Definition of Toxoplasmosis (Toxoplasma Infection)-
Toxoplasmosis is caused by a parasite called Toxoplasma gondii. Description of Toxoplasmosis. The parasite Toxoplasma gondii multiplies in the intestine of the cat and is shed in cat feces, mainly into litter boxes and garden soil. Infection with the protozoan Toxoplasma gondii.
- Approx. 25% of women who become infected for the first time during pregnancy pass the infection on to the developing fetus.
- It usually is a recurrence of a mild infection that is subclinical in persons with normal immune systems;
- approx. 30% of the U.S. population have antibodies indicating they have been infected.
- Patients who receiving immunosuppressive therapy after an organ transplant, reactivation of dormant organisms may be fatal.
- In persons with acquired immunodeficiency syndrome (AIDS)
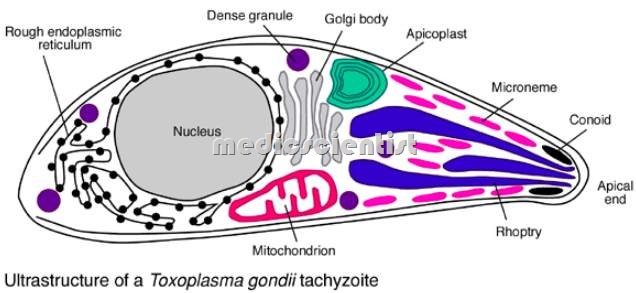
Etiology of Toxoplasmosis
- · Toxoplasma infection is due to intracellular coccidian parasite Toxoplasma gondii.
- Toxoplasmosis is diagnosed by clinical presentation, brain biopsy, brain scans, and response to treatment.
- · Acute infection just after birth may be asymptomatic but the cysts persist within the tissues.
- In 25% of fetuses, toxoplasmosis damages the heart, brain, and lungs.
- In immunosuppressed patients, the infection causes reactivation of latent infection in the transplanted organ.
- It also causes eye infection (chorioretinitis), which may produce blindness.
- In people with AIDS, toxoplasmosis is the most common cause of encephalitis; systemic disease also may occur.
- · The parasite can lead to acute and chronic toxoplasmosis which presents with lymphadenopathy, encephalitis, myocarditis and pneumonitis.
- · Congenital toxoplasmosis is due to transplacental passage of parasite from mother to fetus.
- · The infants are asymptomatic at birth but later develop chorioretinitis, strabismus or squint, epilepsy, mental retardation.
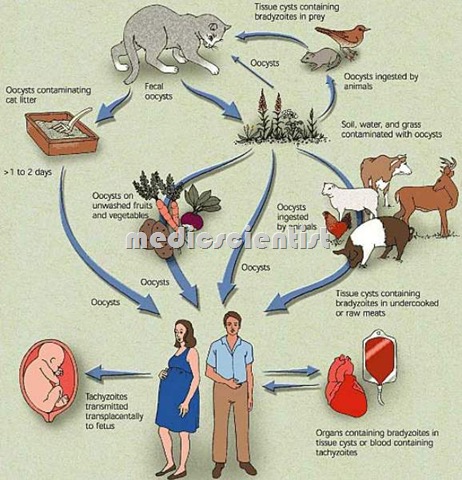
Transmission of Toxoplasma Infection
- · The oocysts of the parasite are taken orally by the host from the soil or uncooked meat.
- The sporozoites in the cysts are very infectious and remain alive for many years in the soil.
- Even a single cyst ingested can cause human infection.
- · In addition to oral transmission, the parasite can enter the body by blood transfusion or organ transplantation.
- · The infection is also transmitted to the fetus from a pregnant mother with the infection.
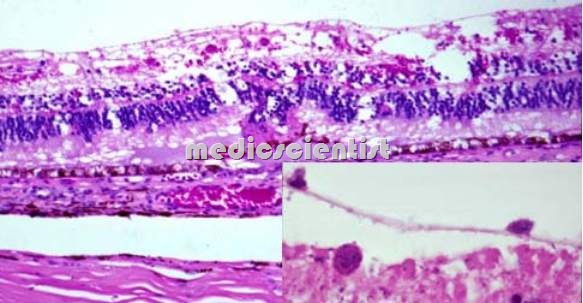
Pathogenesis of Toxoplasma Infection
- · The oocysts which are ingested travel to the GIT and may be disseminated to many organs like lymphatic tissue, skeletal muscle, myocardium, retina, placenta and the CNS.
- · The parasites replicate and invade more and more cells and tissues causing cell death and necrosis.
- · The cysts persist and may rupture in any organ including the CNS.
- · It can lead to organ failure like necrotizing encephalitis, pneumonia, myocarditis.
- · The disease is found in lymph nodes, eyes, CNS, lungs, heart, GIT and other sites like skeletal muscle, pancreas, stomach and kidneys.
Toxoplasma Infection Clinical Manifestations
- · In healthy persons, the acute infection may be asymptomatic and self-limited.
- · The diagnosis is difficult in mothers during pregnancy.
- It leads to congenitally infected children with severe neurological features like hydrocephalus, microcephaly, mental retardation, and chorioretinitis.
|
- · Multi-organ failure and subsequent intrauterine fetal death can occur.
- · There is cervical lymphadenopathy. The lymph node may be single or multiple, discrete, firm and may be generalized or suboccipital, supraclavicular, inguinal, or mediastinal.
- · There is headache, malaise, fatigue, fever, sore throat, myalgia, abdominal pain, meningoencephalitis, pneumonia, myocarditis, pericarditis, polymyositis, seizures, cranial nerve palsies, motor deficits, ataxia, DIC, hypotension, necrotizing retinitis, iridocyclitis, cataracts, glaucoma, chorioretinitis.
Diagnosis of Toxoplasma Infection
- · Serologic testing
- · Appropriate culture
- · PCR (polymerase chain reaction)
- · CT
- · MRI
- · HIV testing
- · IgM -Positive IgM titre indicates acute infection
- · Increased IgG titre but normal IgM titre suggests chronic infection
- · Biopsy – histopathology of affected tissues.
Toxoplasma Infection Treatment
- For congenital toxoplasmosis in neonates, oral pyrimethamine 1 mgjkg and sulphadiazine 100 mgjkg for 1 year.
- A combination of pyrimethamine, sulfadiazine, and leucovorin (folinic acid) is administered until 2 weeks after symptoms disappear; the latter helps prevent bone marrow depression.
- Prednisone is added to the regimen, for patients with toxoplasma meningitis or chorioretinitis.
- Patients with AIDS should be treated for acute toxoplasmosis. If CD4 T lymphocyte count is less than 100 jl-lL, prophylaxis against toxoplasmosis must be given.
- Trimethoprim plus Sulphamethoxazole is given for Pneumocystis carinii infection.
- Other drugs are Atovaquone, Dapsone, and Azithromycin.
- Treatment can be discontinued in patients when the CD4 count is more than 200 /I-IL for 3 months.
- Hand should be wash thoroughly after working in the garden.
- Fruits and vegetables should be cleaned thoroughly so that there is no soil on it.
- Seronegative women should be screened for infection during pregnancy several times.
- HIV positive patients must be given HAART (highly active antiretroviral therapy) and prophylaxis for Toxoplasma.
Prevention of Toxoplasma infections
- Avoid eating undercooked meat.
