side of body).

Contraindications Comatose or severely depressed states; allergy to any phenothiazine; presence of large amounts of other CNS depressants; bone marrow depression or blood dyscrasias; liver damage; subcortical brain damage.

Route/Dosage
Psychiatric
ADULT: Nonhospitalized patients: PO 4 to 8 mg tid, reduce as soon as possible to minimum effective dosage.
Hospitalized patients: PO 8 to 16 mg bid to qid; avoid dosages > 64 mg/day.
Nausea/Vomiting/Hiccoughs
ADULTS: PO 8–16 mg/day in divided doses. (Give elderly and debilitated patients lower doses. Administer 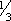 to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
IM
Doses range from 5 to 10 mg/injection, usually given q 6 hr. Do not exceed 30 mg/day. Administer by deep injection to seated or recumbent patient. IM administration usually reserved for instances in which patient is unwilling or unable to take oral medication.
ORAL LIQUID CONCENTRATE AND IV FORM
See Administration/Storage.

Interactions
Alcohol: May result in increased CNS depression and may precipitate extrapyramidal reaction. Anticholinergics: May reduce therapeutic effects of perphenazine and worsen anticholinergic effects. Concomitant administration may worsen schizophrenic symptoms and lead to tardive dyskinesia (see Precautions). Barbiturate anesthetics: Frequency and severity of neuromuscular excitation and hypotension may increase. Guanethidine: Hypotensive action of guanethidine may be inhibited. Metrizamide: Possibility of seizure may be increased when subarachnoid metrizamide injection is used.

Lab Test Interferences May discolor urine pink to red-brown. False-positive pregnancy tests may occur but are less likely to occur with serum test. Increases in protein-bound iodine have been reported.

Adverse Reactions
CV: Orthostatic hypotension; hypertension; tachycardia; bradycardia; syncope; cardiac arrest; circulatory collapse; lightheadedness; faintness; dizziness; ECG changes. CNS: Pseudoparkinsonism dystonia; dyskinesia, motor restlessness; oculogyric crisis; dystonias; hyperreflexia; tardive dyskinesia; drowsiness; headache; fatigue; abnormalities of the cerebrospinal fluid proteins; paradoxical excitement or exacerbation of psychotic symptoms; catatonic-like states; weakness; tremor; paranoid reactions; lethargy; seizures; hyperactivity; nocturnal confusion; bizarre dreams; vertigo; insomnia. DERM: Photosensitivity; skin pigmentation; dry skin; exfoliative dermatitis; urticarial rash; maculopapular hypersensitivity reaction; seborrhea; eczema. EENT: Pigmentary retinopathy; glaucoma; photophobia; blurred vision; mydriasis; increased intraocular pressure; dry mouth or throat; nasal congestion. GI: Dyspepsia; adynamic ileus (may result in death); nausea; vomiting; constipation. GU: Urinary hesitancy or retention; impotence; sexual dysfunction; menstrual irregularities. HEMA: Agranulocytosis; eosinophilia; leukopenia; hemolytic anemia; thrombocytopenic purpura. HEPA: Jaundice. META: Hyperglycemia; hypoglycemia; decreased cholesterol. RESP: Laryngospasm; bronchospasm; dyspnea. OTHER: Increases in appetite and weight; polydipsia; breast enlargement; galactorrhea; increased prolactin levels.

Precautions
Pregnancy: Pregnancy category undetermined. Lactation: Undetermined. Children: Not recommended in children < 12 yr. Elderly: More susceptible to effects; consider lower dose. Special-risk patients: Use caution in patients with cardiovascular disease or mitral insufficiency, history of glaucoma, EEG abnormalities or seizure disorders, prior brain damage, hepatic or renal impairment. Antiemetic effects: Because of suppression of cough reflex, aspiration of vomitus possible. CNS effects: May impair mental or physical abilities, especially during first few days of therapy. Hepatic effects: Jaundice usually occurs between second and fourth weeks of treatment; considered hypersensitivity reaction. Usually reversible. Neuroleptic malignant syndrome: Has occurred with agents of this class; is potentially fatal. Signs and symptoms are hyperpyrexia, muscle rigidity, altered mental status, irregular pulse, irregular blood pressure, tachycardia, and diaphoresis. Pulmonary: Cases of bronchopneumonia, some fatal, have occurred. Sudden death: Has been reported; predisposing factors may be seizures or previous brain damage. Flare-ups of psychotic behavior may precede death. Tardive dyskinesia: Syndrome of potentially irreversible involuntary body and facial movements may develop. Prevalence highest in elderly, especially women. Use smallest effective doses for shortest possible time period.
|
PATIENT CARE CONSIDERATIONS |
|

Administration/Storage
- Administer tablets with meals or with full glass of milk or water.
- Protect from light.
Oral Liquid Concentrate
- Dilute just prior to administration in 60 ml of one of following diluents: Water, saline, homogenized milk, carbonated orange beverage, and pineapple, apricot, prune, orange, V-8, tomato, or grapefruit juices.
- Do not mix with caffeinated beverages or with drinks containing tannins (tea) or pectinates (apple juice), because physical incompatibilities may occur.
- Shake concentrate before use.
- Dilute each 5 ml of concentrate with at least 60 ml of fluid.
- Protect from light; store at room temperature.
IV
- Give as diluted solution by fractional injection of slow-drip infusion. Slow infusion method is preferred for surgical patients.
- Dilute solution to 0.5 mg/ml (1 ml mixed with 9 ml of saline solution) and give £ 1 mg per injection at not less than 1 to 2 min intervals. Do not exceed 5 mg.
IM
- Administer injectable form by deep IM to sitting or recumbent patients.

