Article Contents ::
- 1 Amyloidosis
- 2 Amyloidosis Classification
- 3 Amyloidosis may be :
- 4 Nomenclature of Amyloidosis
- 5 Systemic Amyloidosis
- 6 Precipitating diseases
- 7 Localized amyloidosis
- 8 Senile systemic amyloidosis
- 9 Renal involvement
- 10 Heart
- 11 Liver
- 12 Spleen
- 13 Skin
- 14 Gastrointestinal tract
- 15 Nervous system
- 16 Endocrine
- 17 Joints and muscles
- 18 Respiratory system
- 19 Hematopoietic system
- 20 Amyloidosis Risk Factors
- 21 Amyloidosis DIAGNOSIS
- 22 Amyloidosis PROGNOSIS
- 23 Amyloidosis TREATMENT
- 24 First Line TREATMENT of Amyloidosis
- 25 Second Line TREATMENT of Amyloidosis
Amyloidosis
Amyloidosis is deposition of insoluble amyloid fibrils in extracellular spaces of organ and tissues due to abnormal protein folding. metabolic disorders resulting from the insidious deposition of protein-containing fibrils (amyloid) in tissues, diseases characterized by extracellular deposition of insoluble protein fibrils in organs and tissues clinical manifestations of amyloidosis are enormously varied, and the disease may mimic many other conditions ranging from nephrotic syndrome (when kidneys are infiltrated) or congestive heart failure (myocardial deposition),to dementias (brain involvement) .
Amyloidosis Classification
- is based on the nature of precursor plasma proteins that form fibril deposits :
- ›Dialysis-related: Deposition of fibrils derived from-microglobulin; predilection for osteoarticular structures
- ›Heritable or familial (AF): Many different types of variant plasma proteins form amyloid deposits beginning in midlife; most common form is caused by mutations of transthyretin (ATTR)
- ›Organ-specific amyloidosis: Deposition isolated to 1 organ, resulting in specific syndromes; most common is Alzheimer disease caused by cerebral amyloid plaques:
- ›Primary (AL): Plasma cell dyscrasia; deposition of protein derived from immunoglobulin light chain fragments
- ›Secondary or reactive (AA): Complicates chronic infections or inflammatory diseases; deposition of serum amyloid A(SAA) protein
- ›Senile systemic amyloidosis: Deposition of otherwise normal (wild-type) transthyretin in myocardium and other sites seen in elderly
- Localized amyloidosis: Results from local amyloid deposits in tracheobronchial tree, urinary tract, or skin, which are also derived from monoclonal light chains, but not due to underling systemic plasma cell disorder
Amyloidosis may be :
- · Systemic amyloidosis
- ·Localized or organ limited amyloidosis. Systemic amyloidosis may be :
- · Neoplastic
- · Inflammatory
- · Genetic
- · Iatrogenic.
- Localized amyloidosis may be associated with aging, diabetes.
- There is no systemic involvement. ,
Nomenclature of Amyloidosis
- The first letter is A for amyloid deposits and then a letter for protein designation like.
- AL – amyloidosis involving immunoglobulin light chains.
Systemic Amyloidosis
- AL or Primary Idiopathic Amyloidosis
- Most common form of Systemic Amyloidosis is AL.
- It is associated with multiple myeloma in some cases.
- AA Amyloidosis
- Secondary, reactive or acquired.
- Occurs as a complication of chronic inflammatory disease.
Precipitating diseases
- · Tuberculosis
- · Osteomyelitis
- · Leprosy.
- Familial causes of AA amylo‘dosis
- Familial Mediterranean fever (FMF), Familial cold urticaria (FCU).
- Colchicine blocks FMF and AA amyloidosis. Heredofamilial amyloidosis:
- Less common, presents as: – Neuropathy – Nephropathy
- – Cardiomyopathy
- – Hepatomegaly
- – Dementia.
Localized amyloidosis
- 1. Polypeptide hormone-derived amyloidosis – Calcitonin, prolactin, insulin can lead to amyloidosis.
- 2. Localized corneal amyloidosis.
