Article Contents ::
HYPERGLYCEMIC HYPEROSMOLAR STATE (HHS)
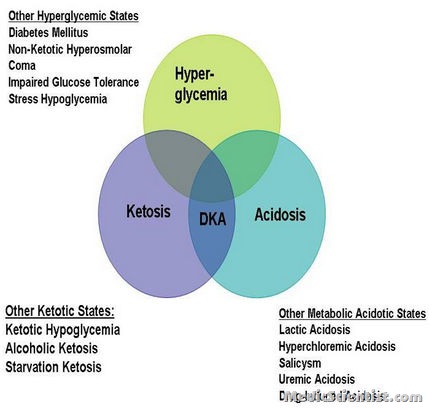
hyperosmolar hyperglycemic state (HHS, also known as nonketotic hyperglycemia) and Diabetic ketoacidosis (DKA) are of the most serious acute complications of diabetes. hyperosmolar hyperglycemic state (HHS, also called nonketotic hyperglycemia) In HHS, there is little or no ketoacid accumulation, the serum glucose concentration frequently exceeds 1000 mg/dL (56 mmol/L), the plasma osmolality may reach 380 mosmol/kg, and neurologic abnormalities are frequently present (including coma in 25 to 50 percent of cases)
Diagnostic criteria for diabetic ketoacidosis (DKA) and hyperosmolar hyperglycemic state (HHS)
| DKA | HHS | |||
| Mild DKA | Moderate DKA | Severe DKA | ||
| Plasma glucose (mg/dL) | >250 | >250 | >250 | >600 |
| Arterial pH | 7.25-7.30 | 7.00-7.24 | <7.00 | >7.30 |
| Serum bicarbonate (mEq/L) | 15-18 | 10 to <15 | <10 | >18 |
| Urine ketones* | Positive | Positive | Positive | Small |
| Serum ketones* | Positive | Positive | Positive | Small |
| Effective serum osmolality (mOsm/kg) | Variable | Variable | Variable | >320 |
| Anion gap | >10 | >12 | >12 | Variable |
| Alteration in sensoria or mental obtundation | Alert | Alert/drowsy | Stupor/coma | Stupor/coma |
Predisposing factors
- · More common in elderly persons
- · In patients with Type 2 diabetes mellitus
- · With polyu ria
- · Weight loss
- · Decreased oral intake
- · Presenting with mental confusion lethargy and coma
- · Severe dehydration
- · Hypotension
- · Tachycardia
- · Altered mental status
- · MI
- · Stroke
- · Sepsis and infections
- · Pneumonia
- · Decreased water intake.

Pathophysiology of HHS
- Cause of HHS:
- • Relative insulin deficiency
- • Inadequate fluid intake Hyperglycemia inauces osmotic diuresis ~Intravascular volume depletion ~Insulin deficiency is less severe than in diabetic keto-acidosis. Lower levels of counter regulatory hormones and free fatty acid in HHS than diabetic ketoacidosis.
Lab diagnosis of HHS Marked hyperglycemia is seen
- (Plasma glucose may be > 100 mg/dl) Hyperosmolality >350 mosmol/L
- Prerenal azotemia
- Serum Na+ – normal or slightly low
- Corrected serum Na+ – is serum sodium +1.6 meq per 100 mg/dl rise in serum glucose
- Acidosis and ketonebodies are absent usually Metabolic acidosis due to lactic acidosis and starvation may be present with small anion gap.
Treatment of HYPERGLYCEMIC HYPEROSMOLAR STATE (HHS)
- Volume depletion and hyperglycemia to be treated as in diabetic ketoacidosis
- Give:
- – IV fluids
- – Insulin infusion
- – Treat precipitating causes of diabetes
- – In HHS dehydration is more than in diabetic ketoacodosis.
- Patients of HHS is usually of older age.
- Mental changes and coma are common. Mortality more in diabetic ketoacidosis.
- 1-3 litre of 0.9% normal saline in 2~3 hours.
- If serum Na is > 150 meq/I then use 0.45% saline. If patient is hemodynamically stable use 0.45% saline of 5% Dextrose solution in water (DSW).
- 10 litre is given in about 2 days.
- Serum potassium is brought to normal by giving potassium. There may be hypomagnesemia or hypophosphotemia. Give KP04 and nutrition.
- Give insulin bolus 5-10 units followed by IV insulin infusion at rate 3 to 7 minutes.
- When blood glucose falls to 250 mg/dl then add glucose to fluid.
- When blood glucose falls to 250 mg/dl infusion rate of insulin decreased to 1-2 unit/hour.
- Insulin infusion to continue till patient takes orally. Then change to subcutaneous insulin. Later switch to oral hypoglycemics if required.
DKA or HHS resolution Facts —
- The hyperglycemic crisis is considered to be resolved after these condition
- The ketoacidosis has resolved, as evidenced by normalization of the serum anion gap (less than 12 meq/L).
- As mentioned above, ketonemia and ketonuria may persist for more than 36 hours due to the slower removal of acetone, in part via the lungs [14,15] .
- Since acetone is biochemically neutral, such patients do not have persistent ketoacidosis.
- Patients with HHS are mentally alert and the plasma effective osmolality is below 315 mosmol/kg.
- The patient is able to eat.