Article Contents ::
- 1 Pleural Effusion pleural fluid Causes Symptoms Diagnosis Treatment
- 2 Physical Exam for Pleural Effusion
- 3 Etiology of Pleural Effusion
- 4 Transudative effusion
- 5 Exudative pleural effusion
- 6 Pleural Effusion Pathophysiology
- 7 Two-test rule of Pleural Effusion
- 8 The pleural fluid is examined for:
- 9 Causes of pleural effusion Transudative
- 10 Causes of pleural effusion Exudative
- 11 Effusion due to heart failure
- 12 Hepatic causes
- 13 Para pneumonic effusion
- 14 Tubercular pleuritis
- 15 Treatment of Pleural Effusion
- 16 First Line Pleural Effusion treatment
- 17 Second Line Pleural Effusion treatment
Pleural Effusion pleural fluid Causes Symptoms Diagnosis Treatment
- The pleural space lies between the lung and the chest wall between the 2 layers of pleura, the visceral and parietal pleura.
- Normally there is a thin layer of fluid in the pleural space.
- Pleural effusion is said to be present when there- is excessive quantity of fluid in the pleural space.
- Pleural fluid accumulates when the pleural fluid formation exceeds the absorption.
- Pleural fluid may be transudate or exudate.
- Determining the cause of a pleural effusion is greatly facilitated by analysis of the pleural fluid.
- Fluid in the thoracic cavity between the visceral and parietal pleura. It may be seen on a chest radiograph if it exceeds 300 ml.
Physical Exam for Pleural Effusion
- When pleural effusion >300 mL:
- No voice transmission
- Mediastinal shift: Usually >1,000 mL
- Decreased or inaudible breath sounds
- Tachypnea
- Egophony, pleural friction rub
- Asymmetric expansion of thoracic cage
- Dullness to percussion
- Decreased or absent tactile fremitus
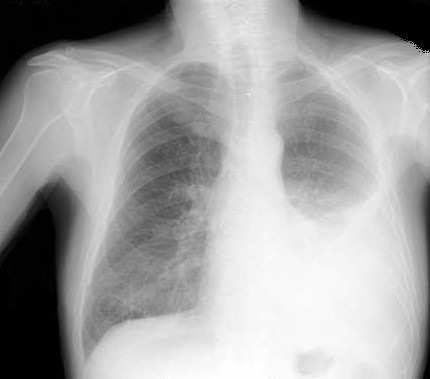
Etiology of Pleural Effusion
Transudative effusion
- Cirrhosis (hepatic hydrothorax): 2/3 right side
- Nephrotic syndrome, hypoalbuminemia
- Transudates are largely due to imbalances in hydrostatic and oncotic pressures in the chest.
- is seen in left ventricular failure, pulmonary embolism, cirrhosis.
- CHF: 80% bilateral
- Constrictive pericarditis
- Urinothorax, central line misplacement
- Atelectasis
- Peritoneal dialysis
- Trapped lung, peritoneal dialysis
- Myxedema, superior vena cava obstruction
Exudative pleural effusion
- is found in bacterial pneumonia. mali nanc viral infection, pulmonary embolism.
- In exudative pleural effusion
- The ratio of pleural fluid protein / serum protein is more than 0.5.
- The ratio of pleural fluid LDH / serum LDH is more than 0.6.
- The pleural fluid LDH is more than 2/3rd of serum LDH.
- GI: Pancreatitis, esophageal rupture, abdominal abscess, after liver transplant
- Chylothorax: Thoracic duct tear, malignancy
- With these criteria, 25% of transudates may be misdiagnosed as exudates. So, if the clinical diagnosis is-. transudative nature of the fluid, the difference between albumin levels in the seum and the pleural fluid is measured. If this difference is more than 1.2g/dl, then the fluid is a transudate.