- 3. Localized cardiovascular amyloidosis – from atherometous plaques, aortic media, atrial natriuretic factor AANF.
- 4. Associated with Alzheimer’s disease – Beta amyloid protein is found in Alzheimer’s disease and Down’s syndrome.
- 5. Prion diseases – Prions are a class of infectious protein responsible for a group of neurodegenerative disease causing encephalopathy. Ex- Kuru, Creutzfeld-Jakob disease, and fatal insomnia.
Senile systemic amyloidosis
- It is cardiac amyloidosis with systemic involvement.
- Proteinuria
- Peripheral neuropathies Dementia
- Cognitive dysfunction Hepatomegaly
- Kidney enlargement Splenomegaly Cardiomegaly.
Renal involvement
- · Mild proteinuria
- · Frank nephrosis
- · Microscopic hematuria
- · Progressive azotemia
- · Rarely hypertension
- · Death.
Heart
- · Heart failure
- · Low voltage ECG
- · Conduction defects
- · AR, MR
- · Pericarditis with effusion
- · Restrictive CM P.
Liver
- · Portal hypertension
- · Hepatomegaly.
Spleen
- • Spler:lOmegaly.
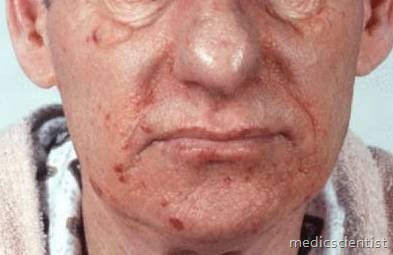
Skin
- · Non pruritic lesions
- · Raised papules or plaque in axilla or inguinal regions
- · Racoon syndrome – periorbital ecchymoses (resembling the face of a racoon).
Gastrointestinal tract
- · Obstruction, ulceration, malabsorption, GI
- haemorrhage
- · Thick tongue – macroglossia.
Nervous system
- · Peripheral neuropathy
- · Postural hypotension
- · Adie’s pupil (a tonic pupil along with weak or absent tendon reflexes in the lower extremities, a benign disorder seen in healthy, young women due to dysautonomia
- · Urinary incontinence.
- Other causes of Adie’s pupil are Shy-Drager syndrome, segmental hypohidrosis, diabetes, amyloidosis.
Endocrine
- · Thyroid enlargement
- · Amyloid infiltration of adrenal gland, pituitary gland and pancreas.
Joints and muscles
- · Symmetric arthritis of small joints
- · Muscle hypertrophy – shoulder pad sign
- · Carpal tunnel syndrome.
Respiratory system
- · Amyloidosis of lungs, bronchi, larynx, trachea
- · May resemble a neoplasm
- · May need excision.
Hematopoietic system
- • Deficiency of clotting factors.
Amyloidosis Risk Factors
- •Depends on type of systemic amyloidosis:
- Untreated chronic inflammatory diseases (AA)
- Untreated chronic infections (AA)
- Underlying plasma cell dyscrasia (AL)
- Long-term hemodialysis
- Heredity (AF/AA)
- Age (senile systemic/Alzheimer)
Amyloidosis DIAGNOSIS
- · Biopsy of abdominal fat, renal or rectal biopsy
- · Congo-red staining shows green birefringence with polarizing microscope.
Amyloidosis PROGNOSIS
- • Death can occur if untreated.
Amyloidosis TREATMENT
- Genetic counseling Hemodialysis
- Kidney transplant
- Liver transplantation Stem cell transplantation Melphalan Iododoxorubicin
- Colchicine – prevents acute attacks.
First Line TREATMENT of Amyloidosis
- •Primary AL
- •Secondary AA:
- Control of underlying inflammatory disease: Consider anticytokine therapy for autoimmune diseases
- Colchicine: for familial Mediterranean fever
Second Line TREATMENT of Amyloidosis
- •Primary AL
- Precautions: Neutropenia, thrombocytopenia, rash, fatigue
- Lenalidomide with dexamethasone
- Bortezomib with dexamethasone
