Article Contents ::
- 1 Hepatitis PROPHYLAXIS and Hepatitis TREATMENT and Management
- 2 Hepatitis PROPHYLAXIS
- 3 Hepatitis A prophylaxis
- 4 Hepatitis B prophylaxis
- 5 Hepatitis D prophylaxis
- 6 Hepatitis C prophylaxis
- 7 Hepatitis E prophylaxis
- 8 PROGNOSIS of Hepatitis
- 9 COMPLICATIONS AND SEQUELAE of Hepatitis
- 10 Hepatitis TREATMENT
- 11 Treatment of Acute Attack of Hepatitis
- 12 MANAGEMENT OF FULMINANT HEPATITIS
- 13 Hepatitis TREATMENT Contraindications:
- 14 Complementary & Alternative Hepatitis Therapies
Hepatitis PROPHYLAXIS and Hepatitis TREATMENT and Management
Hepatitis PROPHYLAXIS
- Prevention is through immunization
Hepatitis A prophylaxis
- Passive immunization with IG
- Active immunization with killed vaccines
- 1. Passive immunization is given before exposure or during early incubation period.
- 2. Post exposure prophylaxis – 0.02 ml/kg IgG is given after exposure as soon as possible. It is effective up to 2 weeks after exposure.
- 3. If a person is traveling to developing countries 0.02 ml/kg IgG is given.
- 4. For more than 3 months- 0.6 ml/kg is given every 4 months.
- 5. Vaccines of HAV are safe and effective and protection lasts about 20 yrs.
Hepatitis B prophylaxis
- 1. Passive immunoprophylaxis with IgG – hepatitis B immune globulin.
- 2. Active immunization with recombinant vaccine
- 3. For pre-exposure prophylaxis 3 intramuscular deltoid injections of hepatitis B vaccine are given at 0, 1 and 6 months. The injection is not given in the gluteal region. All the children up to the age of 18 yrs m ust be vaccinated.
- 4. All the persons at risk of exposure to blood must be vaccinated.
- To recombinant hepatitis B vaccines are:
- 1. Recombivax HB – 10 ~gm of HBsAg
- 2. Engerix B – 20 ~gm of HBsAg
- Protection after vaccination is for approximately 10 years.
Hepatitis D prophylaxis
- Hepatitis D is prevented by vaccination with hepatitis . B vaccine.
Hepatitis C prophylaxis
- IG is ineffective.
- Hepatitis C is prevented by :
- 1. Screening of all blood donors.
- 2. Avoid contact with infected persons’ secretions and blood .
- . 3. Hepatitis C patients should not share toothbrushes, nail clippers, razors.
Hepatitis E prophylaxis
- Recombinant vaccine is under trial.
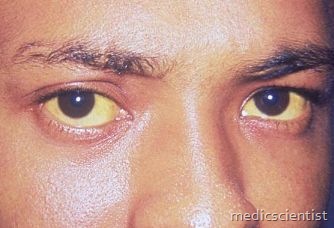
PROGNOSIS of Hepatitis
- Hepatitis A patients recovers completely.
- In hepatitis B healthy adults recovery completely. In hepatitis B prognosis is bad if :
- · Patient is aged
- · Patient has ascites
- · Peripheral edema
- · Hepatic encephalopathy
- · Prolonged PT
- · Low serum albumin
- · Hypoglycemia
- · High serum bilirubin
- Such patients must be hospitalized. Hepatitis C is less severe than hepatitis B.
- In patients of hepatitis Band D mortality is higher than other types of hepatitis.
COMPLICATIONS AND SEQUELAE of Hepatitis
- In hepatitis A there may be a relapse after weeks or months.
- In hepatitis A there may be cholestatic hepatitis. But hepatitis A is self-limited.
- In hepatitis B there may be a serum sickness like syndrome with arthralgia high fever, rash, angioedema, proteinuria, hematuria. ALT and AST are elevated. Serum HBsAg is positive.
- In hepatitis C there may be porphyria cutanea and lichen planus.
- Most serious complication of viral hepatitis is fulminant hepatitis or massive hepatic necrosis. It is seen in hepatitis B, D and E, Most common in hepatitis B and rarest in hepatitis E.