Assessment/Interventions
- Obtain patient history, including drug history and any known allergies.
- Monitor for potential signs of pseudoparkinsonism, dystonia, dyskinesia, or akathisia and report to physician.
- Monitor for evidence of tardive dyskinesia (eg, involuntary dyskinetic movements of tongue, lip, mouth, face, or jaw), and report to physician.
- Be alert for evidence of orthostatic hypotension; take orthostatic BP and report to physician.
- Report any significant unexplained temperature increase to physician.
- When coadministering anticholinergic drugs, be alert for possible decreased therapeutic effects of perphenazine and increased anticholinergic effects.
| OVERDOSAGE: SIGNS & SYMPTOMS |
| |
CNS depression, hypotension, extrapyramidal symptoms, agitation, convulsions, fever, hypothermia, ECG changes, cardiac arrhythmias |
|

Patient/Family Education
- Instruct patient to report the following symptoms to physician: Dizziness, drooling, restlessness, tremors, stiffness, muscle spasms or involuntary face, tongue, mouth, or lip movements.
- Caution patient to avoid sudden position changes to prevent orthostatic hypotension.
- Instruct patient to avoid intake of alcoholic beverages or other CNS depressants.
- Advise patient to use caution driving or performing other tasks requiring mental alertness.
- Caution patient to avoid exposure to sunlight and to use sunscreen or wear protective clothing to avoid photosensitivity reaction.
Drug Dose ::
| (per-FEN-uh-zeen) |
Trilafon,  Apo-Perphenazine, Phenazine, PMS-Perphenazine Apo-Perphenazine, Phenazine, PMS-Perphenazine |
| Class: Antipsychotic/Phenothiazine/Antiemetic |

Action Effects apparently caused by postsynaptic dopamine receptor blockade in CNS.

Indications Management of psychotic disorders; control of severe nausea/vomiting; intractable hiccoughs in adults. Unlabeled use(s): Treatment of Tourette’s syndrome; control of acute agitation in elderly; useful in controlling some symptoms of dementia such as agitation, hyperactivity, hallucinations, suspiciousness, hostility and uncooperative behaviors; treatment of hemiballismus (violent writhing/movement of one side of body).

Contraindications Comatose or severely depressed states; allergy to any phenothiazine; presence of large amounts of other CNS depressants; bone marrow depression or blood dyscrasias; liver damage; subcortical brain damage.

Route/Dosage
Psychiatric
ADULT: Nonhospitalized patients: PO 4 to 8 mg tid, reduce as soon as possible to minimum effective dosage.
Hospitalized patients: PO 8 to 16 mg bid to qid; avoid dosages > 64 mg/day.
Nausea/Vomiting/Hiccoughs
ADULTS: PO 8–16 mg/day in divided doses. (Give elderly and debilitated patients lower doses. Administer 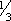 to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
IM
Doses range from 5 to 10 mg/injection, usually given q 6 hr. Do not exceed 30 mg/day. Administer by deep injection to seated or recumbent patient. IM administration usually reserved for instances in which patient is unwilling or unable to take oral medication.
ORAL LIQUID CONCENTRATE AND IV FORM
See Administration/Storage.

Interactions
Alcohol: May result in increased CNS depression and may precipitate extrapyramidal reaction. Anticholinergics: May reduce therapeutic effects of perphenazine and worsen anticholinergic effects. Concomitant administration may worsen schizophrenic symptoms and lead to tardive dyskinesia (see Precautions). Barbiturate anesthetics: Frequency and severity of neuromuscular excitation and hypotension may increase. Guanethidine: Hypotensive action of guanethidine may be inhibited. Metrizamide: Possibility of seizure may be increased when subarachnoid metrizamide injection is used.

Lab Test Interferences May discolor urine pink to red-brown. False-positive pregnancy tests may occur but are less likely to occur with serum test. Increases in protein-bound iodine have been reported.

