Article Contents ::
- 1 Toxic Hepatitis and Drug Induced Hepatitis Diagnosis and Treatment
- 2 Toxic Hepatitis and Drug Induced Hepatitis
- 3 Acute liver injury —
- 4 Drug Induced Hepatitis DIAGNOSIS —
- 5 Classification of liver test abnormalities
- 6 Types of drug-induced liver injury —
- 7 Extrahepatic manifestations —
- 8 Toxic Hepatitis and Drug Induced Hepatitis Treatment
Toxic Hepatitis and Drug Induced Hepatitis Diagnosis and Treatment
Toxic Hepatitis and Drug Induced Hepatitis
- Injury to liver may occur due to drugs and toxins inhaled, eaten, chewed, or swallowed.
- The metabolism of drugs by the liver and the mechanisms by which drugs might injure the liver are discussed separately
- Drug-induced liver injury (also called DILI or drug-induced hepatotoxicity) is a common problem
- It is the most common cause of acute liver failure in the United States, and is the most frequently cited reason for withdrawal of medications from the marketplace
- An inflammation of the liver caused by the entry of toxins or drugs into the body. Included in the great number of agents known to be able to cause this type of hepatitis are common drugs and chemicals
- It is seen in up to 30 percent of patients who present with acute hepatitis and represents up to 10 percent of consultations by hepatologists, and about 1 percent of all general medical admissions
- The annual incidence is generally felt to be between one in 10,000 to 100,000; however, incidences as high as 14 per 100,000 population have been reported
- It accounts for up to 10 percent of all adverse drug reactions
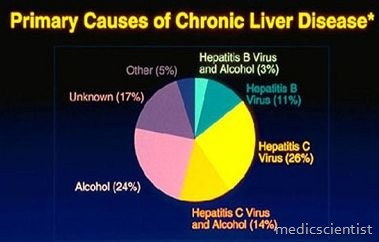
Acute liver injury —
- Acute DILI is the most common form of liver damage caused by drugs.
Drug Induced Hepatitis DIAGNOSIS —
- The diagnosis of DILI can be difficult. The relationship between exposure to the drug and hepatic toxicity is not always clear.
- There is no specific serum biomarker or characteristic histologic feature that reliably identifies a drug as the cause of toxicity
- Exposure must precede the onset of liver injury (although the latent period is highly variable)
- Underlying liver disease should be sought Injury may improve when the drug is stopped (although in some cases injury may initially worsen for days or weeks while in fulminant cases, declining liver biochemical tests may indicate deterioration rather than improvement)
- Liver injury may have recurred more rapidly and severely after repeated exposure.
Classification of liver test abnormalities
- Hepatitis (hepatocellular) ALT 3 x ULN R 5
- Cholestasis ALT 2 x ULN R 2
- Mixed ALT 3 x ULN ALP 2 x ULN R >2 to <5
Types of drug-induced liver injury —
| Acute liver injury –Hepatocellular Acarbose Acetaminophen Allopurinol Aspirin Buproprion Bromfenac Diclofenac Ethanol Fluoxetine Halothane Isoniazid Ketoconazole Lisinopril Losartan Methyl-dopa Nefazodone Nevirapine Paroxetine Phenytoin Pyrazinamide Rifampin Risperidone Ritonavir Sertraline Statins Tetracycline Trazodone Thiazolidinediones Trovafloxacin Valproate Cholestasis ACE inhibitors Amoxicillin/Clavulanate Anabolic Steroids Azathioprine Chlorpromazine Clopidogrel Cytarabine Erythromycins Estrogens Ethanol Irbesartan Phenothiazines Sulindac Terbinafine Tricyclics Mixed Amitryptilline Azathioprine Captopril Carbamazepine Clindamycin Cyproheptadine Enalapril Flutamide Ibuprofen Nitrofurantoin Phenobarbital Phenothiazines Phenytoin Sulfonamides Trazodone Sulfonamides Verapamil | Chronic liver injury –Steatohepatitis Amiodarone Ethanol Tamoxifen Valproic Acid Microvesicular steatosis Ethanol Methotrexate NRTIs Tetracycline Valproic acid Granulomatous hepatitis Allopurinol Carbamazepine Diltiazem Hydralazine Penicillamine Phenytoin Procainamide Quinidine Rosiglitazone Sulfonamides Sinusoidal obstruction syndrome Busulfan Cyclophosphamide Imuran Fibrosis Ethanol Methotrexate Methyldopa Peliosis hepatis Anabolic steroids Vinyl chloride Autoimmune hepatitis Nitrofurantoin Minocycline Statins Chronic hepatitis Diclofenac Methyldopa Minocycline Nitrofurantoin Trazodone Neoplasm Anabolic steroids Oral contraceptives Vinyl chloride Ischemic necrosis Ergot |
- Cholestasis :
- May be caused by anabolic steroids, erythromycin, rifampicin, amoxycilin-clavulanic acid, oral contraceptives, chlorpromazine, cyclosporine, carbamazepine, nifedipine, verapamil.
- Fatty liver :
- Fatty liver may be caused by tetracycline, sodium valproate, amiodarone, zidovudine, indinavir, Methotrexate.
- Hepatitis :
- May be caused by halothane, phenytoin, carbamazepine’, isoniazid, rifampicin, chlorthiazide, amitriptyline, venlafaxine, ibuprofen, indomethacin, diclofenac, ketoconazole, fluconazole, zidovudine, methyldopa, captopril, enalapril, nifedipine, verapamil, diltiazem.
- Toxic necrosis :
- is caused by yellow phosphorous, paracetamol.
- Granulomas :
- are caused by sulphonamide, allopurinol, quinidine, diltiazem, carbamazepine.
Extrahepatic manifestations —
- Some drugs causing liver injury may be associated with clinical features
- Serologic markers of autoimmunity may be seen in patients with toxicity related to procainamide
- Toxicity to multiple organs (eg, bone marrow, kidney, lung, skin and vessels) may be seen with some drugs (eg, chlorpromazine, amoxicillin-clavulanate, erythromycin, and sulindac).
- Drugs causing hypersensitivity reactions (eg, penicillin and procainamide) may be associated with fever, rash, and peripheral eosinophilia.
- Some drugs (eg, dapsone, phenytoin, sulfonamides) may be associated with a mononucleosis-like illness (pseudomononucleosis)
Toxic Hepatitis and Drug Induced Hepatitis Treatment
- Treatment is supportive.
- The drug should be withdrawn and glucocorticoids given.
- Paracetamol poisoning is treated with gastric lavage and N-acetyl cystine which reduces hepatic necrosis, if therapy is started within 8 hours of ingestion.
- The main treatment for DILI is withdrawal of the offending drug