- Lung parenchyma infection, bacterial: parapneumonic, tuberculous pleurisy, fungal, viral
- Disease in virtually any organ can cause exudative pleural effusions by a variety of mechanisms, including infection, malignancy, immunologic responses,
- Parasitic (amebiasis, Echinococcus)
- Malignancy: Lung cancer, metastases (breast, lymphoma, ovaries), mesothelioma
- PE
- Collagen-vascular disease: Rheumatoid arthritis, systemic lupus erythematosus (SLE), Wegener granulomatosis, sarcoidosis
- Hemothorax: Trauma, PE, malignancy, coagulopathy, aortic aneurysm
Pleural Effusion Pathophysiology
- The normal pleural space contains ~1 mL of fluid.
- Trasudates result from imbalances in hydrostatic and oncotic forces.
- Increase hydrostatic and/or low oncotic pressures
- Increase in pleural capillary permeability
- Pleural fluid accumulates when pleural fluid formation exceeds pleural fluid absorption.
- Lymphatic obstruction or impaired drainage
- Movement of fluid from the peritoneal or retroperitoneal space
- Iatrogenic causes
- decortication pleural effusion
Two-test rule of Pleural Effusion
- – Pleural fluid cholesterol greater than 45 mg/dL – Pleural fluid LDH greater than 0.45 times the upper limit of the laboratory’s normal serum LDH Three-test rule
- – Pleural fluid protein greater than 2.9 g/dL – Pleural fluid cholesterol greater than 45 mg/dL – Pleural fluid LDH greater than 0.45 times the upper limit of the laboratory’s normal serum LDH
The pleural fluid is examined for:
- Colour and thickness of fluid.
- Glucose
- Cell count and type
- Microbiology
- Cytology.
- Amylase in pleural fluid is elevated in esophageal rupture, pancreatic disease and malignancy.
- Glucose is less than 60 mg/dl in malignancy, bacterial infections, rheumatoid disease.
Causes of pleural effusion Transudative
- CHF
- Cirrhosis
- Nephrotic syndrome
- Myxodema
- Superior vena cava obstruction
- Pulmonary embolism.
Causes of pleural effusion Exudative
- Infections – Tuberculosis, bacterial, fungal, viral, parasitic
- Neoplastic diseases
- Mesothelioma (primary tumor of pleura) Pulmonary embolism
- Collagen vascular diseases .
- Intraabdominal abscess Esophageal perforation Pancreatic disease Sarcoidosis
- Uraemia
- Asbestosis
- Radiation
- Pericardial diseases Chylothorax
- Nitrofurantoin and amiodarone induced.
Effusion due to heart failure
- · Pleural effusion can occur in LVF
- · Treated with diuretics.
Hepatic causes
- In cirrhosis and ascites usually right-sided pleural effusion may occur.
- Treatment is liver transplant or transjugular intrahepatic portal systemic shunt (TIPS).
Para pneumonic effusion
- In bacterial pneumonia, lung abscess, bronchiectasis, exudative pleural effusion, or even purulent effusion (pus.in the pleural cavity), called empyemais seen.
- Treatment is thoracentesis.
- More invasive methods of removal of fluid or pus is required ifthere is loculated effusion, or gross pus in pleural space.
- Tube thoracostomy is done for recurrent effusions and where the prognosis is poor.
Tubercular pleuritis
- Tuberculosis is the most common cause of pleural effusion in the developing countries. It is due to hypersensitivity reaction to tuberculous protein in the pleural space.
- Symptoms are fever, weight loss, dyspnoea, pleuritic chest pain.
- Pleural fluid has small Iymphocytes, adenosine deaminase in the pleural fluid is more than 45 lUlL, peR for tuberculous DNA is positive.
- Treatment is pleural aspiration and antitubercular arugs.
Treatment of Pleural Effusion
First Line Pleural Effusion treatment
- Treat underlying cause:
- CHF: Diuretics (75% clearing in 48 h)
- Parapneumonic effusion: Antibiotics
- Steroids and nonsteroidal anti-inflammatory drugs (NSAIDs) for rheumatologic and inflammatory causes
Second Line Pleural Effusion treatment
- Symptomatic nonmalignant pleural effusions that are refractory to primary treatment may be managed with repeated therapeutic thoracentesis or pleurodesis.