Adverse Reactions
CV: Orthostatic hypotension; hypertension; tachycardia; bradycardia; syncope; cardiac arrest; circulatory collapse; lightheadedness; faintness; dizziness; ECG changes. CNS: Pseudoparkinsonism dystonia; dyskinesia, motor restlessness; oculogyric crisis; dystonias; hyperreflexia; tardive dyskinesia; drowsiness; headache; fatigue; abnormalities of the cerebrospinal fluid proteins; paradoxical excitement or exacerbation of psychotic symptoms; catatonic-like states; weakness; tremor; paranoid reactions; lethargy; seizures; hyperactivity; nocturnal confusion; bizarre dreams; vertigo; insomnia. DERM: Photosensitivity; skin pigmentation; dry skin; exfoliative dermatitis; urticarial rash; maculopapular hypersensitivity reaction; seborrhea; eczema. EENT: Pigmentary retinopathy; glaucoma; photophobia; blurred vision; mydriasis; increased intraocular pressure; dry mouth or throat; nasal congestion. GI: Dyspepsia; adynamic ileus (may result in death); nausea; vomiting; constipation. GU: Urinary hesitancy or retention; impotence; sexual dysfunction; menstrual irregularities. HEMA: Agranulocytosis; eosinophilia; leukopenia; hemolytic anemia; thrombocytopenic purpura. HEPA: Jaundice. META: Hyperglycemia; hypoglycemia; decreased cholesterol. RESP: Laryngospasm; bronchospasm; dyspnea. OTHER: Increases in appetite and weight; polydipsia; breast enlargement; galactorrhea; increased prolactin levels.

Precautions
Pregnancy: Pregnancy category undetermined. Lactation: Undetermined. Children: Not recommended in children < 12 yr. Elderly: More susceptible to effects; consider lower dose. Special-risk patients: Use caution in patients with cardiovascular disease or mitral insufficiency, history of glaucoma, EEG abnormalities or seizure disorders, prior brain damage, hepatic or renal impairment. Antiemetic effects: Because of suppression of cough reflex, aspiration of vomitus possible. CNS effects: May impair mental or physical abilities, especially during first few days of therapy. Hepatic effects: Jaundice usually occurs between second and fourth weeks of treatment; considered hypersensitivity reaction. Usually reversible. Neuroleptic malignant syndrome: Has occurred with agents of this class; is potentially fatal. Signs and symptoms are hyperpyrexia, muscle rigidity, altered mental status, irregular pulse, irregular blood pressure, tachycardia, and diaphoresis. Pulmonary: Cases of bronchopneumonia, some fatal, have occurred. Sudden death: Has been reported; predisposing factors may be seizures or previous brain damage. Flare-ups of psychotic behavior may precede death. Tardive dyskinesia: Syndrome of potentially irreversible involuntary body and facial movements may develop. Prevalence highest in elderly, especially women. Use smallest effective doses for shortest possible time period.
|
PATIENT CARE CONSIDERATIONS |
|

Administration/Storage
- Administer tablets with meals or with full glass of milk or water.
- Protect from light.
Oral Liquid Concentrate
- Dilute just prior to administration in 60 ml of one of following diluents: Water, saline, homogenized milk, carbonated orange beverage, and pineapple, apricot, prune, orange, V-8, tomato, or grapefruit juices.
- Do not mix with caffeinated beverages or with drinks containing tannins (tea) or pectinates (apple juice), because physical incompatibilities may occur.
- Shake concentrate before use.
- Dilute each 5 ml of concentrate with at least 60 ml of fluid.
- Protect from light; store at room temperature.
IV
- Give as diluted solution by fractional injection of slow-drip infusion. Slow infusion method is preferred for surgical patients.
- Dilute solution to 0.5 mg/ml (1 ml mixed with 9 ml of saline solution) and give £ 1 mg per injection at not less than 1 to 2 min intervals. Do not exceed 5 mg.
IM
- Administer injectable form by deep IM to sitting or recumbent patients.

Assessment/Interventions
- Obtain patient history, including drug history and any known allergies.
- Monitor for potential signs of pseudoparkinsonism, dystonia, dyskinesia, or akathisia and report to physician.
- Monitor for evidence of tardive dyskinesia (eg, involuntary dyskinetic movements of tongue, lip, mouth, face, or jaw), and report to physician.
- Be alert for evidence of orthostatic hypotension; take orthostatic BP and report to physician.
- Report any significant unexplained temperature increase to physician.
- When coadministering anticholinergic drugs, be alert for possible decreased therapeutic effects of perphenazine and increased anticholinergic effects.
| OVERDOSAGE: SIGNS & SYMPTOMS |
| |
CNS depression, hypotension, extrapyramidal symptoms, agitation, convulsions, fever, hypothermia, ECG changes, cardiac arrhythmias |
|

Patient/Family Education
- Instruct patient to report the following symptoms to physician: Dizziness, drooling, restlessness, tremors, stiffness, muscle spasms or involuntary face, tongue, mouth, or lip movements.
- Caution patient to avoid sudden position changes to prevent orthostatic hypotension.
- Instruct patient to avoid intake of alcoholic beverages or other CNS depressants.
- Advise patient to use caution driving or performing other tasks requiring mental alertness.
- Caution patient to avoid exposure to sunlight and to use sunscreen or wear protective clothing to avoid photosensitivity reaction.
Contraindication ::
| (per-FEN-uh-zeen) |
Trilafon,  Apo-Perphenazine, Phenazine, PMS-Perphenazine Apo-Perphenazine, Phenazine, PMS-Perphenazine |
| Class: Antipsychotic/Phenothiazine/Antiemetic |

Action Effects apparently caused by postsynaptic dopamine receptor blockade in CNS.

