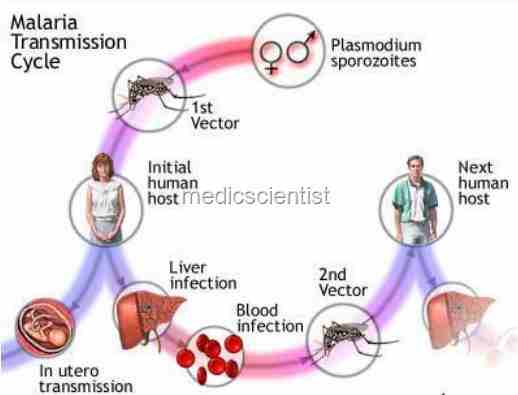
FALCIPARUM MALARIA
- Pregnant women have an increased susceptibility to malaria infection.
- Malarial infection of the placenta by sequestration of the infected red blood cells leading to low birth weight and other effects.
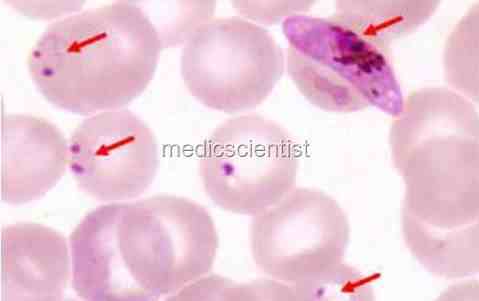 |
| FALCIPARUM Malaria fever |
- There are four types of malaria caused by the protozoan parasite
- This fulminant disease often produces coma, shock, or sudden death.
- Falciparum malaria in which the brain is affected.
- Vital organ dysfunction may occur. Parasitemia may be — 3%.
- Mortality may be high in severe falciparum malaria.
Cerebral malaria
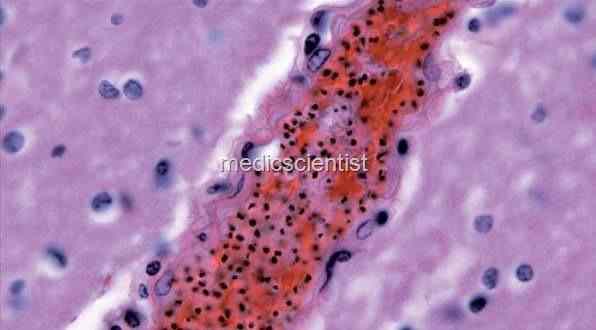 |
| Cerebral malaria |
- It is a serious form of falciparum malaria.
- There is coma with increased mortality despite treatment.
- Obtundation i.e. altered consciousness, delirium, abnormal behaviour occur.
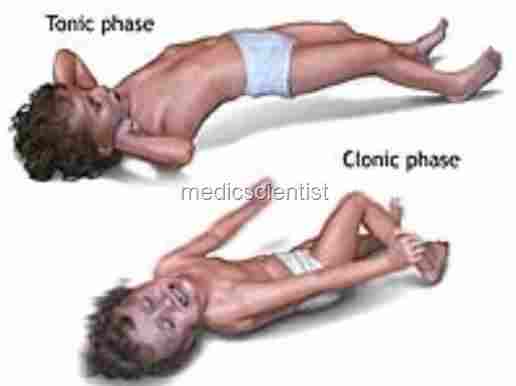
- Onset may be gradual or sudden. There may be convulsions.
- There is a diffuse symmetric encephalopathy.
- Focal neurologic signs and signs of meningeal irritation are absent.
- Corneal reflexes are preserved. Tendon reflexes are variable.
- Plantar reflexes may be flexor or extensor. Abdominal reflexes are absent.
- Fundus may show retinal haemorrhages, papilloedema.
- There may be residual neurologic deficit, blindness, deafness.
