Article Contents ::
- 1 ABDOMINAL PARACENTESIS / ASCITIC TAP /aspiration of peritoneal fluid–
- 2 paracentesis
- 3 Indications for paracentesis-–
- 4 Method of paracentesis —
- 5 THORACOCENTESIS AND PLEURAL BIOPSY Indications–
- 6 THORACOCENTESIS
- 7 Causes of Pleural effusion Exudate/ Transudate :
- 8 Thoracic duct obstruction —
- 9 TUBE THORACOTOMY AND INTERCOSTAL DRAINAGE —
- 10 Endotracheal tube
- 11 OROPHARYNGEAL AIRWAY —
ABDOMINAL PARACENTESIS / ASCITIC TAP /aspiration of peritoneal fluid–
Indications for paracentesis-–
- · Ascites
- · Cirrhosis
- · CHF
- · Abdominal tuberculosis
- · Abdominal malignancy
- · Pancreatitis.
Method of paracentesis —
- · The site of puncture is a point midway between the umbilicus and iliac spine or between the pubis and umbilicus. The patient lies supine after urinating.
- · Patient is sedated, part is prepared, local anaesthetic is infiltrated at the site.
- · A large bore needle is inserted into the abdomen in zig-zag fashion. Fluid comes out and the tube is attached to collecting system. About 1 2 litres offluid is slowly removed.
- For diagnostic purposes only 5 – 10 ml offluid is removed. After the procedure, needle is removed and tincture benzoin seal is applied at the site.
Complication —
- · Syncope, shock – If a large amount of fluid is removed rapidly.
- · Peritonitis
- · Hepatorenal syndrome in hepatic failure.
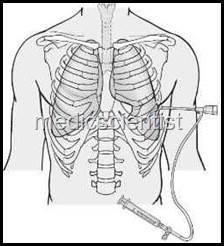
THORACOCENTESIS AND PLEURAL BIOPSY Indications–
- • To confirm the aetiology of pleural effusion.
- · To relieve cardio-respiratory embarrassment due to a massive pleural effusion.
- · In cases of purulent effusion the tap is done to prevent pleural thickening during healing.
Causes of Pleural effusion Exudate/ Transudate :
- 1. Congestive heart failure
- 2. Cirrhosis of liver
- 3.Severe hypoproteinemia ~ Exudate:
- 4. Infection
- i. Synpneumonic effusion ii. Tubercular
- iii. Viral
- iv. Mycoplasmal
- v. Empyema thoracis
- 2. Neoplasm
- i. Bronchogenic carcinoma
- ii. Metastatic carcinoma
- iii. Mesothelioma
- iv. Lymphoma
- 3. Trauma
- 4. Pulmonary infarction
- 5. Connective tissue disorders
- V Chylous
Thoracic duct obstruction —
- 1. Trauma
- 2. Carcinoma
Method —
- · Site of tap is 7th – 9th intercostal space along the scapular or posterior aXilllary line on the affected side.
- · Needle is always introduced at the upper edge of a rib to avoid damage to intercostal vessels.
- · The tap should be done one space below the upper limit of dullness.
- · The patient is made to sit on stool, lean forwards with his hands resting on a table (aspiration table) in front of him.
- · The part is cleaned and draped. Local anaesthetic is injected into the skin, and up to the parietal pleura. A wide bore aspiration needle is connected to a 3 way cannula and a syringe is inserted into the pleural cavity. Fluid is aspirated till possible.
- · Failure of tap may be due to blocked needle, very little fluid, thick fluid, orencysted fluid.
Complications —
- 1. Vasovagal syncope
- 2. Infection
- 3. Pneumothorax
- 4. Haemopneumothorax
- 5. A rapid removal of fluid may cause a rapid fall in intrathoracic pressure leading to acute pulmonary oedema because of the pooling of blood in lungs.
TUBE THORACOTOMY AND INTERCOSTAL DRAINAGE —
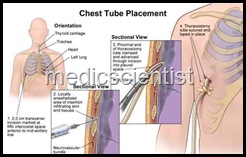 |
| TUBE THORACOTOMY |
Indications
- · Pneumothorax
- · Hemothorax
- · Empyema thoracis
- · Malignant effusions.
Method —
- · Small incision is given a long the upper border of rib.
- A trocar with stilette is introduced, stilette is removed and chest tube is inserted with other end clamped to prevent air entering.
- · This is connected to a sealed bottle with water level.
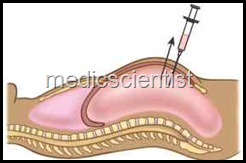
PE ICARDIOCENTESIS Indications
- · Diagnostic and therapeutic in cases of pericardial effusion.
- It is preferably done in a cath lab.
Method —
- · The patient lies supine with head and chest at 60° angle. ECG monitoring is done.
- The needle is inserted into the sub-xiphoid area (preferably under digital imaging-echocardiography), with the tip directed towards the left shoulder at an angle of about 45°.
- A syringe attached to the needle is intermittently sucked to see if fluid comes out.
- When VPCs appear on the ECG the needle is withdrawn so that it lies in the pericardial space. Pericardial fluid is then aspirated.
Complications
- 1. Infection
- 2. Acute traumatic haemopericardium
- 3. Ventricular puncture
- 4. Ventricular arrhythmias
- 5. Pulmonary oedema, due to acute MI, as a result of injury to coronary vessels
- 6. Sudden death.
 |
| Endotracheal tube |
Endotracheal tube
- is used for airway and to administer anaesthesia where face mask cannot be used.
- Positive pressure ventilation can be given with endotracheal tubes as they make an airtight system with the respiratory system.
- Cuffed endotracheal tubes are used for orotracheal intubation.
- Laryngoscope blade is inserted into the mouth to visualize the larynx.
- Endotracheal tube is inserted through the glottis into the larynx and trachea.
 |
| Endoscop |
- This is an instrument for direct view of larynx for intubation for anaesthesia and ventilation.
- It consists of a handle with battery and blade attached to it.
- There is a small electric bulb half way along the blade which is lit by moving the blade to 900 to the handle, in the position in which it can be put in.
- The ambubag is a double-walled structure of rubber which remains in the inflated state. When the bag is squeezed the valve closes the expiratory channel and allows the air to enter into the trachea in inspiration.
- When the bag is released, expiration occurs.
- The air in the bag can be enriched with oxygen through a tube.
- The face mask attached to the ambubag is transparent so that any vomitus or regurgitation can be seen.
 |
| ambubag |
OROPHARYNGEAL AIRWAY —
- This is made of plastic or rubber to prevent biting or obstruction of the endotracheal tube. It also prevents blockage of the air passage by the tongue. It also helps suction from the pharynx.
- This is short discription about these equipments and their uses, I hope you will like this post.
- For future posts and valuable article, subscribe by email, and get latest updates from medicscientist.