Indications Management of psychotic disorders; control of severe nausea/vomiting; intractable hiccoughs in adults. Unlabeled use(s): Treatment of Tourette’s syndrome; control of acute agitation in elderly; useful in controlling some symptoms of dementia such as agitation, hyperactivity, hallucinations, suspiciousness, hostility and uncooperative behaviors; treatment of hemiballismus (violent writhing/movement of one side of body).

Contraindications Comatose or severely depressed states; allergy to any phenothiazine; presence of large amounts of other CNS depressants; bone marrow depression or blood dyscrasias; liver damage; subcortical brain damage.

Route/Dosage
Psychiatric
ADULT: Nonhospitalized patients: PO 4 to 8 mg tid, reduce as soon as possible to minimum effective dosage.
Hospitalized patients: PO 8 to 16 mg bid to qid; avoid dosages > 64 mg/day.
Nausea/Vomiting/Hiccoughs
ADULTS: PO 8–16 mg/day in divided doses. (Give elderly and debilitated patients lower doses. Administer 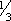 to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
IM
Doses range from 5 to 10 mg/injection, usually given q 6 hr. Do not exceed 30 mg/day. Administer by deep injection to seated or recumbent patient. IM administration usually reserved for instances in which patient is unwilling or unable to take oral medication.
ORAL LIQUID CONCENTRATE AND IV FORM
See Administration/Storage.

Interactions
Alcohol: May result in increased CNS depression and may precipitate extrapyramidal reaction. Anticholinergics: May reduce therapeutic effects of perphenazine and worsen anticholinergic effects. Concomitant administration may worsen schizophrenic symptoms and lead to tardive dyskinesia (see Precautions). Barbiturate anesthetics: Frequency and severity of neuromuscular excitation and hypotension may increase. Guanethidine: Hypotensive action of guanethidine may be inhibited. Metrizamide: Possibility of seizure may be increased when subarachnoid metrizamide injection is used.

Lab Test Interferences May discolor urine pink to red-brown. False-positive pregnancy tests may occur but are less likely to occur with serum test. Increases in protein-bound iodine have been reported.

Adverse Reactions
CV: Orthostatic hypotension; hypertension; tachycardia; bradycardia; syncope; cardiac arrest; circulatory collapse; lightheadedness; faintness; dizziness; ECG changes. CNS: Pseudoparkinsonism dystonia; dyskinesia, motor restlessness; oculogyric crisis; dystonias; hyperreflexia; tardive dyskinesia; drowsiness; headache; fatigue; abnormalities of the cerebrospinal fluid proteins; paradoxical excitement or exacerbation of psychotic symptoms; catatonic-like states; weakness; tremor; paranoid reactions; lethargy; seizures; hyperactivity; nocturnal confusion; bizarre dreams; vertigo; insomnia. DERM: Photosensitivity; skin pigmentation; dry skin; exfoliative dermatitis; urticarial rash; maculopapular hypersensitivity reaction; seborrhea; eczema. EENT: Pigmentary retinopathy; glaucoma; photophobia; blurred vision; mydriasis; increased intraocular pressure; dry mouth or throat; nasal congestion. GI: Dyspepsia; adynamic ileus (may result in death); nausea; vomiting; constipation. GU: Urinary hesitancy or retention; impotence; sexual dysfunction; menstrual irregularities. HEMA: Agranulocytosis; eosinophilia; leukopenia; hemolytic anemia; thrombocytopenic purpura. HEPA: Jaundice. META: Hyperglycemia; hypoglycemia; decreased cholesterol. RESP: Laryngospasm; bronchospasm; dyspnea. OTHER: Increases in appetite and weight; polydipsia; breast enlargement; galactorrhea; increased prolactin levels.

Precautions
Pregnancy: Pregnancy category undetermined. Lactation: Undetermined. Children: Not recommended in children < 12 yr. Elderly: More susceptible to effects; consider lower dose. Special-risk patients: Use caution in patients with cardiovascular disease or mitral insufficiency, history of glaucoma, EEG abnormalities or seizure disorders, prior brain damage, hepatic or renal impairment. Antiemetic effects: Because of suppression of cough reflex, aspiration of vomitus possible. CNS effects: May impair mental or physical abilities, especially during first few days of therapy. Hepatic effects: Jaundice usually occurs between second and fourth weeks of treatment; considered hypersensitivity reaction. Usually reversible. Neuroleptic malignant syndrome: Has occurred with agents of this class; is potentially fatal. Signs and symptoms are hyperpyrexia, muscle rigidity, altered mental status, irregular pulse, irregular blood pressure, tachycardia, and diaphoresis. Pulmonary: Cases of bronchopneumonia, some fatal, have occurred. Sudden death: Has been reported; predisposing factors may be seizures or previous brain damage. Flare-ups of psychotic behavior may precede death. Tardive dyskinesia: Syndrome of potentially irreversible involuntary body and facial movements may develop. Prevalence highest in elderly, especially women. Use smallest effective doses for shortest possible time period.
|
PATIENT CARE CONSIDERATIONS |
|