Hypoglycemia in malaria
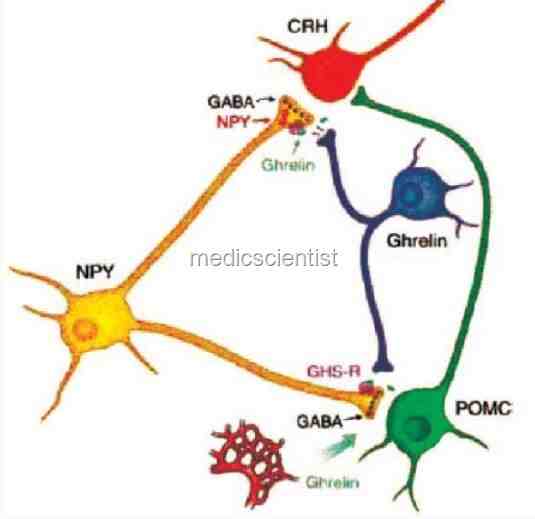 |
| Hypoglycemia in malaria |
- Common in children and pregnant women.
- It is due to failure of hepatic gluconeogenesis. Quinine, used to treat malaria may cause increased pancreatic insulin secretion leading to hypoglycemia.
- There is sweating, tachycardia.
Lactic acidosis in malaria
- It may occur in severe malaria. There is lactic acidosis with ketoacidosis, respiratory distress, circulatory failure, with poor prognosis.
Non cardiogenic pulmonary edema
- May occur in falciparum malaria or vivax malaria. Mortality is 80%.
Renal impairment in malaria
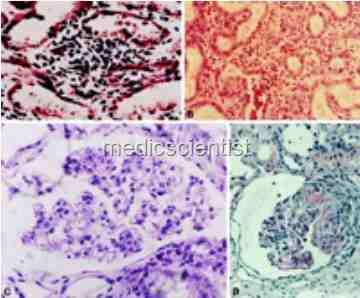 |
| Renal impairment in malaria |
- May occur in falciparum malaria in adults.
- It is due to erythrocyte sequestration, and acute tubular necrosis leading to ARF.
- Treatment is early dialysis.
Hematologic abnormalities in malaria
- There is anaemia, coagulation abnormalities, thrombocytopenia with bleeding.
- There may be disseminated intravascular coagulation (DIe).
Liver dysfunction in malaria Hemolytic jaundice
 |
| Liver dysfunction in malaria Hemolytic jaundice |
- Hepatic dysfunction
- Mild or deep jaundice
- Severe liver dysfunction occurs in falciparum malaria.
MALARIA IN PREGNANCY
 |
| MALARIA IN PREGNANCY |
- Associated with low birth weight, increased mortality, congenital malarial infection in children.
- In the pregnant mother, there is severe anaemia, hypoglycemia, acute pulmonary edema, premature labour.
MALARIA IN CHILDREN
- Convulsions, coma, hypoglycemia, severe anaemia is more common in children.
TRANSFUSION MALARIA
- Malaria can occur by blood transfusion, needle-prick, as in drug addicts, organ transplantation.
ALGID MALARIA
 |
| ALGID MALARIA |
- Algid malaria may be due to adrenal crisis, absorption of endotoxin from gut or TNF (tumor necrosis factor) from endotoxin-activated macrophages.
- There is sub-normal temperature, weakness, prostration, feeling of cold, vomiting, loose motions, rapid respiration and oliguria.
- Death may occur but patient is conscious till the end.
BLACK WATER FEVER
- After several bouts of falciparum malaria, there is occasionally abrupt onset of massive intravascular hemolysis with fever, chills and prostration.
- It is the result of red blood cell destruction and the release of hemoglobin.
- Bloody urine (hemoglobinuria) that occurs as a complication of falciparum malaria infection.
- It occurs most commonly in patients who have been treated with drugs derived from quinine.
- Hemoglobin escapes in urine turning it black, if the urine is acidic.
- The illness is marked by high fevers, dark urine, epigastric pain, vomiting, jaundice, and shock
- This is a serious condition with a bad prognosis.
Patient Care ––
- In such areas, suppressive and prophylactic drugs may be needed to control the disease.
- Health care providers in endemic areas need to work toward prompt detection and effective treatment of malaria.