- Fulminant hepatitis is common in pregnancy.
- In fulminant hepatitis there is encephalopathy, confusion, disorientation, somnolence, ascites, edema, cerebral edema, GI bleeding, sepsis, respiratory failure, altered consciousness, small liver, increased PT, increased bilirubin level, (but SGOT, SGPT may fall), cardiovascular collapse, renal failure and death. When patients go into deep coma, mortality is very high.
- Liver transplant may be life saving in fulminant hepatitis.
- 10% of patients remain positive for HBsAg for more than 6 months after acute hepatitis B. 50% of these become HBsAg negative in some years.
- Acute hepatitis B leads to chronic hepatitis and there is persistent anorexia, weight loss, fatigue, hepatomegaly, bridging hepatic necrosis, high bilirubin and SGPT levels more than 6 months and upto 1 year.
- Rare complications are pancreatitis, myocarditis, aplastic anaemia, transverse myelitis, peripheral neuropathy, hepatocellular carcinoma.
- Hepatitis Band C is common in HIV patients.
Hepatitis TREATMENT
Treatment of Acute Attack of Hepatitis
- In hepatitis B, if patient was healthy before acute hepatitis, recovery occurs in 99% persons.
- No antiviral therapy required.
- Some physicians like to give in acute hepatitis B, Lamivudine 100 mg/day oral.
- In hepatitis C recovery usually does not occur and it progresses to chronic hepatitis.
- In such cases antiviral therapy with interferon alpha 5 million units subcutaneous daily for 4 weeks then 3 times a week for another 20 weeks· results in nearly 100% response.
- For chronic hepatitis C long acting pegylated interferon plus Ribavirin is given.
- Patients with chronic hepatitis C are rare.
- In health workers who get hepatitis C due to contaminated needles therapy should be started immediately.
- Most patients of acute hepatitis do not require hospital admission. Physical activity should be restricted.
- High calorie diet is given especially in the morning.
- If patient has vomiting, IV fluids are given for severe itching (pruritus), Cholestyramine the bile salt binding resin is given.
- Steroids (glucocorticocoid) should not be given. Isolation of patient is not required except if :
- 1. Patients have fecal incontinence
- 2. Severe bleeding in hepatitis Band
- 3. Hepatitis C patients with bleeding.
- Gloves should be used by all those handling stools of hepatitis patients.
- Gloves should be used for people handling blood and body fluids of hepatitis Band C patients.
- Hands should be washed thoroughly when nursing hepatitis patients.
- Patients’ are discharged from hospital when:
- 1. There is symptomatic relief
- 2. Serum aminotransferase (AST and ALT) falls down ‘
- 3. Serum bilirubin falls down
- 4. Prothrombin time returns to normal.
MANAGEMENT OF FULMINANT HEPATITIS
- 1. Maintain fluid balance
- 2. Support of circulation
- 3. Support of respiration
- 4. Control of bleeding
- 5. Treat hypoglycemia
- 6. Management of comatose patient
- 7. Diet – protein restriction, plenty of carbohydrates
- 8. Oral lactulose or neomycin
- 9. Therapies like sterOid, exchange transfusion,
- plasmapharesis are not effective.
- 10. Liver assist devices are under trial
- 11. Intensive care management
- 12. Liver transplantation gives excellent results.
Hepatitis TREATMENT Contraindications:
- Mouse IG, egg, or neomycin allergy
- Pregnancy/breast-feeding
- Decompensated liver disease
- Renal failure
- Untreated psychiatric disease
- Corticosteroid use
- Uncontrolled autoimmune disease
- DDI in HIV patients (substitute comparable agent)
- •Precautions:
- Disorders of coagulation
- Seizures
- Anemia, myelosuppression
- Depression/suicidal ideation; psychiatric clearance and monitoring recommended
- Retinopathy (diabetic/hypertensive). Needs ophthalmology clearance and monitoring
Complementary & Alternative Hepatitis Therapies
- No medical evidence exists for using herbal or alternative therapy in HCV/cirrhosis/HCC
- Milk thistle (silymarin) generally safe and may reduce ALT but does not eradicate virus nor improve outcomes; avoid while on IFN.
- Rate of HCC tripled in patients on herbal therapy compared to IFN therapy