Administration/Storage
- Administer tablets with meals or with full glass of milk or water.
- Protect from light.
Oral Liquid Concentrate
- Dilute just prior to administration in 60 ml of one of following diluents: Water, saline, homogenized milk, carbonated orange beverage, and pineapple, apricot, prune, orange, V-8, tomato, or grapefruit juices.
- Do not mix with caffeinated beverages or with drinks containing tannins (tea) or pectinates (apple juice), because physical incompatibilities may occur.
- Shake concentrate before use.
- Dilute each 5 ml of concentrate with at least 60 ml of fluid.
- Protect from light; store at room temperature.
IV
- Give as diluted solution by fractional injection of slow-drip infusion. Slow infusion method is preferred for surgical patients.
- Dilute solution to 0.5 mg/ml (1 ml mixed with 9 ml of saline solution) and give £ 1 mg per injection at not less than 1 to 2 min intervals. Do not exceed 5 mg.
IM
- Administer injectable form by deep IM to sitting or recumbent patients.

Assessment/Interventions
- Obtain patient history, including drug history and any known allergies.
- Monitor for potential signs of pseudoparkinsonism, dystonia, dyskinesia, or akathisia and report to physician.
- Monitor for evidence of tardive dyskinesia (eg, involuntary dyskinetic movements of tongue, lip, mouth, face, or jaw), and report to physician.
- Be alert for evidence of orthostatic hypotension; take orthostatic BP and report to physician.
- Report any significant unexplained temperature increase to physician.
- When coadministering anticholinergic drugs, be alert for possible decreased therapeutic effects of perphenazine and increased anticholinergic effects.
| OVERDOSAGE: SIGNS & SYMPTOMS |
| |
CNS depression, hypotension, extrapyramidal symptoms, agitation, convulsions, fever, hypothermia, ECG changes, cardiac arrhythmias |
|

Patient/Family Education
- Instruct patient to report the following symptoms to physician: Dizziness, drooling, restlessness, tremors, stiffness, muscle spasms or involuntary face, tongue, mouth, or lip movements.
- Caution patient to avoid sudden position changes to prevent orthostatic hypotension.
- Instruct patient to avoid intake of alcoholic beverages or other CNS depressants.
- Advise patient to use caution driving or performing other tasks requiring mental alertness.
- Caution patient to avoid exposure to sunlight and to use sunscreen or wear protective clothing to avoid photosensitivity reaction.
Drug Precautions ::
| (per-FEN-uh-zeen) |
Trilafon,  Apo-Perphenazine, Phenazine, PMS-Perphenazine Apo-Perphenazine, Phenazine, PMS-Perphenazine |
| Class: Antipsychotic/Phenothiazine/Antiemetic |

Action Effects apparently caused by postsynaptic dopamine receptor blockade in CNS.

Indications Management of psychotic disorders; control of severe nausea/vomiting; intractable hiccoughs in adults. Unlabeled use(s): Treatment of Tourette’s syndrome; control of acute agitation in elderly; useful in controlling some symptoms of dementia such as agitation, hyperactivity, hallucinations, suspiciousness, hostility and uncooperative behaviors; treatment of hemiballismus (violent writhing/movement of one side of body).

Contraindications Comatose or severely depressed states; allergy to any phenothiazine; presence of large amounts of other CNS depressants; bone marrow depression or blood dyscrasias; liver damage; subcortical brain damage.

Route/Dosage
Psychiatric
ADULT: Nonhospitalized patients: PO 4 to 8 mg tid, reduce as soon as possible to minimum effective dosage.
Hospitalized patients: PO 8 to 16 mg bid to qid; avoid dosages > 64 mg/day.
Nausea/Vomiting/Hiccoughs
ADULTS: PO 8–16 mg/day in divided doses. (Give elderly and debilitated patients lower doses. Administer 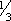 to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
IM
Doses range from 5 to 10 mg/injection, usually given q 6 hr. Do not exceed 30 mg/day. Administer by deep injection to seated or recumbent patient. IM administration usually reserved for instances in which patient is unwilling or unable to take oral medication.
ORAL LIQUID CONCENTRATE AND IV FORM
See Administration/Storage.

Interactions
Alcohol: May result in increased CNS depression and may precipitate extrapyramidal reaction. Anticholinergics: May reduce therapeutic effects of perphenazine and worsen anticholinergic effects. Concomitant administration may worsen schizophrenic symptoms and lead to tardive dyskinesia (see Precautions). Barbiturate anesthetics: Frequency and severity of neuromuscular excitation and hypotension may increase. Guanethidine: Hypotensive action of guanethidine may be inhibited. Metrizamide: Possibility of seizure may be increased when subarachnoid metrizamide injection is used.

