Article Contents ::
Hemolytic Anaemias Classification Diagnosis And Treatment
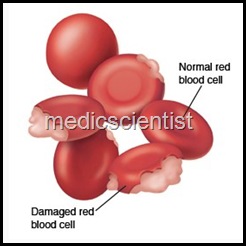 |
| Hemolytic Anaemia |
- The loss of red cells by hemolysis or destruction are main causes hemolytic anaemia. The life span of RBCs is 90 to 120 days in circulation.
- The destroyed RBCs are replaced by new red cells formed by the bone marrow. If the rate of destruction of RBCs is more than the rate of replenishment, then anaemia occurs.
- There is jaundice due to rise in bilirubin generated by destruction of RBCs. There are symptoms of anaemia like fatigue and dyspnoea.
 |
| Hemolytic Anaemia jaundice |
- There is passage of red brown urine (hemoglobinuria).
- There is history of exposure to drugs or toxins. Usually there is splenomegaly.
Lab tests
- There is evidence of hemolysis on examination of blood smears.
- Reticulocyte count is elevated due to erythroid hyperplasia of the bone marrow.
- Reticulocytes are also elevated in patients with blood loss, myelophthisis, decrease of red blood cells in circulation due to any cause.
Red blood cell morphology IS altered as follows
- · Spherocytes in hereditary spherocytosis.
- · Target cells in hemoglobin disorders thalassemias, hemoglobin Sand C.
- · Schistocytes in microangiopathy, intravascular prosthesis.
- · Sickle cells in sickle cell syndromes.
- · Acanthocytes and spur cells in severe liver disease.
- · Agglutinated cells in cold agglutinin disease.
- · Heinz bodies in oxidant stress.
Classification of hemolytic anaemias
- Hemolytic anaemia may be due to intracorpuscular defect or extracorpuscular factors.
- The intracorpuscular (defect is within the RBC) causes are enzyme defects, hemoglobinopathies, hereditary spherocytosis.
- The extracorpuscular factors are liver disease – spur cell .anaemia, hypersplenism, immune complexes, infections, toxins, microangiopathy.
Treatment of Hemolytic Anaemia
- Splenectomy reduces the hemolysis and improves RBC survival.
- Splenectomy is done by laparoscopy for low risk. Folic acid 1 mgjday is given before splenectomy.
HEMOLYTIC ANAEMIA DUE TO DEFECTS IN HEXOSE – MONOPHOSPHATE SHUNT
- When RBC’s are exposed to a drug or toxin which generates free radicals, then glucose metabolism via hexose monophosphate shunt starts to occur. This protects the RBC membrane from oxidation and destruction.
- In G6PD deficiency the hexose monophosphate shunt becomes defective and hemoglobin precipitates within the RBC forming Heinz bodies.
- There is no treatment but the disease is self remitting.
- Oxidant drugs, infections, and Fava beans should be avoided.
- Drugs causing hemolysis in G6PD deficiency patientsPrimaquine, Sulphonamides, Nitrofurantoin, Nalidixic aCid, Furazolidone, Vitamin K, dapsone, doxorubicin etc.