Lab Test Interferences May discolor urine pink to red-brown. False-positive pregnancy tests may occur but are less likely to occur with serum test. Increases in protein-bound iodine have been reported.

Adverse Reactions
CV: Orthostatic hypotension; hypertension; tachycardia; bradycardia; syncope; cardiac arrest; circulatory collapse; lightheadedness; faintness; dizziness; ECG changes. CNS: Pseudoparkinsonism dystonia; dyskinesia, motor restlessness; oculogyric crisis; dystonias; hyperreflexia; tardive dyskinesia; drowsiness; headache; fatigue; abnormalities of the cerebrospinal fluid proteins; paradoxical excitement or exacerbation of psychotic symptoms; catatonic-like states; weakness; tremor; paranoid reactions; lethargy; seizures; hyperactivity; nocturnal confusion; bizarre dreams; vertigo; insomnia. DERM: Photosensitivity; skin pigmentation; dry skin; exfoliative dermatitis; urticarial rash; maculopapular hypersensitivity reaction; seborrhea; eczema. EENT: Pigmentary retinopathy; glaucoma; photophobia; blurred vision; mydriasis; increased intraocular pressure; dry mouth or throat; nasal congestion. GI: Dyspepsia; adynamic ileus (may result in death); nausea; vomiting; constipation. GU: Urinary hesitancy or retention; impotence; sexual dysfunction; menstrual irregularities. HEMA: Agranulocytosis; eosinophilia; leukopenia; hemolytic anemia; thrombocytopenic purpura. HEPA: Jaundice. META: Hyperglycemia; hypoglycemia; decreased cholesterol. RESP: Laryngospasm; bronchospasm; dyspnea. OTHER: Increases in appetite and weight; polydipsia; breast enlargement; galactorrhea; increased prolactin levels.

Precautions
Pregnancy: Pregnancy category undetermined. Lactation: Undetermined. Children: Not recommended in children < 12 yr. Elderly: More susceptible to effects; consider lower dose. Special-risk patients: Use caution in patients with cardiovascular disease or mitral insufficiency, history of glaucoma, EEG abnormalities or seizure disorders, prior brain damage, hepatic or renal impairment. Antiemetic effects: Because of suppression of cough reflex, aspiration of vomitus possible. CNS effects: May impair mental or physical abilities, especially during first few days of therapy. Hepatic effects: Jaundice usually occurs between second and fourth weeks of treatment; considered hypersensitivity reaction. Usually reversible. Neuroleptic malignant syndrome: Has occurred with agents of this class; is potentially fatal. Signs and symptoms are hyperpyrexia, muscle rigidity, altered mental status, irregular pulse, irregular blood pressure, tachycardia, and diaphoresis. Pulmonary: Cases of bronchopneumonia, some fatal, have occurred. Sudden death: Has been reported; predisposing factors may be seizures or previous brain damage. Flare-ups of psychotic behavior may precede death. Tardive dyskinesia: Syndrome of potentially irreversible involuntary body and facial movements may develop. Prevalence highest in elderly, especially women. Use smallest effective doses for shortest possible time period.
|
PATIENT CARE CONSIDERATIONS |
|

Administration/Storage
- Administer tablets with meals or with full glass of milk or water.
- Protect from light.
Oral Liquid Concentrate
- Dilute just prior to administration in 60 ml of one of following diluents: Water, saline, homogenized milk, carbonated orange beverage, and pineapple, apricot, prune, orange, V-8, tomato, or grapefruit juices.
- Do not mix with caffeinated beverages or with drinks containing tannins (tea) or pectinates (apple juice), because physical incompatibilities may occur.
- Shake concentrate before use.
- Dilute each 5 ml of concentrate with at least 60 ml of fluid.
- Protect from light; store at room temperature.
IV
- Give as diluted solution by fractional injection of slow-drip infusion. Slow infusion method is preferred for surgical patients.
- Dilute solution to 0.5 mg/ml (1 ml mixed with 9 ml of saline solution) and give £ 1 mg per injection at not less than 1 to 2 min intervals. Do not exceed 5 mg.
IM
- Administer injectable form by deep IM to sitting or recumbent patients.

Assessment/Interventions
- Obtain patient history, including drug history and any known allergies.
- Monitor for potential signs of pseudoparkinsonism, dystonia, dyskinesia, or akathisia and report to physician.
- Monitor for evidence of tardive dyskinesia (eg, involuntary dyskinetic movements of tongue, lip, mouth, face, or jaw), and report to physician.
- Be alert for evidence of orthostatic hypotension; take orthostatic BP and report to physician.
- Report any significant unexplained temperature increase to physician.
- When coadministering anticholinergic drugs, be alert for possible decreased therapeutic effects of perphenazine and increased anticholinergic effects.
| OVERDOSAGE: SIGNS & SYMPTOMS |
| |
CNS depression, hypotension, extrapyramidal symptoms, agitation, convulsions, fever, hypothermia, ECG changes, cardiac arrhythmias |
|

Patient/Family Education
- Instruct patient to report the following symptoms to physician: Dizziness, drooling, restlessness, tremors, stiffness, muscle spasms or involuntary face, tongue, mouth, or lip movements.
- Caution patient to avoid sudden position changes to prevent orthostatic hypotension.
- Instruct patient to avoid intake of alcoholic beverages or other CNS depressants.
- Advise patient to use caution driving or performing other tasks requiring mental alertness.
- Caution patient to avoid exposure to sunlight and to use sunscreen or wear protective clothing to avoid photosensitivity reaction.
Drug Side Effects ::
| (per-FEN-uh-zeen) |
Trilafon,  Apo-Perphenazine, Phenazine, PMS-Perphenazine Apo-Perphenazine, Phenazine, PMS-Perphenazine |
| Class: Antipsychotic/Phenothiazine/Antiemetic |

Action Effects apparently caused by postsynaptic dopamine receptor blockade in CNS.

Indications Management of psychotic disorders; control of severe nausea/vomiting; intractable hiccoughs in adults. Unlabeled use(s): Treatment of Tourette’s syndrome; control of acute agitation in elderly; useful in controlling some symptoms of dementia such as agitation, hyperactivity, hallucinations, suspiciousness, hostility and uncooperative behaviors; treatment of hemiballismus (violent writhing/movement of one side of body).

Contraindications Comatose or severely depressed states; allergy to any phenothiazine; presence of large amounts of other CNS depressants; bone marrow depression or blood dyscrasias; liver damage; subcortical brain damage.

Route/Dosage
Psychiatric
ADULT: Nonhospitalized patients: PO 4 to 8 mg tid, reduce as soon as possible to minimum effective dosage.
Hospitalized patients: PO 8 to 16 mg bid to qid; avoid dosages > 64 mg/day.
Nausea/Vomiting/Hiccoughs
ADULTS: PO 8–16 mg/day in divided doses. (Give elderly and debilitated patients lower doses. Administer 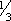 to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
IM
Doses range from 5 to 10 mg/injection, usually given q 6 hr. Do not exceed 30 mg/day. Administer by deep injection to seated or recumbent patient. IM administration usually reserved for instances in which patient is unwilling or unable to take oral medication.
ORAL LIQUID CONCENTRATE AND IV FORM
See Administration/Storage.

Interactions
Alcohol: May result in increased CNS depression and may precipitate extrapyramidal reaction. Anticholinergics: May reduce therapeutic effects of perphenazine and worsen anticholinergic effects. Concomitant administration may worsen schizophrenic symptoms and lead to tardive dyskinesia (see Precautions). Barbiturate anesthetics: Frequency and severity of neuromuscular excitation and hypotension may increase. Guanethidine: Hypotensive action of guanethidine may be inhibited. Metrizamide: Possibility of seizure may be increased when subarachnoid metrizamide injection is used.

Lab Test Interferences May discolor urine pink to red-brown. False-positive pregnancy tests may occur but are less likely to occur with serum test. Increases in protein-bound iodine have been reported.

Adverse Reactions
CV: Orthostatic hypotension; hypertension; tachycardia; bradycardia; syncope; cardiac arrest; circulatory collapse; lightheadedness; faintness; dizziness; ECG changes. CNS: Pseudoparkinsonism dystonia; dyskinesia, motor restlessness; oculogyric crisis; dystonias; hyperreflexia; tardive dyskinesia; drowsiness; headache; fatigue; abnormalities of the cerebrospinal fluid proteins; paradoxical excitement or exacerbation of psychotic symptoms; catatonic-like states; weakness; tremor; paranoid reactions; lethargy; seizures; hyperactivity; nocturnal confusion; bizarre dreams; vertigo; insomnia. DERM: Photosensitivity; skin pigmentation; dry skin; exfoliative dermatitis; urticarial rash; maculopapular hypersensitivity reaction; seborrhea; eczema. EENT: Pigmentary retinopathy; glaucoma; photophobia; blurred vision; mydriasis; increased intraocular pressure; dry mouth or throat; nasal congestion. GI: Dyspepsia; adynamic ileus (may result in death); nausea; vomiting; constipation. GU: Urinary hesitancy or retention; impotence; sexual dysfunction; menstrual irregularities. HEMA: Agranulocytosis; eosinophilia; leukopenia; hemolytic anemia; thrombocytopenic purpura. HEPA: Jaundice. META: Hyperglycemia; hypoglycemia; decreased cholesterol. RESP: Laryngospasm; bronchospasm; dyspnea. OTHER: Increases in appetite and weight; polydipsia; breast enlargement; galactorrhea; increased prolactin levels.

Precautions
Pregnancy: Pregnancy category undetermined. Lactation: Undetermined. Children: Not recommended in children < 12 yr. Elderly: More susceptible to effects; consider lower dose. Special-risk patients: Use caution in patients with cardiovascular disease or mitral insufficiency, history of glaucoma, EEG abnormalities or seizure disorders, prior brain damage, hepatic or renal impairment. Antiemetic effects: Because of suppression of cough reflex, aspiration of vomitus possible. CNS effects: May impair mental or physical abilities, especially during first few days of therapy. Hepatic effects: Jaundice usually occurs between second and fourth weeks of treatment; considered hypersensitivity reaction. Usually reversible. Neuroleptic malignant syndrome: Has occurred with agents of this class; is potentially fatal. Signs and symptoms are hyperpyrexia, muscle rigidity, altered mental status, irregular pulse, irregular blood pressure, tachycardia, and diaphoresis. Pulmonary: Cases of bronchopneumonia, some fatal, have occurred. Sudden death: Has been reported; predisposing factors may be seizures or previous brain damage. Flare-ups of psychotic behavior may precede death. Tardive dyskinesia: Syndrome of potentially irreversible involuntary body and facial movements may develop. Prevalence highest in elderly, especially women. Use smallest effective doses for shortest possible time period.
|
PATIENT CARE CONSIDERATIONS |
|

Administration/Storage
- Administer tablets with meals or with full glass of milk or water.
- Protect from light.
Oral Liquid Concentrate
- Dilute just prior to administration in 60 ml of one of following diluents: Water, saline, homogenized milk, carbonated orange beverage, and pineapple, apricot, prune, orange, V-8, tomato, or grapefruit juices.
- Do not mix with caffeinated beverages or with drinks containing tannins (tea) or pectinates (apple juice), because physical incompatibilities may occur.
- Shake concentrate before use.
- Dilute each 5 ml of concentrate with at least 60 ml of fluid.
- Protect from light; store at room temperature.
IV
- Give as diluted solution by fractional injection of slow-drip infusion. Slow infusion method is preferred for surgical patients.
- Dilute solution to 0.5 mg/ml (1 ml mixed with 9 ml of saline solution) and give £ 1 mg per injection at not less than 1 to 2 min intervals. Do not exceed 5 mg.
IM
- Administer injectable form by deep IM to sitting or recumbent patients.

Assessment/Interventions
- Obtain patient history, including drug history and any known allergies.
- Monitor for potential signs of pseudoparkinsonism, dystonia, dyskinesia, or akathisia and report to physician.
- Monitor for evidence of tardive dyskinesia (eg, involuntary dyskinetic movements of tongue, lip, mouth, face, or jaw), and report to physician.
- Be alert for evidence of orthostatic hypotension; take orthostatic BP and report to physician.
- Report any significant unexplained temperature increase to physician.
- When coadministering anticholinergic drugs, be alert for possible decreased therapeutic effects of perphenazine and increased anticholinergic effects.
| OVERDOSAGE: SIGNS & SYMPTOMS |
| |
CNS depression, hypotension, extrapyramidal symptoms, agitation, convulsions, fever, hypothermia, ECG changes, cardiac arrhythmias |
|

Patient/Family Education
- Instruct patient to report the following symptoms to physician: Dizziness, drooling, restlessness, tremors, stiffness, muscle spasms or involuntary face, tongue, mouth, or lip movements.
- Caution patient to avoid sudden position changes to prevent orthostatic hypotension.
- Instruct patient to avoid intake of alcoholic beverages or other CNS depressants.
- Advise patient to use caution driving or performing other tasks requiring mental alertness.
- Caution patient to avoid exposure to sunlight and to use sunscreen or wear protective clothing to avoid photosensitivity reaction.
Drug Mode of Action ::
| (per-FEN-uh-zeen) |
Trilafon,  Apo-Perphenazine, Phenazine, PMS-Perphenazine Apo-Perphenazine, Phenazine, PMS-Perphenazine |
| Class: Antipsychotic/Phenothiazine/Antiemetic |

Action Effects apparently caused by postsynaptic dopamine receptor blockade in CNS.

Indications Management of psychotic disorders; control of severe nausea/vomiting; intractable hiccoughs in adults. Unlabeled use(s): Treatment of Tourette’s syndrome; control of acute agitation in elderly; useful in controlling some symptoms of dementia such as agitation, hyperactivity, hallucinations, suspiciousness, hostility and uncooperative behaviors; treatment of hemiballismus (violent writhing/movement of one side of body).
 Apo-Perphenazine, Phenazine, PMS-Perphenazine
Apo-Perphenazine, Phenazine, PMS-Perphenazine



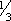 to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.






 Apo-Perphenazine, Phenazine, PMS-Perphenazine
Apo-Perphenazine, Phenazine, PMS-Perphenazine



 to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.
to ½ adult dose.) CHILDREN > 12 YR May be given lowest limit of adult dosage.






 Apo-Perphenazine, Phenazine, PMS-Perphenazine
Apo-Perphenazine, Phenazine, PMS-Perphenazine

